Back
BackMicrobiology Study Guide: Infectious Disease, Epidemiology, Host-Microbe Interactions, and Immunity
Study Guide - Smart Notes

Disease Terminology and Epidemiology
Basic Principles of Infectious Disease and Epidemiology
Understanding infectious disease and epidemiology is fundamental in microbiology. Infectious diseases are caused by pathogens, and epidemiology involves monitoring and controlling disease occurrence to promote public health.
Pathogens: Include prions, viruses, bacteria, protozoans, helminths, and fungi.
Opportunistic pathogens: Cause disease only when the host is weakened.
True pathogens: Cause disease in healthy hosts.
Sporadic: Isolated cases in a population.
Endemic: Routinely detected in a population or region.
Epidemic: Widespread outbreak in a region.
Pandemic: Epidemic that spreads to multiple countries.
Zoonotic diseases: Spread from animals to humans.
Communicable diseases: Transmit from human to human.
Contagious diseases: Easily transmitted between hosts.
Signs: Objective indicators (e.g., fever, rash).
Symptoms: Subjective feelings (e.g., pain, fatigue).
Latent infection: Asymptomatic phase.
Acute disease: Rapid onset and progression.
Chronic disease: Slow onset and progression.
Koch’s Postulates
Koch’s postulates are a set of criteria used to establish the causative relationship between a microbe and a disease.
The same organism must be present in every case of the disease.
The organism must be isolated and grown in pure culture.
The cultured organism should cause disease in a susceptible host.
The organism must be re-isolated from the inoculated host.
Limitations include inability to apply to noninfectious diseases, obligate intracellular pathogens, and latent diseases.
Reservoirs and Sources of Infection
Pathogens originate from various sources, some of which are reservoirs. Reservoirs are habitats where pathogens are naturally found, while sources disseminate pathogens to new hosts.
Endogenous source: Pathogen from the host’s own body.
Exogenous source: Pathogen external to the host.
Modes of Transmission
Pathogens can be transmitted through direct or indirect contact, airborne particles, vehicles (contaminated objects, food, water), and vectors (biological or mechanical).
Stages of Infectious Disease
Five General Stages of Disease
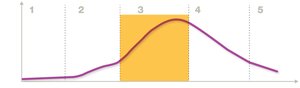
Infections progress through five stages: incubation, prodromal, acute, period of decline, and convalescent phase. Infectivity, pathogenicity, and virulence are key concepts describing a pathogen’s ability to establish infection and cause disease.
Incubation period: Time between infection and earliest symptoms.
Prodromal phase: Early symptoms develop.
Acute phase: Peak of disease.
Period of decline: Symptoms start to resolve.
Convalescent phase: Recovery; pathogen may remain latent.
Epidemiology Essentials
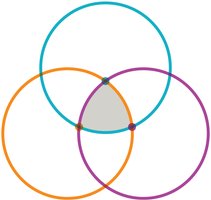
The Epidemiological Triangle
The epidemiological triangle links the host, etiological agent, and environment. Disease results from the interaction of these three factors.
Host factors: General health, sex, lifestyle, age, ethnicity, occupation.
Etiological agent: Fungi, bacteria, virus, parasite, or prion.
Environmental factors: Climate, geography, vectors, water, food sources.
Public Health Strategies
Strategies to break the epidemiological triangle include public education, quarantine, and vector control.
Host–Microbe Interactions and Pathogenesis
Normal Microbiota and Pathogens
Host–microbe interactions are dynamic. Normal microbiota colonize various body sites and usually do not cause disease unless disrupted (dysbiosis). Pathogens have adaptations for interacting with host tissues.
Virulence Factors
Virulence factors are mechanisms pathogens use to overcome host defenses, such as adhesion, invasion, immune evasion, and nutrient acquisition.
Pathogenicity: Ability to cause disease.
Virulence: Degree of disease caused.
Virulence factors: Features aiding in adherence, invasion, immune evasion, and nutrient acquisition.

Attenuation
Attenuated pathogens are infectious but weakened, often used in vaccines.
Toxins as Virulence Factors
Toxins are molecules that cause tissue damage and suppress immune responses. Toxigenic microbes produce toxins, and toxemia refers to toxins in the bloodstream.
Endotoxins: Part of Gram-negative cell wall; released upon cell death.
Exotoxins: Soluble proteins affecting various cell types; produced by both Gram-positive and Gram-negative bacteria.
Steps to Infection
Five Steps to Infection
To establish infection, pathogens must:
Enter the host
Adhere to host tissues
Invade tissues and obtain nutrients
Replicate while evading immune defenses
Transmit to a new host
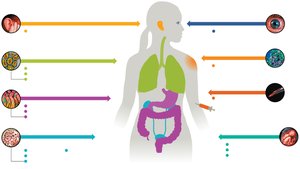
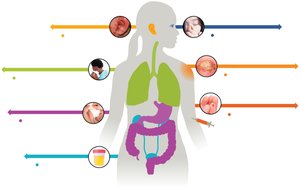
Portals of Entry
Pathogens enter hosts through specific portals, including respiratory mucosa, skin, ocular, transplacental, parenteral, urogenital, GI mucosa, and otic routes.
Portals of Exit
Pathogens exit hosts via feces, urine, blood, wound drainage, saliva, mucus, semen, etc. The portal of entry is often the same as the portal of exit.
Immune System and Host Defense
Innate and Adaptive Immunity
The immune system has two main branches: innate and adaptive immunity. Both recognize pathogens, eliminate invaders, and distinguish self from foreign antigens.
Innate immunity: Inborn, nonspecific, rapid response.
Adaptive immunity: Specific, develops over time, exhibits memory.
First-Line Defenses
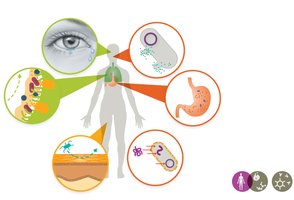
First-line defenses prevent pathogen entry and include mechanical, chemical, and physical barriers.
Mechanical barriers: Flushing, rinsing, trapping (e.g., tears, urine, saliva, mucus).
Chemical barriers: Molecules that attack microbes or create hostile environments (e.g., lysozyme, stomach acid, fatty acids).
Physical barriers: Structures that block entry (e.g., skin, mucous membranes).
Leukocytes and Lymphoid Tissues
Leukocytes are essential for immune responses. Primary lymphoid tissues (thymus, bone marrow) produce and mature leukocytes, while secondary lymphoid tissues (lymph nodes, spleen, MALT) filter lymph and sample antigens.
Cytokines and Complement System
Cytokines are signaling proteins that coordinate immune actions. The complement system is a cascade of proteins that enhances phagocytosis, inflammation, and cytolysis.
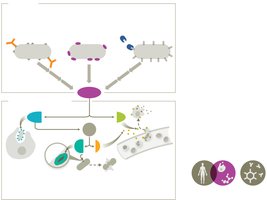
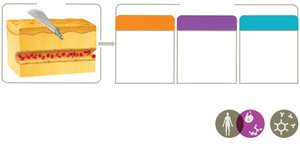
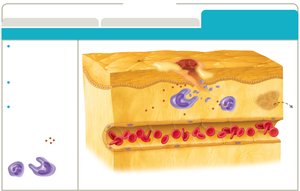
Inflammation
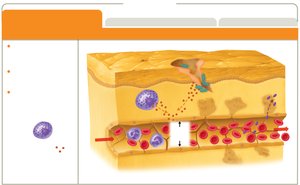
Inflammation is a key innate immune response, essential for healing. It occurs in three phases: vascular changes, leukocyte recruitment, and resolution.
Vascular changes: Increased blood flow and vessel permeability.
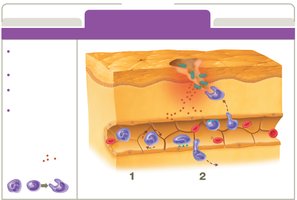
Leukocyte recruitment: Neutrophils and monocytes migrate to the site.
Resolution: Inflammation signals decrease; tissue repair begins.
Fever
Fever is a systemic innate response that enhances immune efficiency and limits pathogen growth.
Immune System Disorders
Primary and Secondary Immunodeficiencies
Primary immunodeficiencies are congenital, while secondary immunodeficiencies are acquired due to aging, disease, or medical interventions.
Autoimmunity and Hypersensitivities
Autoimmunity is an attack against self-tissues. Hypersensitivities are inappropriate immune responses classified into four types (ACID mnemonic):
Type I: Allergy (IgE mediated)
Type II: Cytotoxic (IgG or IgM mediated)
Type III: Immune complex (IgG or IgM mediated)
Type IV: Delayed (T cell mediated)
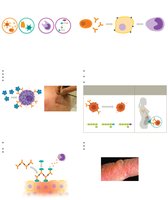
Humoral Immunity
Acquisition of Immunity
Humoral immunity can be acquired naturally or artificially, and is either passive or active.
Active immunity: Individual produces their own antibodies (infection or vaccination).
Passive immunity: Individual receives antibodies from another source (placenta, antivenom).
Visual Summary: Innate and Adaptive Immunity