 Back
BackNervous System Infections: Microbiology and Clinical Principles
Study Guide - Smart Notes

Nervous System Overview: Structure & Defenses
Central and Peripheral Nervous System
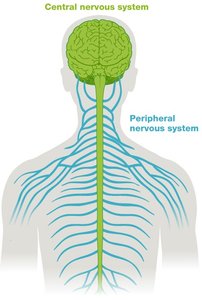
The nervous system is divided into two main parts: the Central Nervous System (CNS) and the Peripheral Nervous System (PNS). The CNS integrates information and consists of the brain and spinal cord, while the PNS transmits sensory input and motor output via nerves.
CNS: Brain and spinal cord; responsible for processing and integrating information.
PNS: Nerves outside the CNS; transmits signals to and from the CNS.
Neurons: Types and Structure
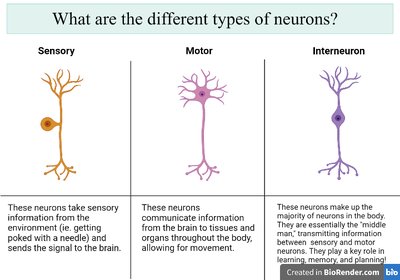
Neurons are specialized cells that transmit signals throughout the nervous system. They are classified based on their function:
Sensory (Afferent) Neurons: Carry sensory information from the environment to the CNS.
Motor (Efferent) Neurons: Transmit commands from the CNS to muscles and glands.
Interneurons: Connect neurons within the CNS and PNS, facilitating communication.
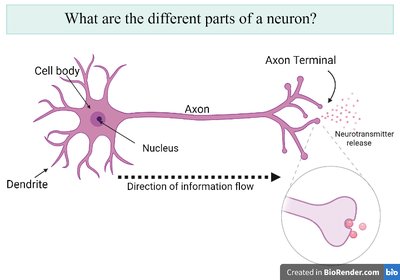
Neurons have distinct parts: dendrites (receive signals), cell body (contains nucleus), axon (transmits signals), and axon terminals (release neurotransmitters).
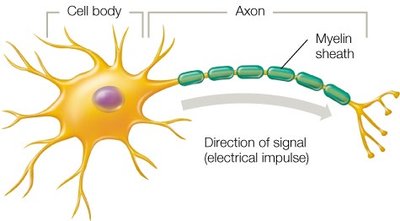
The axon may be covered by a myelin sheath, which increases the speed of electrical signal transmission.
Neurotransmitters
Neurotransmitters are chemical messengers released by neurons in response to stimuli. Examples include serotonin, dopamine, and epinephrine. They play a critical role in transmitting signals between neurons.
The Nervous System and the Microbiome
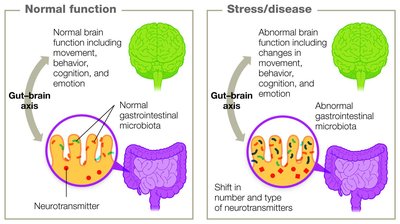
Microbiota and the Gut-Brain Axis
The nervous system itself contains no resident microbiota; any microbes present are considered abnormal and potentially pathogenic. However, the gut-brain axis describes the bidirectional communication between the gastrointestinal tract's microbiota and the nervous system, influencing mood, cognition, and neurological health.
Involves endocrine, nervous, and immune systems.
Impacts conditions such as anxiety, depression, and neurodegenerative diseases (e.g., Alzheimer's, Parkinson's).
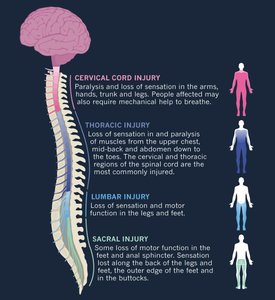
Vulnerability of the Nervous System
The brain, spinal cord, and nerves are highly susceptible to damage and have limited regenerative capacity. Loss of function due to injury or infection is often permanent, highlighting the importance of protective mechanisms.
Nervous System Defenses
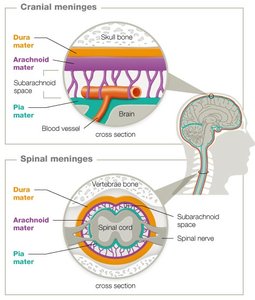
Meninges
The meninges are three protective tissue layers (dura mater, arachnoid mater, pia mater) that surround the brain and spinal cord. They provide physical protection, supply nutrients, and remove waste.
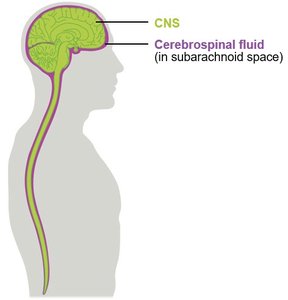
Cerebrospinal Fluid (CSF)
Cerebrospinal fluid is produced within the brain and acts as a cushion for the CNS, protecting it from physical trauma and helping to maintain homeostasis.
Blood–Brain Barrier (BBB)
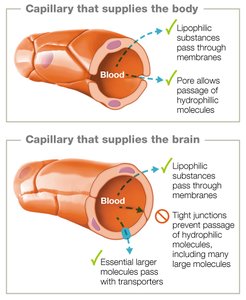
The blood–brain barrier is formed by specialized capillaries that tightly regulate the passage of substances from the blood into the CNS. Only small or lipophilic molecules can cross easily, protecting the brain from pathogens and toxins.
Limits pathogen access to the CNS.
Essential for maintaining the brain's microenvironment.
Nervous System Infections
Types and Causes
Nervous system infections are rare due to robust defenses but can occur, especially after injury or in immunocompromised individuals. Major types include:
Meningitis: Inflammation of the meninges.
Encephalitis: Inflammation of the brain.
Meningoencephalitis: Inflammation of both the brain and meninges.
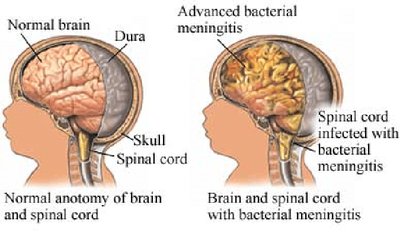
Viruses are the most common cause, but bacteria, fungi, and parasites can also be responsible. Viral forms generally have a better prognosis than bacterial forms.
Peripheral Nervous System Infections
Some viruses can persist in neurons and cause periodic flare-ups, but these are rarely classified as nervous system diseases unless neurological symptoms are present. Certain pathogens produce toxins that can disable the PNS.
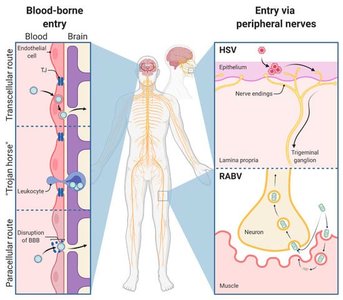
Viral Nervous System Infections
General Features
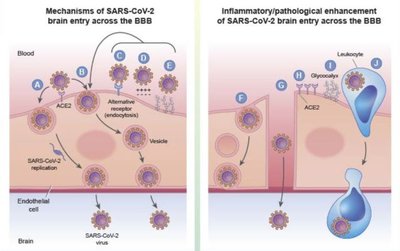
Viruses can more easily cross the blood–brain barrier due to their small size. Common viral infections of the nervous system include poliomyelitis, rabies, and arboviral encephalitis/meningitis.
Poliomyelitis (Polio)
Etiological agent: Poliovirus (Picornaviridae family), a small, non-enveloped RNA virus with a protein coat that protects it from stomach acid.
Transmission: Fecal-oral route.
Signs and symptoms: Most cases are mild (flulike), but the virus can travel from the gut to skeletal muscle and then to the CNS, causing neuron lysis, inflammation, and paralysis.
Complications: Muscle weakness, asymmetric or symmetric paralysis, post-polio syndrome (muscle deterioration years after recovery).
Treatment: Supportive; pleconaril may be used.
Prevention: Salk (IPV, inactivated) and Sabin (OPV, live attenuated) vaccines.

Rabies
Etiological agent: Rabies virus (Rhabdoviridae family), enveloped, single-stranded RNA virus. Transmission occurs via animal bites (zoonosis).
Incubation: 2–12 months.
Symptoms: Fever, nausea, paraesthesia, followed by neurological symptoms (pharyngeal spasms, hydrophobia, delirium, coma, death).
Mechanism: Replicates in muscle, travels to CNS, induces apoptosis without lysing cells.
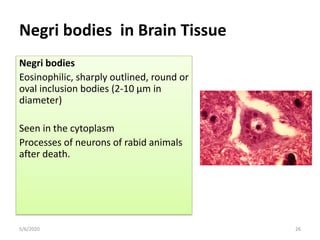
Treatment: Postexposure prophylaxis (antibodies, inactivated vaccine); Negri bodies in neurons are diagnostic.
Prevention: Vaccination of pets and at-risk humans.

Arboviral Encephalitis and Meningitis
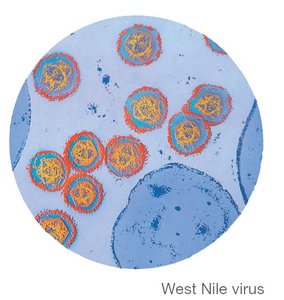
Etiological agents: Arboviruses (e.g., West Nile virus), enveloped, single-stranded RNA viruses transmitted by arthropods (mosquitoes).
Transmission: Zoonosis via mosquito bites; humans are dead-end hosts.
Symptoms: Flulike symptoms, fever, headache; severe cases cause neuroinvasive disease and death.
Prevention: Insect repellent, mosquito control.
Bacterial Nervous System Infections - CNS
General Features
Bacterial meningitis is less common but more severe than viral forms, with high rates of disability and mortality. Rapid progression requires immediate treatment.
Bacterial vs. Viral Meningitis: Diagnosis
CSF Culture: Bacterial meningitis shows growth; viral does not.
CSF Glucose: Bacterial meningitis often lowers glucose; viral does not affect glucose levels.
Haemophilus Meningitis
Etiological agent: Haemophilus influenzae (type b most serious), Gram-negative bacteria.
Transmission: Normal microbiota can invade blood and CSF.
Symptoms: Sudden fever, headache, stiff neck, confusion.
Complications: Near 100% mortality if untreated.
Treatment: Antibiotics; 3–6% mortality even with treatment.
Prevention: Hib vaccine; cases have dropped dramatically post-vaccine.
Meningococcal Meningitis
Etiological agent: Neisseria meningitidis, Gram-negative aerobe with a capsule (major virulence factor).
Transmission: Carried by 10% of population; outbreaks after capsular switching.
Symptoms: Rapid onset, petechial rash, can progress to death within hours if untreated.
Treatment: Antibiotics; high mortality if not treated promptly.
Prevention: Multiple vaccines targeting different serogroups.
Pneumococcal Meningitis
Etiological agent: Streptococcus pneumoniae, Gram-positive diplococcus, leading cause of bacterial meningitis.
Progression: Spreads from nose/throat to blood, then to CNS.
Mechanism: Produces pneumolysin exotoxin, causing severe inflammation and immune-mediated damage.
Symptoms: Similar to other meningitis; may include sensitivity to light, vomiting, subdural empyema.
Prevention: PCV7 vaccine; most cases in nonimmunized young children and elderly.
Listeria Meningitis (Listeriosis)
Etiological agent: Listeria monocytogenes, Gram-positive rod, grows at various pH and temperatures.
Transmission: Foodborne (tainted cheese, deli meats, produce).
Symptoms: Mild in healthy adults; severe in pregnant women, neonates, elderly, and immunocompromised.
Mechanism: Intracellular pathogen; escapes phagosome, uses actin tails to move between cells.
Complications: Can cross blood–brain barrier, cause fetal damage, neonatal meningitis, high mortality in elderly.
Prevention: Avoid high-risk foods; 1,600 cases and 260 deaths annually in the U.S.
Key Vocabulary
Meninges: Three layers of tissue encasing the CNS.
Cerebrospinal fluid (CSF): Fluid cushioning and nourishing the CNS.
Meningitis: Inflammation of the meninges.
Encephalitis: Inflammation of the brain.
Meningoencephalitis: Inflammation of both brain and meninges.
Immunocompromised: Individual with a weakened immune system.
Zoonosis: Disease transmitted from animals to humans.
Flaccid paralysis: Paralysis with loss of muscle tone.
Serotype: Group of microbes with shared surface antigens.
