 Back
BackNormal Flora, Symbiosis, and Infectious Disease: Microbiome and Epidemiology
Study Guide - Smart Notes

Normal Flora and Symbiosis
Introduction to the Human Microbiome
The human body is a complex ecosystem inhabited by trillions of microorganisms, collectively known as the microbiota or normal flora. These microbes play essential roles in health and disease, forming intricate relationships with their human host. The study of these interactions is central to understanding infectious diseases and the maintenance of health.
Human cells vs. Bacterial cells: The human body contains approximately as many bacterial cells as human cells, with bacteria making up a significant portion of the total cell count but a much smaller fraction of body mass.
Microbiome: The collective genomes of the microbiota, studied using metagenomics, which allows for the identification and cataloging of microbes without the need for culturing.

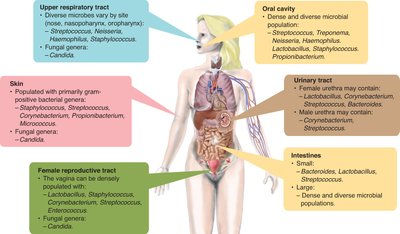
Sites of Normal Microbiota in the Human Body
Normal microbiota colonize various body sites, each with distinct microbial communities. These sites include the skin, oral cavity, upper respiratory tract, intestines, urinary tract, and female reproductive tract.
Skin: Dominated by Gram-positive bacteria such as Staphylococcus and Micrococcus.
Oral cavity: Contains diverse genera including Streptococcus and Neisseria.
Intestines: Populated by Bacteroides, Lactobacillus, and others.
Female reproductive tract: Rich in Lactobacillus and Streptococcus.
Types of Symbiotic Relationships
Symbiosis refers to the close association between two different species. In the context of microbiology, it describes the interactions between humans and their microbiota. There are four main types of symbiotic relationships:
Type | Organism 1 | Organism 2 | Example |
|---|---|---|---|
Mutualism | Benefits | Benefits | Bacteria in human colon |
Commensalism | Benefits | Neither benefits nor is harmed | Mites in human hair follicles |
Amensalism | Is harmed | Neither benefits nor is harmed | Fungus secreting antibiotic, inhibiting bacteria |
Parasitism | Benefits | Is harmed | Tuberculosis bacteria in human lung |

Microbiota Beyond Humans: The Rhizosphere
Plant-Microbe Interactions
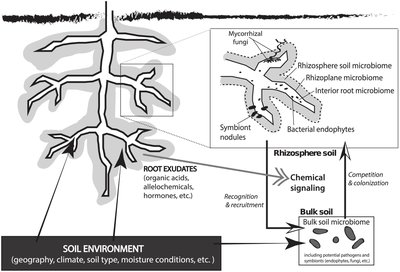
The rhizosphere is the narrow region of soil influenced by root secretions and associated microbial activity. This 'root microbiome' is crucial for nutrient cycling, especially nitrogen fixation, and plant health.
Rhizobium: Nitrogen-fixing bacteria that form symbiotic nodules on plant roots, converting atmospheric nitrogen into forms usable by plants.
Soil Microbiome: Includes mycorrhizal fungi, bacterial endophytes, and other organisms that interact with plant roots.

Acquisition and Development of the Human Microbiome
Establishment of Microbiota
Humans are born with a sterile internal environment. Colonization by microbiota begins during birth and continues through early life, influenced by delivery mode (vaginal vs. Caesarian), feeding (breast milk vs. formula), and environment.
Vaginal birth: Infants acquire microbiota similar to their mother's vaginal and gut flora.
Caesarian birth: Infants are colonized by environmental microbes, which may increase risk for certain diseases.
Breastfeeding: Human milk contains complex carbohydrates that nourish beneficial bacteria such as Bifidobacterium longum infantis.

Microbiota and Human Health
Benefits of Normal Microbiota
Normal microbiota provide numerous benefits to the host, including:
Competing with pathogens for resources and attachment sites
Producing vitamins (e.g., vitamin K, B vitamins)
Maintaining proper pH (e.g., in the vagina)
Stimulating immune system development
Protecting against chronic diseases
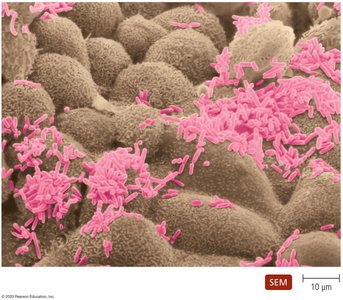
Opportunistic Pathogens
Normal microbiota can become opportunistic pathogens under certain conditions, such as:
Introduction into unusual body sites
Immune suppression
Disruption of normal microbiota (e.g., antibiotic use)
Infectious Diseases: Concepts and Epidemiology
Reservoirs of Infection
Pathogens are maintained in reservoirs, which can be:
Animal reservoirs: Zoonoses are diseases transmitted from animals to humans.
Human carriers: Infected individuals who may or may not show symptoms.
Nonliving reservoirs: Soil, water, and food contaminated with pathogens.
Disease | Causative Agent | Animal Reservoir | Mode of Transmission |
|---|---|---|---|
Malaria | Plasmodium spp. | Monkeys | Bite of Anopheles mosquito |
Rabies | Rabies virus | Bats, skunks, foxes, dogs | Bite of infected animal |
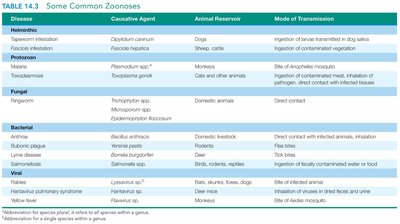
Transmission of Infectious Diseases
Diseases can be transmitted by direct contact, indirect contact (fomites), vehicles (air, water, food), and vectors (biological or mechanical).
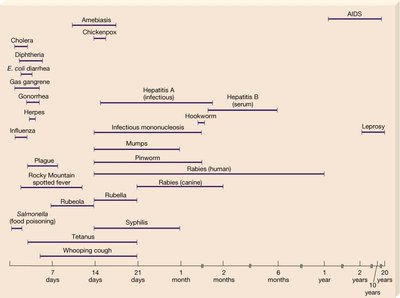
Stages of Infectious Disease
The progression of infectious disease typically follows these stages:
Incubation period: No signs or symptoms
Prodromal period: Mild, general symptoms
Illness: Most severe signs and symptoms
Decline: Declining signs and symptoms
Convalescence: Recovery; no signs or symptoms
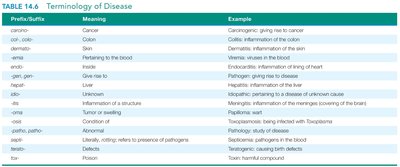
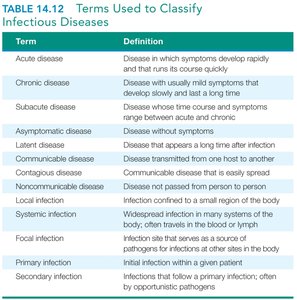
Classification of Infectious Diseases
Term | Definition |
|---|---|
Acute disease | Symptoms develop rapidly and run a short course |
Chronic disease | Symptoms develop slowly and last a long time |
Latent disease | Pathogen remains inactive for a time but can reactivate |
Communicable disease | Transmitted from one host to another |
Noncommunicable disease | Not transmitted from host to host |
Manifestations of Disease
Symptoms (Sensed by Patient) | Signs (Detected by Observer) |
|---|---|
Pain, nausea, headache, chills, fatigue, malaise, discomfort, itching, abdominal cramps | Swelling, rash, vomiting, diarrhea, fever, pus, anemia, leukocytosis/leukopenia, bubo, tachycardia/bradycardia |

Epidemiology: Occurrence and Spread of Disease
Key Epidemiological Terms
Incidence: Number of new cases in a given area during a specific period.
Prevalence: Total number of cases in a given area during a specific period.
Endemic: Disease constantly present in a population.
Epidemic: Disease acquired by many hosts in a short time.
Pandemic: Worldwide epidemic.
Sporadic: Disease that occurs occasionally.
Herd immunity: Immunity in most of a population, reducing disease spread.
Models of Disease Spread
The SIR model (Susceptible, Infected, Removed) is used to understand and predict the spread of infectious diseases in populations.
Index Case
The index case (or "patient zero") is the first documented patient in an outbreak, crucial for tracing the source and understanding the spread of disease.
Summary Table: Types of Symbiotic Relationships
Type | Definition | Example |
|---|---|---|
Mutualism | Both organisms benefit | Bacteria in human colon |
Commensalism | One benefits, other unaffected | Mites in hair follicles |
Amensalism | One harmed, other unaffected | Fungus secreting antibiotic |
Parasitism | One benefits, other harmed | Tuberculosis in lungs |
Additional info: These notes integrate foundational concepts from microbiology, including the human microbiome, symbiosis, infectious disease transmission, and epidemiology, as outlined in standard college-level microbiology curricula.
