 Back
BackPathogenic Gram-Positive and Gram-Negative Bacteria: Structure, Pathogenicity, and Clinical Relevance
Study Guide - Smart Notes

Pathogenic Gram-Positive Bacteria
Staphylococcus
Staphylococcus species are Gram-positive cocci that are part of the normal human microbiota but can also cause a range of diseases, from minor skin infections to life-threatening systemic conditions.
Structure and Physiology: Gram-positive, anaerobic, spherical cells arranged in clusters. Notable for salt, heat, and desiccation tolerance.
Key Species: S. aureus (more virulent) and S. epidermidis (opportunistic, especially with medical devices).
Pathogenicity: Determined by evasion of phagocytosis, enzyme production, and toxin secretion.
Structural Defenses Against Phagocytosis
Protein A: Binds antibody stems, inhibiting opsonization and complement activation.
Coagulase: Forms protective fibrin clots around bacteria.
Capsule: Polysaccharide layer inhibits chemotaxis and phagocytosis.
Enzymes
Coagulase: Triggers clotting (only S. aureus).
Hyaluronidase: Breaks down tissue matrix, aiding spread.
Staphylokinase: Dissolves clots for bacterial escape.
Lipase: Digests skin oils, supporting growth on skin.
Penicillinase: Confers resistance to beta-lactam antibiotics.
Toxins
Cytolytic Toxins: Disrupt cell membranes (e.g., leukocidin targets leukocytes).
Exfoliative Toxins: Cause skin cell separation (e.g., scalded skin syndrome).
Toxic Shock Syndrome Toxin: Induces systemic shock.
Enterotoxins: Cause food poisoning; heat-stable.
Diseases
Non-Invasive: Food poisoning (nausea, vomiting, diarrhea).
Cutaneous: Impetigo, folliculitis, furuncles, carbuncles, scalded skin syndrome.
Systemic: Toxic shock syndrome, bacteremia, endocarditis, pneumonia, osteomyelitis.
Diagnosis, Treatment, and Prevention
Diagnosis: Microscopy, coagulase test.
Treatment: Vancomycin for MRSA; removal of pus; long-term therapy for systemic infections.
Prevention: Hand hygiene, especially in healthcare settings.
Streptococcus
Streptococcus species are Gram-positive cocci arranged in chains or pairs, classified by serological properties (Lancefield groups), hemolysis, and genetic analysis.
Group A (S. pyogenes): Causes pharyngitis, scarlet fever, rheumatic fever, pyoderma, erysipelas, cellulitis, necrotizing fasciitis, glomerulonephritis.
Virulence Factors: M protein, hyaluronic acid capsule, C5a peptidase, hyaluronidase, pyrogenic toxins, streptolysins.
Diagnosis/Treatment: Rapid strep test, penicillin (or erythromycin/cephalosporin), surgical removal for necrotizing fasciitis.
Group B (S. agalactiae): Neonatal bacteremia, meningitis, pneumonia; diagnosed by ELISA, treated with penicillin/ampicillin.
Other Beta Hemolytic: S. equisimilis, S. anginosus (pharyngitis).
Alpha Hemolytic (Viridans): Dental caries, endocarditis, meningitis; produce dextran for biofilm formation.
S. pneumoniae: Pneumonia, sinusitis, otitis media, bacteremia, endocarditis, meningitis; diagnosed by Quellung reaction, treated with penicillin or alternatives, prevented by vaccine.
Enterococcus
Gram-positive cocci, Lancefield group D, non-hemolytic, inhabit intestines. E. faecalis and E. faecium can cause HAI bacteremia, endocarditis, and wound infections. Resistant to harsh conditions and many antibiotics.
Bacillus
Large, rod-shaped, endospore-forming bacteria. B. anthracis causes anthrax (cutaneous, inhalational, gastrointestinal). Virulence due to capsule and anthrax toxins.
Clostridium
Anaerobic, endospore-forming rods. Notable for potent exotoxins. C. difficile causes antibiotic-associated diarrhea and pseudomembranous colitis. Treated by discontinuing causative antibiotics, metronidazole, or vancomycin.
Listeria
Non-spore-forming, can grow at refrigeration temperatures. Causes listeriosis, especially dangerous for immunocompromised individuals. Treated with antibiotics.
Mycoplasma
Smallest free-living microbes, lack cell wall, associated with pneumonia. Require host-derived sterols for growth.
Corynebacterium
High G+C, non-endospore-forming, pleomorphic rods. C. diphtheriae causes diphtheria via toxin production. Diagnosed by pseudomembrane and Elek test; treated with antitoxin and antibiotics; prevented by DTaP vaccine.
Mycobacterium
Non-endospore-forming, slow-growing, waxy mycolic acid in cell wall. Resistant to desiccation, lysis, and many drugs.
Propionibacterium
Anaerobic rods, cause acne by growing in sebaceous glands. Treated with antibiotics or retinoids in severe cases.
Pathogenic Gram-Negative Bacteria
General Features
Gram-negative bacteria possess an outer membrane containing Lipid A (endotoxin), which is responsible for many of their pathogenic effects, including fever, inflammation, shock, and disseminated intravascular coagulation (DIC).
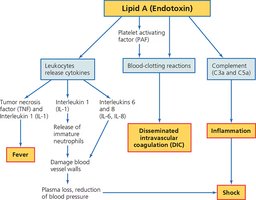
Lipid A Effects: Triggers cytokine release, blood clotting, complement activation, leading to fever, inflammation, DIC, and shock.
Classification
Bergey's Manual: Groups bacteria by DNA similarities.
Clinical: Grouped by shape, oxygen requirements, and biochemical traits.
Neisseria
The only Gram-negative cocci genus commonly causing human disease. Includes N. gonorrhoeae (gonorrhea) and N. meningitidis (meningitis).
Structure: Gram-negative diplococci, nonmotile, oxidase positive, fastidious.
Virulence: Fimbriae, capsule, lipooligosaccharide (LOS with Lipid A).
Diagnosis: Microscopy, culture, sugar fermentation tests.
Treatment: Ceftriaxone plus azithromycin/doxycycline for gonorrhea; cephalosporins for meningitis.
Prevention: Vaccines (except for some strains), prophylactic antibiotics, safe practices.
Facultatively Anaerobic Gram-Negative Bacilli
Families: Enterobacteriaceae (oxidase negative), Pasteurellaceae (oxidase positive).
Virulence Factors: LPS, capsules, fimbriae, exotoxins, siderophores, hemolysins, type III secretion systems, drug resistance enzymes.
Diagnosis: Selective/differential media (EMB, MacConkey), serology, Kirby-Bauer testing.
Prevention: Hygiene, sewage control, prudent antibiotic use.
Enterobacteriaceae Clinical Groups
Coliforms: Rapid lactose fermenters, normal microbiota, opportunists (e.g., E. coli).
Noncoliform Opportunists: Do not ferment lactose (e.g., Proteus).
True Pathogens: Always pathogenic (e.g., Salmonella, Shigella, Yersinia).
Key Genera and Diseases
E. coli: Gastroenteritis, UTIs, neonatal meningitis, HUS. Virulence via toxins, fimbriae, type III secretion system.
Klebsiella: Pneumonia, UTIs, bacteremia; large capsule resists phagocytosis.
Serratia: HAI, red pigment, antibiotic resistance.
Proteus: Swarming motility, UTIs, stone formation via urease.
Salmonella: Salmonellosis, typhoid fever; systemic spread possible.
Shigella: Shigellosis, shiga toxin, severe dysentery.
Yersinia: Plague (bubonic, pneumonic), enteric illness.
Pasteurellaceae
Pasteurella: Animal bites, local inflammation, bacteremia in immunocompromised.
Haemophilus: H. influenzae type b (Hib) causes meningitis, epiglottitis, arthritis; prevented by Hib vaccine.
Pathogenic Gram-Negative Anaerobic Bacilli
Bacteroides: Bile tolerant, colon resident, low endotoxin activity, causes GI and wound infections.
Prevotella: Bile sensitive, found in urinary, genital, and respiratory tracts; causes periodontal, gynecological, and brain abscesses.
Summary Table: Key Features of Gram-Negative Pathogens
Genus | Key Diseases | Virulence Factors | Diagnosis | Treatment/Prevention |
|---|---|---|---|---|
Neisseria | Gonorrhea, Meningitis | Fimbriae, Capsule, LOS | Microscopy, Culture | Cephalosporins, Vaccine (meningitis) |
Escherichia | UTI, Gastroenteritis, HUS | Fimbriae, Exotoxins, Type III system | Cultures, Serology | Supportive, Antibiotics (if needed) |
Klebsiella | Pneumonia, UTI | Capsule | Cultures | Antibiotics (resistance common) |
Salmonella | Salmonellosis, Typhoid | Type III system, Capsule | Stool/Blood culture | Fluids, Antibiotics (typhoid) |
Shigella | Shigellosis | Shiga toxin | Stool culture | Fluids, Antibiotics |
Yersinia | Plague | Type III system | Cultures | Antibiotics |
Pasteurella | Wound infections | Capsule | Cultures | Oral antibiotics |
Haemophilus | Meningitis, Epiglottitis | Capsule | CSF culture | IV cephalosporin, Vaccine (Hib) |
Bacteroides | GI, wound infections | Capsule, Fimbriae | Anaerobic culture | Metronidazole |
Prevotella | Periodontal, abscesses | Proteases | Anaerobic culture | Carbapenem, Surgery |
