Back
BackChapter 18-19_Hypersensitivities & Vaccines
Study Guide - Smart Notes

Practical Applications of Immunology
Vaccines and Immunization
Vaccines are preparations derived from pathogens or their products, designed to induce active immunity and protect individuals and populations from infectious diseases. Immunization is a critical public health tool that prevents the spread of diseases and can lead to herd immunity, reducing disease prevalence even among unvaccinated individuals.
Vaccine: A suspension of organisms or fractions of organisms used to induce immunity.
Immunologic Memory: The ability of the immune system to respond more rapidly and effectively to pathogens that have been encountered previously.
Herd Immunity: When a significant portion of a population is immune, the spread of disease is minimized.
Artificial Passive Immunity: Transfer of antibodies from another individual, used for immediate protection.
Natural Passive Immunity: Transfer of maternal antibodies to the fetus or infant, providing temporary protection.
Types of Vaccines
Vaccines can be classified based on their composition and method of preparation. Each type has specific advantages and limitations.
Attenuated Whole-Agent Vaccines: Contain live, weakened pathogens (e.g., MMR vaccine). Induce strong, long-lasting immunity but may not be suitable for immunocompromised individuals.
Inactivated Whole-Agent Vaccines: Contain killed pathogens (e.g., Salk polio vaccine). Safer but often require booster doses.
Subunit Vaccines: Contain only antigenic fragments (e.g., pertussis, hepatitis B).
Toxoid Vaccines: Contain inactivated toxins (e.g., diphtheria, tetanus).
Conjugated Vaccines: Combine polysaccharides with proteins to enhance immunogenicity (e.g., Hib vaccine).
DNA and Recombinant Vaccines: Use genetic material or recombinant proteins to induce immunity (e.g., rVSV-ZEBOV for Ebola).
Examples of Principal Vaccines Used in the USA
Bacterial Vaccines: Diphtheria (toxoid), Meningococcal (polysaccharide), Pertussis (acellular fragments), Pneumococcal (polysaccharide), Tetanus (toxoid), Hib (conjugated).
Viral Vaccines: Influenza (inactivated/attenuated), Measles, Mumps, Rubella, Chickenpox (attenuated), Polio (inactivated), Rabies (inactivated), Hepatitis B (subunit), Hepatitis A (inactivated), Smallpox (live vaccinia), HPV (subunit).
Development and Delivery of Vaccines
Modern vaccine development utilizes recombinant DNA technology and aims to induce both humoral and cellular immunity. Adjuvants, such as alum, are used to enhance immune responses. Combination vaccines and proper storage are essential for efficacy and safety.
Controversies and Public Health Impact
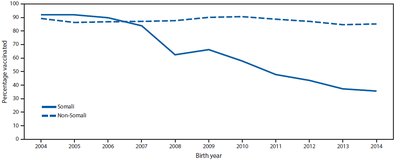
Vaccines have dramatically reduced morbidity and mortality from infectious diseases. Despite occasional controversies, such as the fraudulent claim linking MMR vaccine to autism, scientific evidence supports vaccine safety and efficacy. Outbreaks, such as the 2017 measles outbreak in Minnesota, highlight the risks of declining vaccination rates.
Immunology-Based Diagnostic Tests
Serological Tests
Serological tests detect the presence of antigens or antibodies in patient samples, aiding in the diagnosis of infectious and autoimmune diseases.
Direct Tests: Detect antigens from patient samples.
Indirect Tests: Detect antibodies in patient serum.
Types of Serological Reactions
Precipitation Reactions: Soluble antigens and antibodies form visible precipitates.
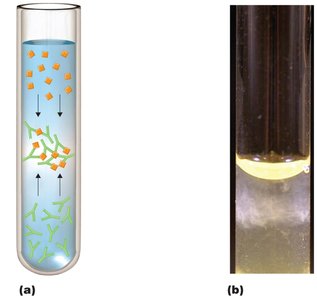
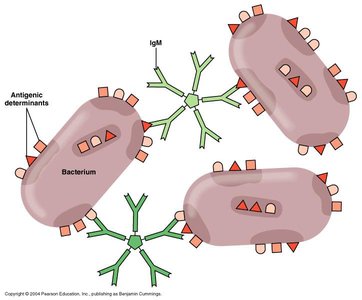
Agglutination Reactions: Particulate antigens (e.g., cells, beads) clump together in the presence of specific antibodies.
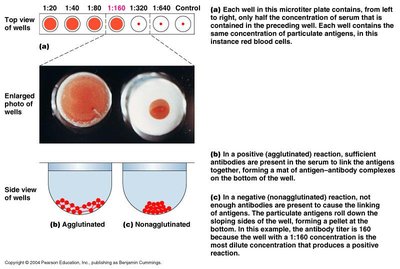
Measuring Antibody Titer: The highest dilution of serum that still produces agglutination indicates antibody concentration.
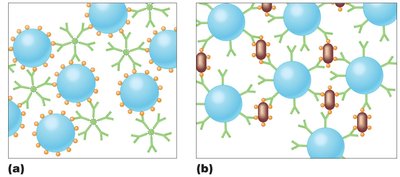
Indirect Agglutination Tests: Use particles coated with antigen or antibody to detect corresponding antibodies or antigens in patient samples.
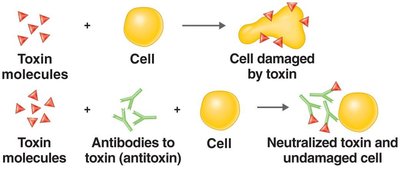
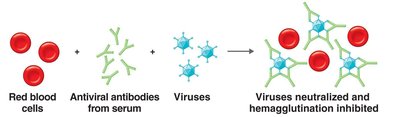
Neutralization Reactions: Antibodies neutralize toxins or viruses, preventing cell damage.
Hemagglutination: Agglutination of red blood cells, used in blood typing and viral diagnostics.
Hemagglutination Inhibition: Antibodies prevent viral-induced agglutination of RBCs.
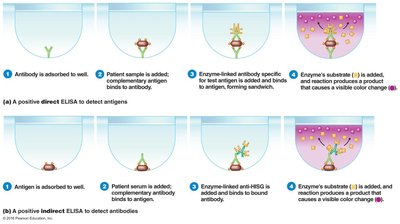
ELISA (Enzyme-Linked Immunosorbent Assay): Detects antigens or antibodies using enzyme-linked indicators and color change.
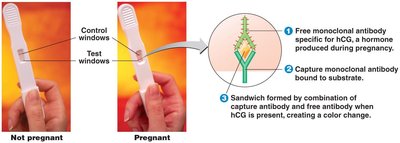
Monoclonal Antibody-Based Tests: Used in home pregnancy tests and other rapid diagnostics.
Hypersensitivities
Definition and Types
Hypersensitivity reactions are exaggerated or inappropriate immune responses to antigens (allergens) in previously sensitized individuals. They are classified into four main types based on their mechanisms and timing.
Type of Reaction | Time Before Clinical Signs | Characteristics | Examples |
|---|---|---|---|
Type I (Anaphylactic) | < 30 min | IgE binds to mast cells/basophils, degranulation, release of mediators | Anaphylactic shock, hay fever, asthma |
Type II (Cytotoxic) | 5–12 hours | IgG/IgM antibodies + complement cause cell lysis | Transfusion reactions, Rh incompatibility |
Type III (Immune Complex) | 3–8 hours | Antigen-antibody complexes deposit in tissues, activate complement | Arthus reaction, serum sickness |
Type IV (Delayed Cell-Mediated) | 24–48 hours | Cell-mediated response, T cells activate macrophages | Contact dermatitis, transplant rejection |

Type I: Anaphylactic Reactions
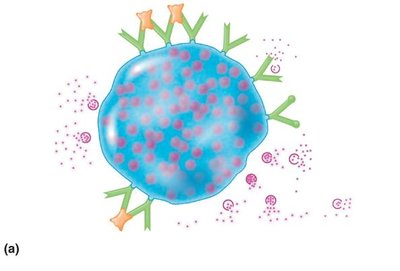
Type I hypersensitivity involves IgE-mediated degranulation of mast cells and basophils, releasing histamine and other mediators. Symptoms can be localized (e.g., hay fever, asthma) or systemic (anaphylactic shock).
Mechanism: First exposure leads to IgE production; subsequent exposure causes cross-linking of IgE on mast cells, triggering mediator release.
Mediators: Histamine (vasodilation, increased permeability), leukotrienes (smooth muscle contraction), prostaglandins (mucus secretion).
Type II: Cytotoxic Reactions
Type II hypersensitivity involves IgG or IgM antibodies directed against cell surface antigens, leading to complement activation and cell lysis. Classic examples include transfusion reactions and hemolytic disease of the newborn (Rh incompatibility).
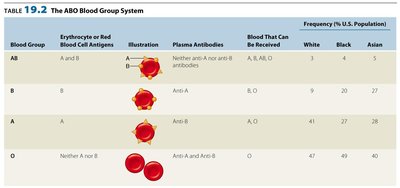
ABO Blood Group System: Blood types are determined by carbohydrate antigens on RBCs. Incompatible transfusions result in antibody-mediated lysis of donor RBCs.
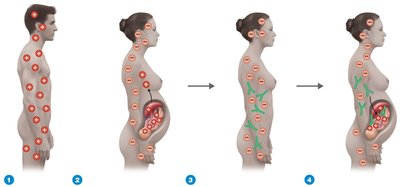
Rh Factor: Rh- individuals can develop anti-Rh antibodies after exposure to Rh+ blood, leading to hemolytic disease in subsequent pregnancies.
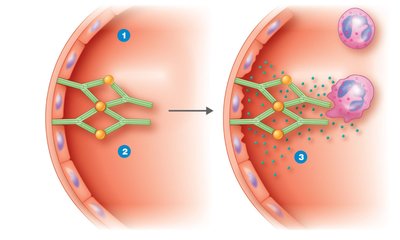
Type III: Immune Complex Reactions
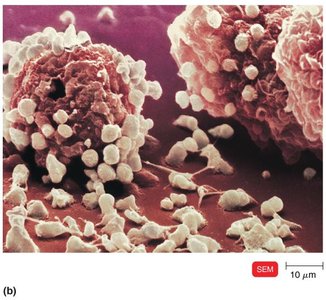
Type III hypersensitivity is caused by immune complexes (antigen-antibody aggregates) that deposit in tissues, activate complement, and attract neutrophils, resulting in tissue damage. Examples include glomerulonephritis and serum sickness.
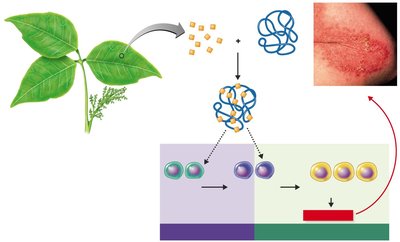
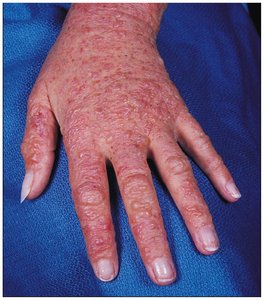
Type IV: Delayed Cell-Mediated Reactions
Type IV hypersensitivity is mediated by T cells rather than antibodies. Upon re-exposure to antigen, memory T cells activate macrophages and cause inflammation. Examples include contact dermatitis (e.g., poison ivy) and transplant rejection.
Autoimmune Diseases and Immunopathology
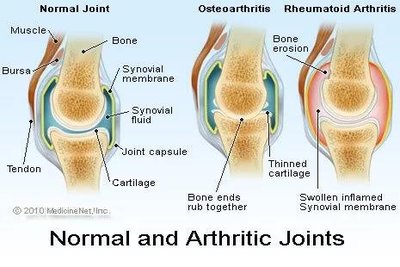
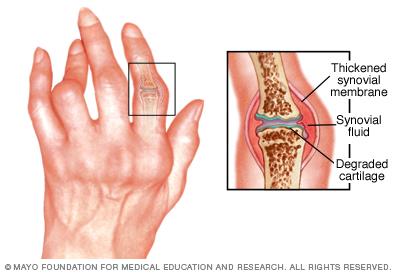
Autoimmune diseases occur when the immune system attacks self-antigens, leading to tissue damage. Examples include rheumatoid arthritis, where antibodies target synovial membrane proteins, causing joint inflammation and deformity.
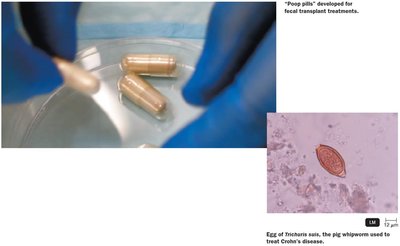
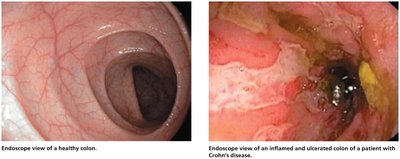
The Hygiene Hypothesis
The hygiene hypothesis suggests that reduced exposure to microbes in early life may increase susceptibility to allergies and autoimmune diseases. Dysbiosis, or imbalance of the normal microbiota, can contribute to inflammatory diseases such as Crohn's disease. Treatments include fecal transplants and, experimentally, helminth therapy.