Back
BackPractical Applications of Immunology: Vaccines and Diagnostic Immunology
Study Guide - Smart Notes

Practical Applications of Immunology
Vaccines
Vaccines are a cornerstone of immunology, providing artificial immunity to infectious diseases. They work by stimulating the immune system to produce a primary response, leading to the formation of memory cells and antibodies, which enable a rapid and robust secondary response upon future exposure to the pathogen.
Vaccine: A suspension of organisms or fractions of organisms that induce immunity.
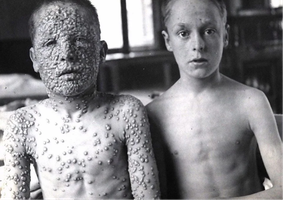
Variolation: Early method of inoculating smallpox (Variola virus) into the skin.
Edward Jenner: Pioneered vaccination by using cowpox (Vaccinia virus) to prevent smallpox.
Herd Immunity: When most of the population is immune, outbreaks are sporadic due to the lack of susceptible individuals.
Principles and Effects of Vaccination
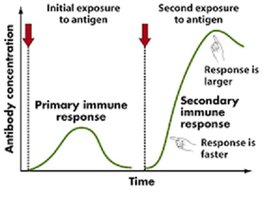
Vaccination provokes a primary immune response, leading to the formation of antibodies and memory cells. Upon subsequent exposure to the same antigen, the immune system mounts a faster and more intense secondary response.
Primary Immune Response: Initial response to antigen exposure, slower and less robust.
Secondary Immune Response: Faster and stronger response upon re-exposure due to memory cells.
Types of Vaccines
Vaccines can be classified based on their composition and method of preparation. Each type has distinct advantages and limitations.
Live Attenuated Vaccines: Contain weakened pathogens that closely mimic natural infection. Provide long-lasting immunity but are not suitable for immunocompromised individuals.
Inactivated (Killed) Vaccines: Contain killed pathogens. Safer but require booster doses and induce mainly humoral immunity.
Subunit Vaccines: Use antigenic fragments to stimulate an immune response. Includes recombinant and virus-like particle (VLP) vaccines.
Conjugated Vaccines: Combine polysaccharide antigens with proteins to enhance immunogenicity, especially in children.
Nucleic Acid (DNA) Vaccines: Injected DNA produces protein antigens, stimulating both humoral and cellular immunity.
Toxoids: Inactivated toxins used to target harmful bacterial substances.
Antitoxins: Serums containing antibodies against toxins.
Principal Vaccines Used in the United States
The following tables summarize the main vaccines used to prevent bacterial and viral diseases in humans, including their recommendations and booster requirements.
Disease | Vaccine | Recommendation | Booster |
|---|---|---|---|
Haemophilus influenzae type b meningitis | Polysaccharide from Haemophilus influenzae type b conjugated with protein | Children prior to school age | None recommended |
Meningococcal meningitis | Purified polysaccharide from Neisseria meningitidis | For people with substantial risk of infection | Not established |
Pneumococcal pneumonia | Purified polysaccharide from Streptococcus pneumoniae | For adults with certain chronic diseases | Recommended every 5–10 years |
Tetanus, diphtheria, and pertussis | DTP: inactivated toxin and acellular fragments | Children at 2, 4, 6, 15–18 months, and 4–6 years | Booster every 10 years |

Disease | Vaccine | Recommendation | Booster |
|---|---|---|---|
Chickenpox | Attenuated virus | For infants aged 12 months | Duration of immunity not known |
Hepatitis A | Inactivated virus | For people at risk | Duration of protection not known |
Hepatitis B | Antigenic fragments of virus | For infants and children, and adults at risk | Duration of protection not known |
Influenza | Inactivated or attenuated virus | For chronically ill, elderly, and children | Annual |


Adjuvants
Adjuvants are chemical additives used in vaccines to enhance their effectiveness by improving the innate immune response. Common adjuvants include aluminium hydroxide and aluminium phosphate.
Safety of Vaccines
Vaccines are among the safest and most effective means of preventing infectious diseases. Rarely, vaccines can cause adverse effects, but there is no scientific evidence linking vaccines such as MMR to autism.
Diagnostic Immunology
Sensitivity and Specificity
Diagnostic tests are evaluated based on their sensitivity and specificity:
Sensitivity (True Positive Rate): Probability that a test correctly identifies a true positive specimen.
Specificity (True Negative Rate): Probability that a test correctly identifies a true negative specimen.
Monoclonal Antibodies
Monoclonal antibodies (Mabs) are uniform, highly specific antibodies produced in large quantities by hybridoma cells (fusion of a myeloma cell and an antibody-producing B cell). They are used in diagnostics and therapy.
Murine Mabs: Mouse proteins (-omab)
Chimeric Mabs: Mouse variable region, human constant region (-ximab)
Humanized Mabs: Mostly human, mouse antigen-binding sites (-zumab)
Fully Human Mabs: Produced from human gene in mouse (-umab)
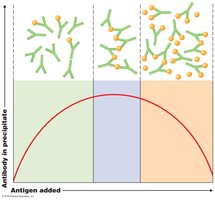
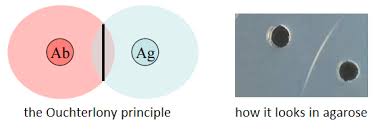
Precipitation Reactions
Precipitation reactions involve the reaction of soluble antigens with antibodies to form visible aggregates (lattices). The optimal ratio of antigen to antibody forms a precipitate, as seen in the precipitin ring test and immunodiffusion tests (Ouchterlony principle).

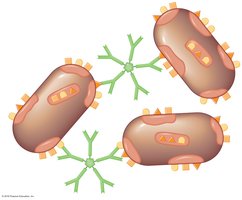
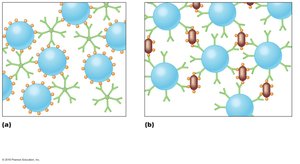
Agglutination Reactions
Agglutination reactions occur when particulate antigens bind to antibodies, forming visible aggregates. These tests can be direct (detecting antibodies against large cellular antigens) or indirect (using particles coated with antigens or antibodies).
Titer: Concentration of serum antibody.
Seroconversion: Significant change in titer as a disease progresses.
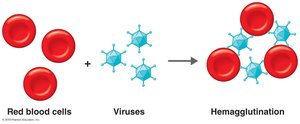
Hemagglutination
Hemagglutination is the agglutination of red blood cells (RBCs) by antibodies or viruses. It is used in blood typing and viral diagnostics. Viral hemagglutination occurs when viruses agglutinate RBCs without antigen-antibody reactions.
Neutralization Reactions
Neutralization reactions involve antibodies blocking the harmful effects of exotoxins or viruses. The viral hemagglutination inhibition test is used for subtyping viruses by mixing viruses and RBCs with patient serum; inhibition of hemagglutination indicates the presence of antibodies.
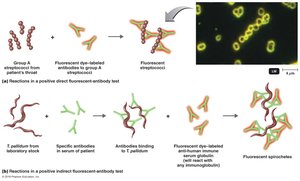
Fluorescent-Antibody Techniques
These techniques use antibodies labeled with fluorescent dyes to detect antigens or antibodies. Direct FA tests identify microorganisms in clinical specimens, while indirect FA tests detect specific antibodies in serum.
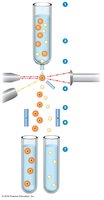
Fluorescence-Activated Cell Sorter (FACS)
FACS is a specialized technique that sorts cells based on their fluorescence and size. Cells are labeled with fluorescent antibodies, passed through a laser, and separated into different tubes based on their properties.
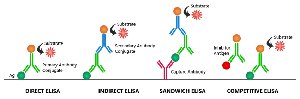
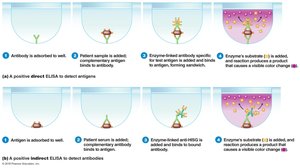
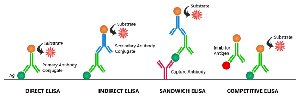
Enzyme-Linked Immunosorbent Assay (ELISA)
ELISA is a sensitive technique for detecting antigens or antibodies. In direct ELISA, antigens are detected using enzyme-linked antibodies. In indirect ELISA, antibodies are detected using a secondary enzyme-linked antibody. A color change indicates a positive result.
Monoclonal Antibodies in Home Pregnancy Tests
Home pregnancy tests use monoclonal antibodies to detect human chorionic gonadotropin (hCG) in urine. The test forms a visible line when hCG is present, indicating pregnancy.
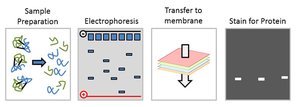
Western Blotting
Western blotting is an analytical technique used to identify specific proteins in a sample. Proteins are separated by electrophoresis, transferred to a membrane, and detected using antibodies.