 Back
BackPractical Applications of Immunology: Vaccines and Diagnostic Immunology
Study Guide - Smart Notes

Practical Applications of Immunology
Introduction
This chapter explores the principles and applications of immunology in the prevention, diagnosis, and treatment of infectious diseases. It focuses on vaccines, their types, mechanisms, and safety, as well as immunological diagnostic techniques.
Vaccines
History and Definition
Variolation: Early method involving inhalation or inoculation of smallpox scabs, resulting in mild infection and subsequent immunity. Mortality was about 1% compared to 50% for natural smallpox.
Vaccination: Introduced by Jenner (1798) using cowpox to prevent smallpox, later termed by Pasteur. Safer than variolation.
Vaccine: A suspension of organisms or their fractions that induces immunity.
Principles and Effects of Vaccination
Provokes a primary immune response, leading to antibody and memory cell formation without causing illness.
Enables a rapid, intense secondary response upon future exposure (immunity).
Herd immunity: When most of the population is immune, outbreaks are sporadic due to a lack of susceptible individuals. The required percentage for herd immunity depends on disease virulence (e.g., polio: 80–85%, measles: 90–95%).

Types of Vaccines and Their Characteristics
Live attenuated vaccines: Contain weakened pathogens that replicate in the host, mimicking natural infection and inducing strong, lifelong immunity (both cellular and humoral). Example: MMR vaccine.
Inactivated vaccines: Contain killed bacteria or inactivated viruses. Safer but require booster doses and mainly induce humoral immunity.
Subunit vaccines: Use antigenic fragments to stimulate an immune response. Includes recombinant vaccines (produced by genetic modification) and virus-like particle (VLP) vaccines.
Toxoids: Inactivated toxins (e.g., diphtheria, tetanus). Require boosters.
Conjugated vaccines: Combine antigens with proteins to enhance immune response, especially for polysaccharide antigens.
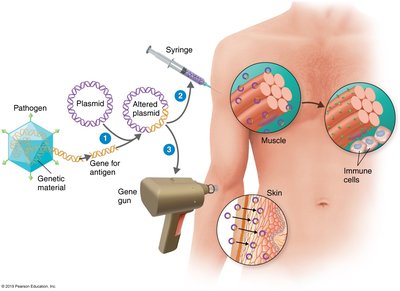
Nucleic acid (DNA) vaccines: Inject DNA encoding antigen into host cells, which then produce the antigen and stimulate immunity.
CDC-Recommended Vaccines to Prevent Bacterial Diseases
Disease(s) | Vaccine | Recommendation | Booster |
|---|---|---|---|
Haemophilus influenzae type b meningitis | Polysaccharide from H. influenzae type b | Children 2–18 months | None recommended |
Meningococcal meningitis | Purified polysaccharide from Neisseria meningitidis | For people with substantial risk | Not established |
Pneumococcal pneumonia | Purified polysaccharide from 13 or 23 strains of Streptococcus pneumoniae | PPSV for adults with chronic diseases; PCV13 for children 2–59 months | None if first dose administered at 2–4 months |
Tetanus, diphtheria, pertussis | DTP (children), Tdap (older children, adults) | DTP: 2, 4, 6 months; Tdap: 11–12 years, adults | Td or Tdap every 10 years |

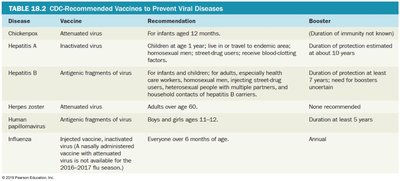
CDC-Recommended Vaccines to Prevent Viral Diseases
Disease(s) | Vaccine | Recommendation | Booster |
|---|---|---|---|
Chickenpox | Attenuated virus | Infants after 12 months | Duration of immunity not known |
Hepatitis A | Inactivated virus | Children at age 1 year, travelers, high-risk groups | About 10 years |
Hepatitis B | Antigenic fragments of virus | Infants, children, adults at risk | At least 7 years |
Herpes zoster | Attenuated virus | Adults over 60 years | None recommended |
Human papillomavirus | Antigenic fragments of virus | Boys and girls 11–12 years | At least 5 years |
Influenza | Inactivated/recombinant virus | Everyone over 6 months | Annual |

Vaccine Development and Technologies
Vaccine development is less profitable than medicines and often requires host animals for growth.
Recombinant and nucleic acid vaccines can be produced without animal cells; plants are being explored as sources.
Oral vaccines are more effective for pathogens entering via mucous membranes and do not require needles.
Technologies include nanopatches (dry vaccine delivery to skin, no refrigeration needed) and multiple-combination vaccines (e.g., MMR plus varicella in one shot).
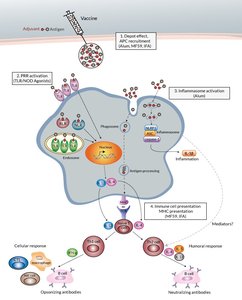
Adjuvants
Adjuvants are chemical additives that enhance vaccine effectiveness.
In the U.S., only alum (aluminum salts) and a lipid A derivative are approved; others are used in Europe.
They likely work by activating Toll-like receptors, but mechanisms are not fully understood.
Vaccine Safety
Vaccines are among the safest and most effective means of preventing infectious diseases in children.
Rarely, vaccines can cause disease, but there is no scientific evidence linking MMR vaccines to autism.
Diagnostic Immunology
Principles of Diagnostic Immunology
Immunological tests are highly specific due to the precise nature of antibody-antigen interactions.
These reactions are used to detect the presence of antibodies or antigens in patient samples.
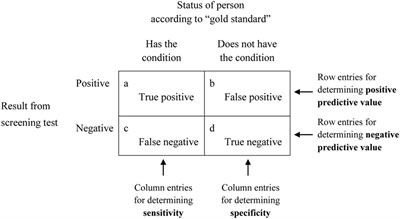
Sensitivity and Specificity
Sensitivity: Probability that a test is reactive if the specimen is a true positive.
Specificity: Probability that a test is not reactive if the specimen is a true negative.
Immunologic-Based Diagnostic Tests
Use antibody-antigen interactions in blood samples.
Known antibodies can identify unknown pathogens, and known pathogens can identify unknown antibodies.
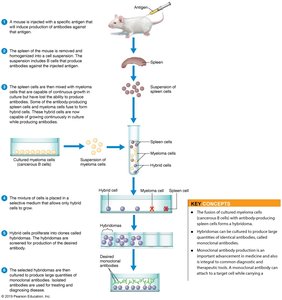
Monoclonal Antibodies (Mab)
Produced from a single B cell clone, so all antibodies are specific to one epitope.
Can be made in mice, but mouse antibodies may cause issues in humans; chimeric Mabs (90% human, 10% mouse) are used to reduce this.
Highly specific, uniform, and can be mass-produced.
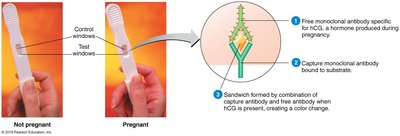
Applications: diagnostic tools, serological identification, pregnancy tests, and therapies for diseases like MS, Crohn’s, cancer, asthma, and arthritis.
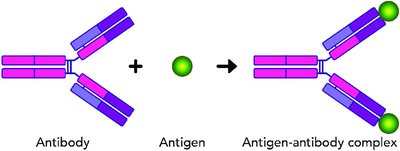
Agglutination Reactions
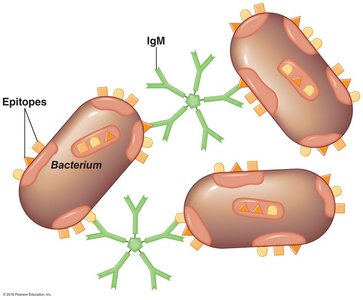
Principles
Antigens bind to antibodies, forming visible clumps (agglutination).
Used to diagnose diseases by combining patient serum with known antigens and observing for agglutination.
Rising antibody titer in serum indicates infection.

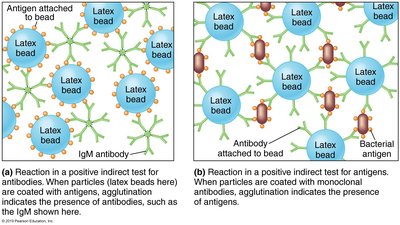
Types of Agglutination Tests
Direct agglutination: Antibodies bind directly to large antigens.
Indirect (passive) agglutination: Small antigens are attached to latex beads to enhance visibility.
Hemagglutination: Agglutination of red blood cells, used in blood typing.
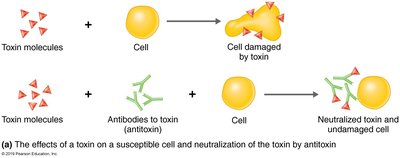
Neutralization Reactions
Principles
Antibodies (antitoxins) neutralize the harmful effects of exotoxins or viruses.
Used to diagnose and treat diseases like botulism, tetanus, and diphtheria.
Enzyme-Linked Immunosorbent Assay (ELISA)
Principles and Applications
Most widely used enzyme immunoassay; easy to read and rapid.
Applications: rapid strep test, home pregnancy tests, urine drug tests.
Highly sensitive with clear positive or negative results.
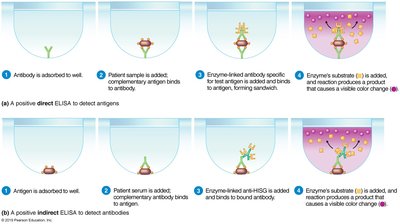
Types of ELISA
Direct ELISA: Detects antigens using enzyme-linked antibodies; color change indicates presence of antigen.
Indirect ELISA: Detects antibodies; antigen is bound in the test well, and patient serum is added.
Summary Table: Types of Vaccines
Type | Example | Key Features |
|---|---|---|
Live attenuated | MMR, Varicella | Strong, lifelong immunity; risk for immunocompromised |
Inactivated | Polio (Salk), Influenza | Safer, requires boosters |
Subunit | Hepatitis B | Fewer side effects, highly specific |
Toxoid | Tetanus, Diphtheria | Inactivated toxins, require boosters |
Conjugated | Hib | Enhanced response in children |
Nucleic acid | Experimental | Induces both humoral and cellular immunity |
