 Back
BackPrinciples of Disease and Epidemiology: Microbiology Study Guide
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Pathology, Infection, and Disease
Pathology is the scientific study of disease, including its causes, development, and effects on the body. Understanding the terminology is essential for microbiology students.
Pathology: The study of disease.
Etiology: The cause of a disease.
Pathogenesis: The manner in which a disease develops.
Infection: Invasion or colonization of the body by pathogens.
Infectious disease: Occurs when an infection results in any change in the state of health.
Infections may exist without detectable disease, and disease can occur when microorganisms colonize areas where they are not normally found.
The Human Microbiome
The human microbiome consists of the collection of microorganisms that inhabit the human body. It is acquired before birth and continues to develop throughout life, influenced by various environmental and physiological factors.
Acquisition: Begins in utero, with placental microbiome and colonization during birth (e.g., Lactobacilli during vaginal birth).
Normal microbiota: Permanently colonize the host and do not cause disease under normal conditions.
Transient microbiota: Present temporarily and then disappear.
Factors influencing microbiota: Nutrients, physical/chemical factors, mechanical factors, body defenses, age, diet, hygiene, geography, lifestyle.
Normal microbiota play a crucial role in immune system development and health.
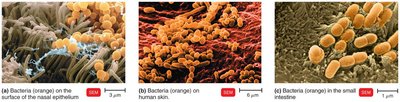
Representative Normal Microbiota by Body Region
Microbiota composition varies by body region, influenced by local conditions.
Region | Principal Components | Comments |
|---|---|---|
Skin | Propionibacterium, Staphylococcus, Corynebacterium, Micrococcus, Acinetobacter, Brevibacterium, Candida, Malassezia | Antimicrobial properties of skin secretions; low pH and moisture inhibit many microbes. |
Eyes (Conjunctiva) | Staphylococcus epidermidis, S. aureus, diphtheroids, Propionibacterium, Corynebacterium, streptococci, Micrococcus | Tears and blinking eliminate/inhibit microbes; lysozyme is antimicrobial. |
Nose and Throat | S. aureus, S. epidermidis, aerobic diphtheroids, Streptococcus pneumoniae, Haemophilus, Neisseria | Microbial antagonism reduces pathogenicity; mucus and ciliary action remove microbes. |
Mouth | Streptococcus, Lactobacillus, Actinomyces, Bacteroides, Veillonella, Neisseria, Haemophilus, Fusobacterium, Treponema, Staphylococcus, Corynebacterium, Candida | Moisture and food support diverse populations; saliva contains antimicrobial substances. |
Large Intestine | E. coli, Bacteroides, Fusobacterium, Lactobacillus, Enterococcus, Bifidobacterium, Enterobacter, Citrobacter, Proteus, Klebsiella, Candida | Largest numbers due to moisture/nutrients; microbial antagonism prevents pathogen growth. |
Urinary and Genital Systems | Staphylococcus, Micrococcus, Enterococcus, Lactobacillus, Bacteroides, aerobic diphtheroids, Pseudomonas, Klebsiella, Proteus, Clostridium, Candida, Trichomonas vaginalis | Acid-tolerant populations; urine flow and acidity inhibit microbes. |
Microbiome and Birth
The mode of birth influences the initial microbiome:
Vaginal birth: Lactobacillus and Bacteroides are prevalent.
Cesarean birth: Microbiome resembles human skin, with Staphylococcus aureus common.
Relationships Between Microbiota and Host
Microbial antagonism and symbiosis describe interactions between microbiota and the host.
Microbial antagonism: Competition between microbes; normal microbiota protect the host by competing for nutrients, producing harmful substances, and affecting pH/oxygen.
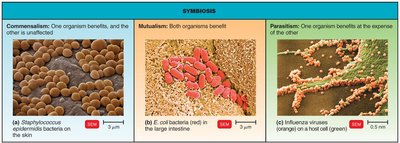
Symbiosis: Relationship where at least one organism depends on the other.
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit.
Parasitism: One organism benefits at the expense of the other.
Opportunistic pathogens: Normal microbiota that cause disease under certain conditions.
The Etiology of Infectious Diseases
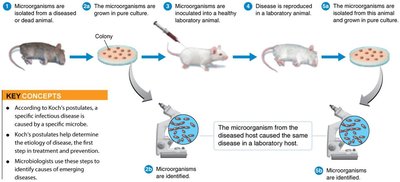
Koch’s Postulates
Koch’s postulates are a set of criteria used to establish the causative relationship between a microbe and a disease.
The same pathogen must be present in every case of the disease.
The pathogen must be isolated from the diseased host and grown in pure culture.
The pathogen from the pure culture must cause the disease when inoculated into a healthy, susceptible laboratory animal.
The pathogen must be isolated from the inoculated animal and shown to be the original organism.
Exceptions include pathogens that cause multiple diseases, those only infecting humans, unculturable microbes, and diseases with similar signs caused by different pathogens.
Classifying Infectious Diseases
Symptoms, Signs, and Syndromes
Diseases are classified based on their communicability, frequency, and severity.
Symptoms: Subjective changes felt by the patient.
Signs: Objective changes measurable or observable.
Syndrome: Specific group of signs and symptoms accompanying a disease.
Communicable vs. Noncommunicable Diseases
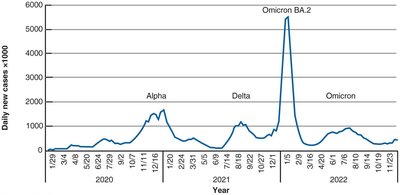
Communicable disease: Spread from one host to another (e.g., COVID-19, influenza).
Contagious disease: Easily and rapidly spread.
Noncommunicable disease: Not spread from host to host (e.g., tetanus).
Occurrence of Disease
Incidence: Number of new cases during a specific time period.
Prevalence: Total number of cases at a specified time, including old and new cases.
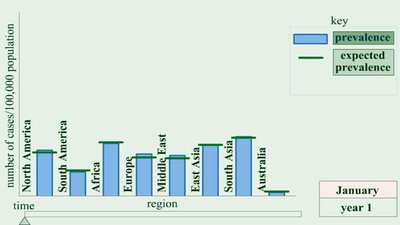
Frequency and Severity of Disease
Sporadic disease: Occurs occasionally.
Endemic disease: Constantly present in a population.
Epidemic disease: Acquired by many people in a short time.
Pandemic disease: Worldwide epidemic.
Severity or Duration of Disease
Acute disease: Rapid onset, short duration.
Chronic disease: Slow development, long duration.
Subacute disease: Intermediate between acute and chronic.
Latent disease: Inactive for a time, then activates.
Herd immunity: Immunity in most of a population.
Extent of Host Involvement
Local infection: Limited to a small area.
Systemic infection: Spread throughout the body.
Focal infection: Systemic infection that began as a local infection.
Sepsis: Toxic inflammatory condition from spread of microbes or toxins.
Bacteremia: Bacteria in the blood.
Septicemia: Growth of bacteria in the blood.
Toxemia: Toxins in the blood.
Viremia: Viruses in the blood.
Primary infection: Initial acute infection.
Secondary infection: Opportunistic infection after primary infection.
Subclinical infection: No noticeable signs or symptoms.
Patterns of Disease
Predisposing Factors
Factors that increase susceptibility to disease or alter its course include nutrition, sex, genetics, climate, environment, vaccination, age, lifestyle, and compromised host status.
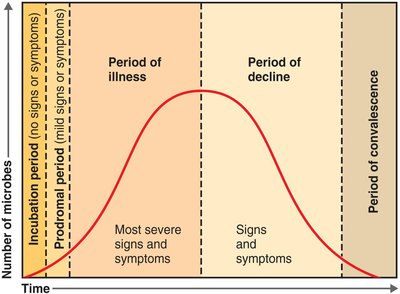
Development of Disease
Incubation period: Interval between infection and first symptoms.
Prodromal period: Early, mild symptoms.
Period of illness: Most severe symptoms.
Period of decline: Symptoms subside.
Period of convalescence: Recovery and return to health.

The Spread of Infection
Reservoirs of Infection
Reservoirs are continual sources of infection and include human, animal, and nonliving sources.
Human reservoirs: People with symptoms or carriers (asymptomatic, incubating, convalescent, chronic, passive).
Animal reservoirs: Zoonoses are diseases transmitted from animals to humans.
Nonliving reservoirs: Soil, water, and foods.
Transmission of Disease
Contact transmission: Direct (physical contact), indirect (fomites), droplet (airborne droplets <1 meter).
Vehicle transmission: Transmission by inanimate reservoirs (air, water, food).
Vector transmission: Arthropods transmit disease mechanically (on feet) or biologically (pathogen reproduces in vector).



Healthcare-Associated Infections (HAIs)
Definition and Importance
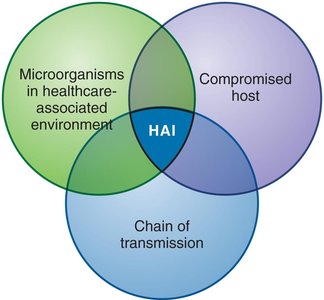
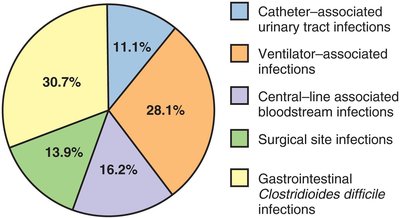
HAIs, also known as nosocomial infections, are acquired during treatment in healthcare facilities. They affect a significant proportion of patients and are a major public health concern.
Sources: Hospital environment, compromised hosts, chain of transmission.
Compromised host: Resistance impaired by disease, therapy, or burns.
Control and Prevention
Universal precautions: Reduce transmission in healthcare settings.
Standard precautions: Hand hygiene, PPE, respiratory hygiene, disinfection, safe practices.
Transmission-based precautions: Contact, droplet, and airborne precautions.
Reduce pathogens: Handwashing, cleaning, disposable equipment.
Improve resistance: Judicious antibiotic use, avoid invasive procedures.
Infection control committees: Monitor and oversee infection control.
Emerging Infectious Diseases
Definition and Contributing Factors
Emerging infectious diseases are new, changing, or increasing in incidence. Most are zoonotic and vector-borne.
Genetic recombination: e.g., E. coli O157:H7, avian influenza.
Evolution of organisms: e.g., Vibrio cholerae O139.
Antibiotic/pesticide use: Antibiotic-resistant strains.
Genetic instability: RNA viruses, antigenic shift/drift.
Climate/weather changes: e.g., Hantavirus.
Modern transportation: e.g., Zika virus.
Ecological disaster/war: e.g., Coccidioidomycosis.
Animal control measures: e.g., Lyme disease.
Public health failure: e.g., Diphtheria.
Bioterrorism: Deliberate spread of pathogens.
Epidemiology
Definition and Types
Epidemiology is the study of where and when diseases occur and how they are transmitted in populations. It includes descriptive, analytical, and experimental investigations.
Descriptive epidemiology: Collection and analysis of data (e.g., John Snow's cholera investigation).
Analytical epidemiology: Determines probable cause/risk factors (e.g., Florence Nightingale).
Experimental epidemiology: Hypothesis and controlled experiments (e.g., Ignaz Semmelweis).
Roles and Functions
Determine etiology of disease.
Identify factors and patterns in disease spread.
Assemble data and graphs to outline incidence.
Predict probability of infection spread ( reproductive number).
Explore methods for disease control.
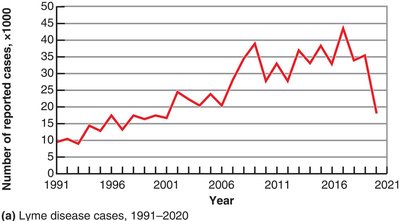
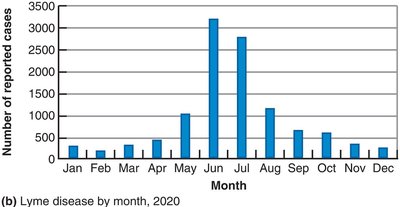
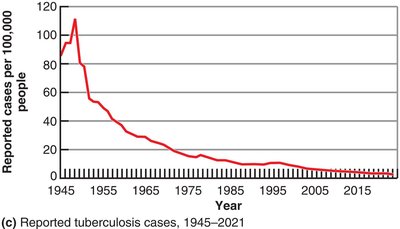
Case Reporting and CDC
Case reporting: Health workers report specified diseases to officials; enables tracking and outbreak warning.
CDC: Collects and analyzes epidemiological information; publishes Morbidity and Mortality Weekly Report (MMWR).
Morbidity: Incidence of a specific notifiable disease.
Mortality: Deaths from notifiable diseases.
Morbidity rate: Number affected relative to population.
Mortality rate: Number of deaths relative to population.
Additional info: All images included are directly relevant to the adjacent paragraphs and reinforce key microbiological concepts.
