 Back
BackPrinciples of Disease and Epidemiology: Mini-Textbook Study Notes
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Introduction to Disease and Pathogenesis
The study of disease in microbiology focuses on how microbes cause disease, how infections develop, and the factors influencing disease spread. Understanding these principles is essential for controlling infectious diseases and improving public health.
Pathogen: A disease-causing microbe.
Pathogenesis: The process by which a disease develops.
Infection: The growth of microbes in or on the body.
Virulence: The degree of pathogenicity or aggressiveness of a microbe.
Disease: Can occur when microbes are found in parts of the body where they are not normally present (e.g., Escherichia coli in the urinary tract).
Normal Microbiota and the Host
Normal Microbiota (Microflora)
Normal microbiota are the permanent, beneficial microbial residents of specific body sites. They play a crucial role in health by providing protection and aiding in physiological functions.
Permanent residents of specific body parts (e.g., skin, gut).
Engage in a symbiotic relationship with the host, often providing protection in exchange for nutrients.
Example: E. coli produces vitamin K in the gut.
Can cause disease if displaced to other body sites (e.g., urinary tract infection).
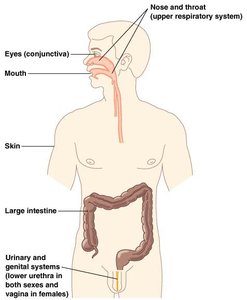
Acquisition and Importance of Normal Microbiota
Humans are germ-free in utero; colonization begins during and after birth.
Greatest numbers found in the large intestine.
Colonization stages: Lactobacilli (from vaginal birth) → E. coli → complex flora after dietary changes.
Normal microbiota are essential for health; germ-free organisms are less healthy.
Types of Symbiotic Relationships
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit (e.g., protection from pathogens).
Parasitism: One benefits at the expense of the other, often causing disease.
Opportunism: Microbes cause disease only under certain conditions (e.g., weakened host).
Microbial Antagonism and Probiotics
Microbial antagonism: Competition between microbes; normal microbiota protect the host by occupying niches, producing acids, and bacteriocins.
Probiotics: Live microbes ingested or applied to exert beneficial effects (e.g., lactic acid bacteria).
Opportunistic Pathogens and Nosocomial Infections
Opportunistic pathogen: Causes disease in weakened hosts (e.g., Pseudomonas aeruginosa in hospitals).
Nosocomial infections: Hospital-acquired infections, often due to compromised immunity.
Koch’s Postulates and Disease Causation
Koch’s Postulates
Robert Koch established scientific criteria to link specific microbes to specific diseases, forming the foundation of medical microbiology.
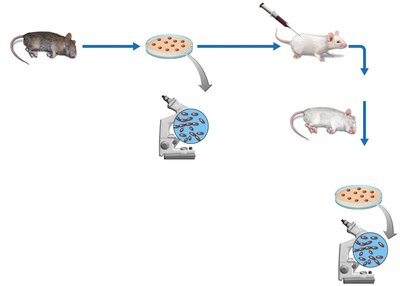
The same organism must be found in all cases of the disease.
The organism must be isolated and grown in pure culture.
The isolated organism must reproduce the disease when inoculated into a healthy animal.
The organism must be re-isolated from the experimentally infected animal.
Classifying Infectious Diseases
Symptoms, Signs, and Syndromes
Symptom: Subjective changes felt by the patient (e.g., pain, malaise).
Sign: Objective, measurable changes (e.g., fever, rash).
Syndrome: A specific group of symptoms or signs that always accompany a disease.
Types of Infectious Diseases
Communicable disease: Spread from one host to another.
Contagious disease: Easily spread from host to host (e.g., chickenpox).
Noncommunicable disease: Not transmitted between hosts.
Occurrence of Disease
Incidence: Number of new cases during a specific time period.
Prevalence: Total number of cases (old and new) at a specific time.
Sporadic disease: Occurs occasionally in a population.
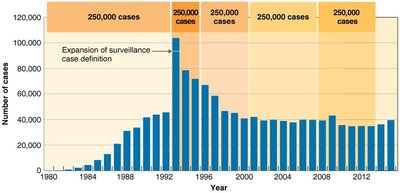
Patterns of Disease Occurrence
Endemic: Constantly present at low levels in a region (e.g., malaria in tropics).
Epidemic: Sudden increase in cases in a region.
Pandemic: Worldwide epidemic (e.g., influenza).
Emerging infectious disease: Newly identified or increasing in incidence.
Herd immunity: Immunity in most of a population, reducing disease spread.
Severity and Duration of Disease
Acute: Rapid onset, short duration (e.g., influenza).
Chronic: Slow onset, long duration (e.g., tuberculosis).
Subacute: Intermediate between acute and chronic.
Latent: Inactive for a period, can reactivate (e.g., herpes simplex, HIV).
Extent of Host Involvement
Local infection: Confined to a specific area (e.g., conjunctivitis).
Systemic infection: Microbes or toxins spread throughout the body (e.g., measles).
Focal infection: Systemic infection that began as a local infection.
Sepsis: Toxic inflammatory condition from microbe spread.
Bacteremia: Bacteria in the blood.
Septicemia: Growth of bacteria in the blood.
Primary infection: Acute infection causing initial illness.
Secondary infection: Caused by opportunistic microbe after primary infection weakens host.
Subclinical infection: No noticeable symptoms, but organism can be transmitted.
Predisposing Factors
Short urethra in females
Inherited traits (e.g., sickle-cell gene)
Climate and weather
Fatigue, age, lifestyle, chemotherapy
Stages of Disease
Progression of Disease
Incubation period: Time between infection and appearance of symptoms; patient can be infectious.
Prodromal period: Short period of mild symptoms; immune response may halt disease here.
Period of illness: Most severe symptoms; immune system actively fighting infection.
Period of decline: Symptoms subside as pathogen is controlled.
Period of convalescence: Recovery and return to pre-illness health.
Spread of Microbes
Reservoirs of Infection
Reservoir: Source of infectious agent (living or nonliving).
Animal reservoirs: Animals harboring pathogens (e.g., rabies in dogs).
Nonliving reservoirs: Soil, water, food (e.g., botulism, tetanus).
Fomite: Inanimate object transmitting pathogens (e.g., pencil).
Carrier: Asymptomatic individual spreading disease (e.g., HIV, Typhoid Mary).
Routes of Transmission
Contact transmission:
Direct: Person-to-person (e.g., STDs, handshake).
Indirect: Via fomites (e.g., contaminated objects).
Droplet: Short distance (<1 m), e.g., sneezing.


Vehicle transmission: Transmission by a medium (food, water, air).
Waterborne: Contaminated water (e.g., cholera).
Foodborne: Contaminated food (e.g., Salmonella).
Airborne: Microbes in dust or droplets over long distances (e.g., TB).

Vector transmission: Animals or insects transmit pathogens.
Mechanical: Pathogen carried on body (e.g., flies).
Biological: Pathogen lives/reproduces in vector (e.g., malaria in mosquitoes).

Vertical transmission: Mother to offspring (transplacental, perinatal, breastfeeding).
Horizontal transmission: Person to person (contact, vehicle, airborne, vector-borne).
Control of Disease Spread
Hygiene (personal and public)
Control of vectors (e.g., mosquito nets, pet vaccination)
Avoiding contact with carriers/infected individuals
Isolation and quarantine (e.g., for tuberculosis)
Nosocomial (Healthcare-Associated) Infections
Infections acquired in healthcare settings are a major concern due to the vulnerability of patients and the presence of antibiotic-resistant bacteria.
Common sources: surgery, catheters, direct contact with staff/patients.
Compromised hosts are most susceptible.
CDC estimates 2 million cases/year in the US, with about 90,000 deaths.
Type of Infection | Percentage |
|---|---|
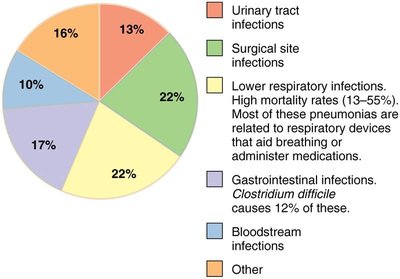
Urinary tract infections | 13% |
Surgical site infections | 22% |
Lower respiratory infections | 22% |
Gastrointestinal infections | 17% |
Bloodstream infections | 10% |
Other | 16% |
Control of Nosocomial Infections
Universal precautions (standard and transmission-based)
Handwashing, cleaning instruments, disposable supplies
Infection control committees
Emerging Infectious Diseases
Diseases that are new, increasing, or likely to increase in incidence.
Contributing factors: new strains, antibiotic misuse, climate change, travel, ecological changes, public health failures.
Epidemiology
Definition and Importance
Epidemiology is the study of where and when diseases occur and how they are transmitted in populations. Epidemiologists identify causes, risk factors, and methods for disease control.
Determine etiology (cause) of disease
Identify factors in disease spread
Develop control methods
Assemble and analyze data (e.g., incidence, prevalence)
Historical Figures in Epidemiology
John Snow: Mapped cholera outbreaks in London (1848-1849).
Ignaz Semmelweis: Demonstrated handwashing reduced puerperal sepsis (1846-1848).
Florence Nightingale: Showed improved sanitation reduced epidemic typhus (1858).
