 Back
BackPrinciples of Disease and Epidemiology: Mini-Textbook Study Guide
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Symbiotic Relationships
Symbiosis refers to the biological interactions between two different organisms or species. These relationships are fundamental to understanding how microorganisms interact with their hosts, including humans.
Mutualism: Both organisms benefit from the relationship. Example: Escherichia coli in the human gut produces vitamins for the host and receives nutrients.
Commensalism: One organism benefits, while the other is unaffected. Example: Skin bacteria that live on human skin without causing harm.
Parasitism: One organism benefits at the expense of the other, often causing harm. All pathogens are considered parasites.
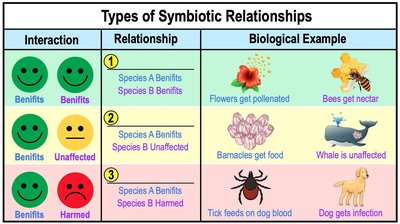
Interaction | Relationship | Biological Example |
|---|---|---|
Benefits / Benefits | Species A Benefits, Species B Benefits | Flowers get pollinated, Bees get nectar |
Benefits / Unaffected | Species A Benefits, Species B Unaffected | Barnacles get food, Whale is unaffected |
Benefits / Harmed | Species A Benefits, Species B Harmed | Tick feeds on dog blood, Dog gets infection |
The Human Microbiome
The human microbiome consists of communities of microbes that inhabit the body. These microbes live in symbiotic relationships with humans and are classified as resident or transient microbiota.
Resident Microbiota: Microbes that persist on/in the host for extended periods.
Transient Microbiota: Microbes that are only temporarily found in the body, often including pathogens.

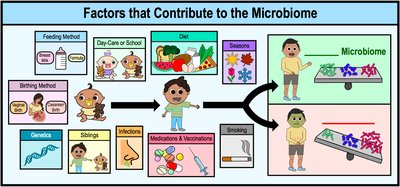
Factors Influencing the Microbiome
Many factors contribute to the composition and diversity of the human microbiome, including birth method, feeding, genetics, environment, diet, and exposure to infections or medications.
Birth method (vaginal vs. cesarean)
Feeding method (breast milk vs. formula)
Diet, siblings, daycare/school, seasons
Medications, vaccinations, infections
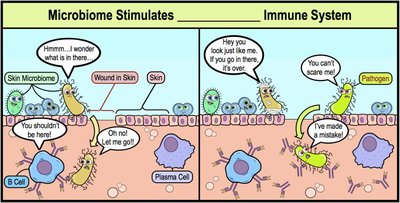
Microbiome and Immunity
The microbiome is part of innate immunity, creating a competitive environment for pathogens and stimulating the immune system.
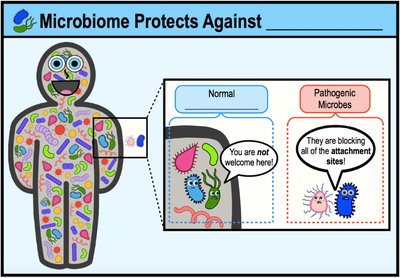
Microbes block attachment sites for pathogens.
Microbiome can stimulate the adaptive immune system, leading to antibody production.
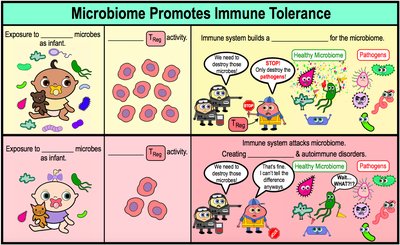
Immune Tolerance and the Hygiene Hypothesis
Immune tolerance is the ability of the immune system to distinguish harmless from harmful microbes. Early exposure to microbes increases regulatory T cell (TReg) activity, reducing the risk of allergies and autoimmune disorders.
Insufficient exposure to microbes increases allergy and autoimmune risk (hygiene hypothesis).
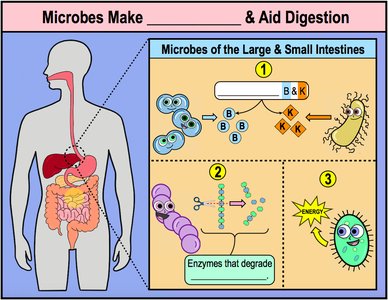
Microbiome and Digestion
The intestinal microbiome produces essential vitamins (B and K), enzymes that degrade complex carbohydrates, and energy sources for epithelial cells.
Humans lack enzymes to digest certain fibers; gut bacteria provide this function.
Characteristics of Infectious Disease
Definitions
Disease: Condition where normal structure and function of a host is impaired.
Infection: Colonization and replication of a pathogen in a host.
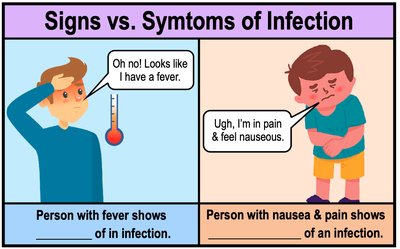
Infectious Disease: Disease caused by infection, resulting in observable signs and symptoms.
Signs: Objective evidence of infection (e.g., fever, rash).
Symptoms: Subjective evidence (e.g., pain, nausea).
Asymptomatic Disease: Infection without observable signs or symptoms.

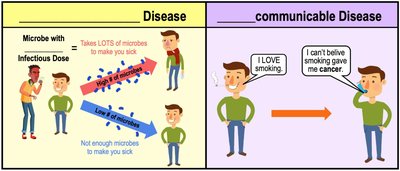
Communicable vs. Noncommunicable Diseases
Communicable Diseases: Infectious diseases that spread between hosts.
Noncommunicable Diseases: Diseases that do not spread between hosts (e.g., cancer).
Infectious Dose: Number of microbes required to establish infection.
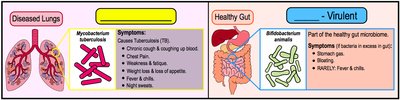
Virulence and Pathogenicity
Virulence: Degree of pathogenicity of an organism.
Virulence Factors: Traits that allow an organism to cause disease (e.g., adhesins, capsules, toxins).
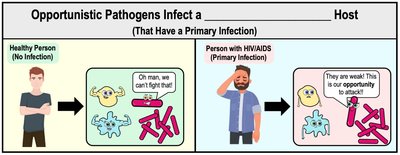
Primary vs. Secondary Infections
Primary Infection: Initial infection caused by a primary pathogen.
Secondary Infection: Subsequent infection caused by opportunistic pathogens in a compromised host.
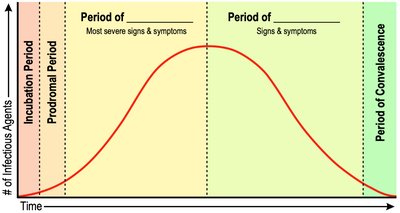
Stages of Infectious Disease Progression
Acute infectious diseases progress through several stages:
Incubation Period: Time between pathogen introduction and appearance of symptoms.
Prodromal Period: Early, vague symptoms.
Period of Illness: Most severe signs and symptoms.
Period of Decline: Signs and symptoms decrease.
Period of Convalescence: Recovery and elimination of pathogen.
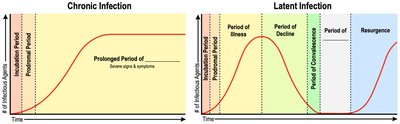
Chronic and Latent Infections
Chronic Infection: Prolonged period of illness.
Latent Infection: Periods of latency and resurgence (e.g., herpes viruses).
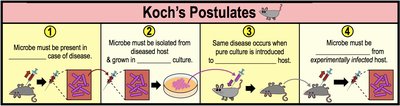
Koch's Postulates
Classical Koch's Postulates
Robert Koch developed four postulates to identify the causative agent of a disease:
The same microbe must be present in every case of the disease.
The microbe must be isolated and grown in pure culture.
The pure culture must cause the disease when introduced into a healthy host.
The microbe must be re-isolated from the experimentally infected host.

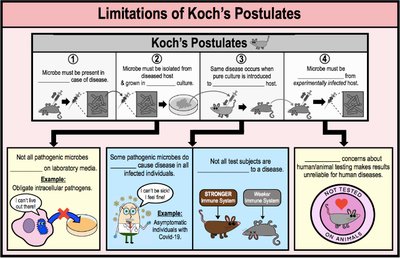
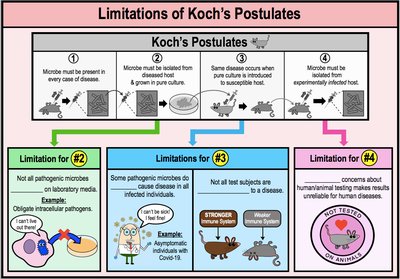
Limitations of Koch's Postulates
Not all pathogens can be cultured in the laboratory.
Some diseases are caused by multiple pathogens or have asymptomatic carriers.
Not all test subjects are susceptible to the disease.
Ethical concerns with human/animal testing.
Epidemiology
Introduction to Epidemiology
Epidemiology is the study of the distribution, patterns, and determinants of health and disease in populations. It includes concepts such as etiology (origin of disease), endemic, epidemic, outbreak, and pandemic.
Endemic: Disease consistently present in a population.
Epidemic: Unusually high number of cases in a population.
Pandemic: Epidemic that spreads worldwide.
Sporadic Disease: Occasional cases in isolated groups.
Morbidity: Incidence vs. Prevalence
Incidence: Number of new cases in a population during a specific time period.
Prevalence: Total number of cases (new and pre-existing) at a specific time.
Incidence Proportion Formula:
Prevalence Proportion Formula:
Mortality & Case-Fatality Rates
Mortality Rate: Proportion of deaths among the entire population.
Case-Fatality Rate (CFR): Proportion of deaths among diagnosed individuals.
Mortality Rate Formula:
Case-Fatality Rate Formula:
Chain of Infection
The spread of infectious disease follows a series of steps known as the chain of infection:
Pathogen in its natural habitat (reservoir)
Portal of exit
Transmission
Portal of entry
Colonization of susceptible host
Reservoirs of Infection
Human Reservoirs: Can be active or passive carriers.
Non-Human Reservoirs: Animals, environmental sources (water, soil).
Zoonoses: Diseases originating in animals and transmitted to humans.
Disease Transmission
Vertical Transmission: Direct transfer from mother to offspring.
Horizontal Transmission: Any other method (direct or indirect).
Direct Transmission: Physical contact or droplet transmission.
Indirect Transmission: Airborne, vehicle-borne, or vector-borne.
Mechanical vs. Biological Vectors
Mechanical Vector: Passively transports pathogen without replication.
Biological Vector: Pathogen replicates within the vector before transmission.
Colonization of Susceptible Host
Pathogen gains access via specific portals of entry (e.g., respiratory, gastrointestinal, skin wounds).
Successful colonization depends on entry point and host susceptibility.
Factors Influencing Epidemiology
Host-microbe interactions
Dose of pathogen
Incubation period
Host population characteristics
Environment
Herd immunity
Emerging and Re-Emerging Infectious Diseases
Emerging Infectious Disease: New or recently increasing in incidence/spread.
Re-Emerging Infectious Disease: Previously controlled, now prevalent again.
Factors: Microbe evolution, population increase, food production, misuse of antibiotics, climate change, societal changes.
Healthcare-Associated Infections (HAIs)
Infections acquired in healthcare settings.
Risk factors: Other patients, hospital environment, workers, visitors, invasive procedures.
Prevention: Infection control committees and practitioners, national guidelines.
Epidemiological Studies
Descriptive: Patterns of who, where, and when.
Analytical: Observational comparison to find associations.
Experimental: Intervention to determine effectiveness.
