 Back
BackPrinciples of Disease and Epidemiology: Pathology, Infection, and Disease
Study Guide - Smart Notes

Pathology, Infection, and Disease
Key Terminology and Concepts
Understanding the principles of disease and epidemiology requires familiarity with foundational terms and concepts in microbiology. These terms help describe the interactions between microbes and their hosts, as well as the mechanisms and patterns of disease spread.
Pathology: The scientific study of disease, including its causes, development, and effects on the body.
Disease: An abnormal state in which the body is not functioning normally.
Etiology: The study of the cause of a disease.
Infection: Colonization of the body by pathogens.
Normal Microbiota and Symbiosis
The human body is colonized by a diverse array of microorganisms, collectively known as the normal microbiota. These microbes play essential roles in health and disease, often forming complex relationships with their host.
Normal microbiota: Microorganisms that permanently colonize the host without causing disease under normal conditions.
Transient microbiota: Microbes that are present for a short period (days, weeks, or months).
Probiotics: Live microbes ingested or applied to the body to confer a health benefit.
Symbiosis: The relationship between normal microbiota and the host, which can be classified as:
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit.
Parasitism: One organism benefits at the expense of the other.
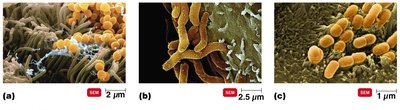
Distribution and Composition of Normal Microbiota
The composition of the normal microbiota is influenced by several factors, including nutrient availability, physical and chemical conditions, host defenses, and mechanical factors. These microbes occupy niches that might otherwise be taken by pathogens, providing protection through microbial antagonism (competition between microbes).
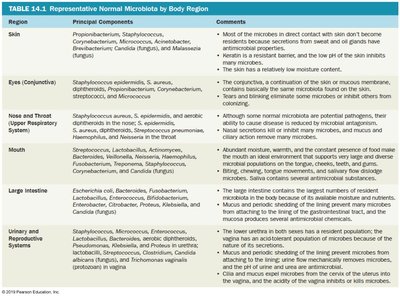
Representative Normal Microbiota by Body Region
Region | Principal Components | Comments |
|---|---|---|
Skin | Propionibacterium, Staphylococcus, Corynebacterium, Micrococcus, Acinetobacter, Brevibacterium, Candida (fungus), Malassezia (fungus) | Most skin microbes do not become residents due to secretions and the dry, salty environment. Keratin and low moisture content inhibit many microbes. |
Eyes (Conjunctiva) | Staphylococcus epidermidis, S. aureus, diphtheroids, Propionibacterium, Streptococcus, Micrococcus | The conjunctiva is a continuation of the skin/mucous membrane; tears and blinking eliminate microbes. |
Nose and Throat (Upper Respiratory System) | Staphylococcus aureus, S. epidermidis, aerobic diphtheroids, Streptococcus pneumoniae, Haemophilus, Neisseria | Some are potential pathogens; mucus and ciliary action remove many microbes. |
Mouth | Streptococcus, Lactobacillus, Actinomyces, Bacteroides, Veillonella, Neisseria | Abundant moisture and food; biting, chewing, and saliva dislodge microbes. |
Large Intestine | Escherichia coli, Bacteroides, Fusobacterium, Enterococcus, Clostridium, Candida (fungus) | Largest microbial population; mucus and shedding of lining cells remove microbes. |
Urinary and Reproductive Systems | Staphylococcus, Micrococcus, Enterococcus, Lactobacillus, Streptococcus, Mycobacterium, Bacteroides, Aerococcus, Candida (fungus) | Urine flow and vaginal secretions remove microbes; acidity of urine and vagina inhibits microbes. |

Koch’s Postulates and the Etiology of Disease
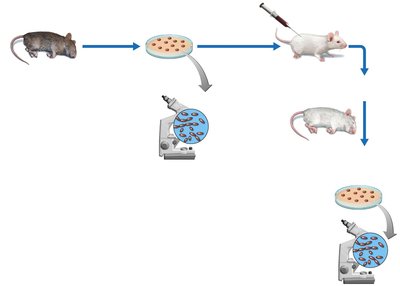
Koch’s Postulates
Koch’s postulates are a set of criteria used to establish a causative relationship between a microbe and a disease. They are fundamental to the study of infectious diseases.
The same pathogen must be present in every case of the disease.
The pathogen must be isolated from the diseased host and grown in pure culture.
The pathogen from the pure culture must cause the disease when inoculated into a healthy, susceptible laboratory animal.
The pathogen must be re-isolated from the inoculated animal and shown to be the original organism.
Classifying Infectious Diseases
Symptoms, Signs, and Syndromes
Diseases are classified based on their observable and subjective effects on the host.
Symptom: A change in body function felt by the patient (e.g., nausea).
Sign: A change that can be measured or observed (e.g., fever).
Syndrome: A specific group of signs and symptoms that accompany a disease.

Communicable, Contagious, and Noncommunicable Diseases
Communicable disease: Spread from one host to another (e.g., chickenpox, measles).
Contagious disease: Easily spread from one host to another (e.g., COVID-19).
Noncommunicable disease: Not transmitted from host to host (e.g., tetanus).
Occurrence of Disease: Incidence and Prevalence
Understanding how diseases spread and persist in populations requires knowledge of incidence and prevalence.
Incidence: Fraction of a population that contracts a disease during a specific time (new cases).
Prevalence: Fraction of a population having a specific disease at a given time (existing cases).

Patterns of Disease Occurrence
Sporadic disease: Occurs occasionally (e.g., typhoid fever).
Endemic disease: Constantly present in a population (e.g., common cold).
Epidemic disease: Acquired by many hosts in a short time (e.g., influenza).
Pandemic disease: Worldwide epidemic (e.g., COVID-19).
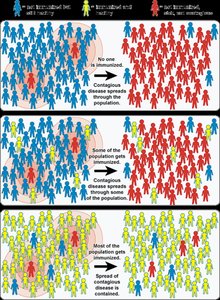
Herd immunity: Immunity in most of the population protects those who are vulnerable.
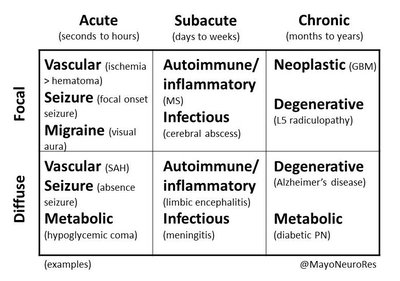
Severity and Duration of Disease
Classification by Severity
Acute disease: Symptoms develop rapidly and last a short time (e.g., influenza).
Chronic disease: Develops slowly, lasts a long time (e.g., tuberculosis).
Subacute disease: Symptoms between acute and chronic.
Latent disease: Period of no symptoms when the causative agent is inactive (e.g., shingles).
Extent of Host Involvement
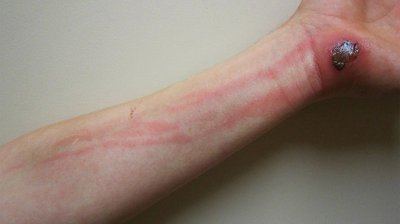
Types of Infections
Local infection: Pathogens are limited to a small area (e.g., boils).
Systemic infection: Infection throughout the body (e.g., measles).
Focal infection: Systemic infection that began as a local infection.
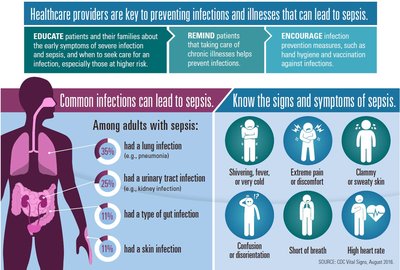
Sepsis and Related Terms
Sepsis: Toxic inflammatory condition from the spread of microbes or their toxins.
Bacteremia: Bacteria in the blood.
Septicemia: Growth of bacteria in the blood (a type of sepsis).
Toxemia: Toxins in the blood (e.g., tetanus).
Viremia: Viruses in the blood (e.g., COVID-19).
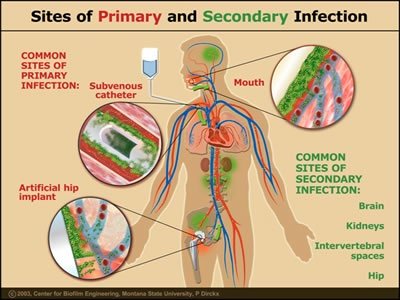
Primary infection: Acute infection causing the initial illness.
Secondary infection: Opportunistic infection after a primary infection.
Subclinical disease: No noticeable signs or symptoms (e.g., poliovirus).
Predisposing Factors
Predisposing factors make the body more susceptible to disease. These include anatomical differences (e.g., short urethra in females), inherited traits, climate, fatigue, age, lifestyle, and medical treatments such as chemotherapy.
Reservoirs and Transmission of Disease
Reservoirs of Infection
Human reservoirs: Carriers may have unapparent infections or latent diseases (e.g., AIDS).
Animal reservoirs: Zoonoses are diseases transmitted from animals to humans (e.g., rabies).
Nonliving reservoirs: Soil and water can harbor pathogens (e.g., tetanus, botulism).

Modes of Disease Transmission
Contact transmission:
Direct contact: Close association between infected and susceptible host.
Indirect contact: Spread by fomites (nonliving objects).
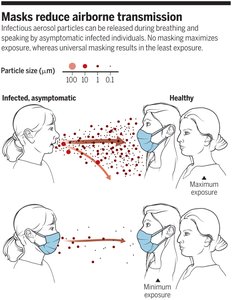
Droplet transmission: Via airborne droplets.
Vehicle transmission: Transmission by an inanimate reservoir (food, water, air).
Vector transmission: Arthropods (e.g., fleas, ticks, mosquitoes) transmit disease by mechanical or biological means.




Nosocomial (Hospital-Acquired) Infections
Overview and Prevention
Nosocomial infections are acquired during hospital stays and affect 5–15% of all hospital patients. They result from the interaction of microorganisms in the hospital environment, a compromised host, and the chain of transmission.

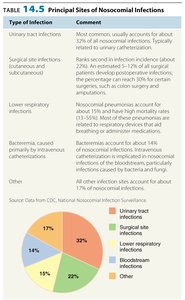
Principal Sites and Causes of Nosocomial Infections
Type of Infection | Comment |
|---|---|
Urinary tract infections | Most common; often related to urinary catheterization. |
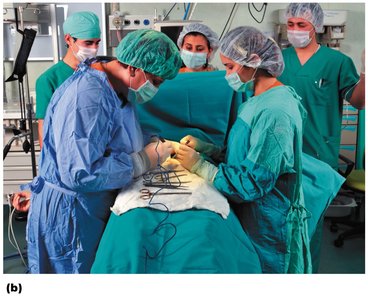
Surgical site infections | Second most common; associated with postoperative infections. |
Lower respiratory infections | Often due to respiratory devices; high mortality rate. |
Bacteremia (catheter-associated) | Bloodstream infections from intravenous catheters. |
Other | Includes gastrointestinal and skin infections. |
Common Pathogens and Resistance
Coagulase-negative staphylococci, S. aureus, Enterococcus, Gram-negative rods, C. difficile
Many are resistant to antibiotics, making treatment challenging.
Clostridium difficile (C. diff) and MRSA
C. diff: Anaerobic, endospore-forming bacterium; survives many antibiotics and can cause severe colitis. Requires strict hygiene and sporocidal disinfectants for control.
MRSA: Methicillin-resistant Staphylococcus aureus; major cause of hospital and community-acquired infections.
Emerging Infectious Diseases
Definition and Contributing Factors
Emerging infectious diseases are those that are new, increasing in incidence, or have the potential to increase soon. Most are zoonotic, viral, and vector-borne.
Genetic recombination and evolution of new strains
Inappropriate use of antibiotics and pesticides
Changes in weather patterns
Modern transportation and ecological changes
Public health failures
Epidemiology
Principles and Methods
Epidemiology is the study of where and when diseases occur and how they are transmitted. It uses descriptive, analytical, and experimental methods to track and control disease spread.
Descriptive: Collection and analysis of data (e.g., John Snow and cholera mapping).
Analytical: Comparison of diseased and healthy groups (e.g., Florence Nightingale).
Experimental: Controlled experiments (e.g., Semmelweis and handwashing).
CDC and Disease Reporting
The Centers for Disease Control and Prevention (CDC) collects and analyzes epidemiological data in the US.
Publishes the Morbidity and Mortality Weekly Report (MMWR).
Morbidity: Incidence of a specific notifiable disease.
Mortality: Deaths from notifiable diseases.
Case reporting is required for nationally notifiable diseases.
