 Back
BackPrinciples of Disease and Epidemiology: Study Notes for Microbiology Students
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Pathology, Infection, and Disease
Pathology is the scientific study of disease, focusing on its causes, development, and effects on the host. Understanding pathology is essential for identifying how diseases originate and progress in the human body.
Etiology: The cause of a disease, often determined by identifying the responsible pathogen.
Pathogenesis: The mechanism by which a disease develops and progresses.
Structural and Functional Changes: Disease leads to observable changes in tissues and organs.
Infection: Invasion or colonization of the body by pathogenic microorganisms.
Disease: An abnormal state in which the body is not functioning normally.
The Human Microbiome
The human microbiome consists of the collection of microorganisms that inhabit various sites in the human body. These microbes play crucial roles in health and disease.
How: Microbiota are acquired through birth, environment, and diet.
When: Colonization begins at birth and continues throughout life.
Where: Microbiota are found on the skin, in the gut, respiratory tract, and other surfaces.
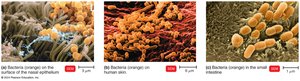
Factors Influencing Normal Microbiota
Several factors affect the composition and function of the normal microbiota.
Nutrient Availability: Microbes require specific nutrients to thrive.
Physical and Chemical Factors: Temperature, pH, and oxygen levels influence microbial growth.
Host Defenses: The immune system regulates microbial populations.
Mechanical Forces: Actions such as chewing, swallowing, and peristalsis affect microbial distribution.
Normal Microbiota and Prevention of Opportunistic Microbes
Normal microbiota protect the host by preventing the growth of opportunistic pathogens.
Nutrient Competition: Microbiota compete for resources, limiting pathogen access.
Secretion of Antimicrobial Substances: Some bacteria produce bacteriocins that inhibit other microbes (e.g., E. coli inhibits Salmonella and Shigella).
Maintaining pH: Microbiota help regulate pH, preventing overgrowth of pathogens (e.g., Candida albicans in vaginitis).
Affecting Oxygen Levels: Microbial activity can alter oxygen availability, influencing pathogen survival.
Relationships Between Microbiota and Host
Microbiota interact with the host in various symbiotic relationships.
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit.
Parasitism: One organism benefits at the expense of the other; many pathogens are parasites.
Opportunistic Pathogens: Some normal microbiota can cause disease under certain conditions.
Etiology and Koch’s Postulates
Koch’s postulates are a set of criteria used to establish the causative relationship between a microbe and a disease.
The same pathogen must be present in every case of the disease.
The pathogen must be isolated from the diseased host and grown in pure culture.
The pathogen from the pure culture must cause the disease when inoculated into a healthy, susceptible laboratory animal.
The pathogen must be isolated from the inoculated animal and shown to be the original organism.
Exceptions to Koch’s Postulates
Some pathogens cause multiple disease conditions.
Some pathogens only infect humans (e.g., HIV).
Some microbes cannot be cultured (e.g., Treponema pallidum, Mycobacterium leprae).
Viruses require host cells for growth.
Different pathogens may cause similar symptoms (e.g., pneumonia).
Symptoms vs Signs
Symptoms and signs are used to describe disease manifestations.
Symptoms: Subjective, not measurable (e.g., pain, fatigue).
Signs: Objective and measurable (e.g., blood pressure, heart rate, temperature).
Classifying Infectious Diseases
Diseases are classified based on their mode of transmission.
Communicable Disease: Spread from one host to another (e.g., COVID-19, influenza).
Contagious Disease: Easily and rapidly spread (e.g., measles).
Noncommunicable Disease: Not spread between hosts (e.g., tetanus).
Occurrence of Disease: Incidence and Prevalence
Incidence and prevalence are epidemiological measures used to describe disease frequency.
Incidence: Number of new cases during a specific time period.
Prevalence: Total number of cases (old and new) at a specific time.
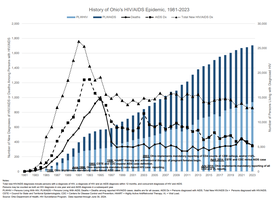
Year-over-Year Trends for Influenza-like Illness (ILI)
Tracking ILI trends helps monitor seasonal and epidemic patterns.

Influenza Positive Tests
Laboratory-confirmed influenza cases are reported to monitor disease activity.
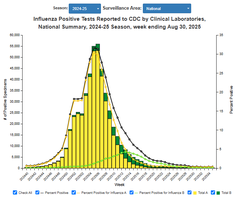
Types of Disease Occurrence
Sporadic Disease: Occurs occasionally.
Endemic Disease: Constantly present in a population.
Epidemic Disease: Acquired by many people in a short time.
Pandemic Disease: Worldwide epidemic.
Duration and Severity of Disease
Diseases vary in duration and severity.
Acute Disease: Rapid onset, short duration (e.g., influenza).
Chronic Disease: Slow onset, long duration (e.g., tuberculosis).
Subacute Disease: Intermediate between acute and chronic.
Latent Disease: Inactive for a time, then activates (e.g., herpes, chicken pox).
Herd Immunity: Immunity in most of a population protects susceptible individuals.
Severity of Disease
Severity is determined by the extent and impact of disease.
Asymptomatic: No signs or symptoms.
Mild: Minor symptoms.
Moderate: More pronounced symptoms.
Severe: Serious complications (e.g., pneumonia).
Critical: Life-threatening (e.g., SARS).
Sepsis: Extreme inflammatory response to infection.
Infection Fatality Ratio (IFR) vs Case Fatality Ratio (CFR)
IFR and CFR are measures of disease lethality.
IFR: Number of deaths divided by total infected individuals (including undiagnosed and asymptomatic cases).
CFR: Proportion of diagnosed cases who die from the disease.
Table: Diseases with High Case Fatality Ratios
Disease | Type | CFR | Treatment |
|---|---|---|---|
Rabies | Viral | >99% | No cure once symptoms manifest |
Tetanus | Bacterial | 40-60% | Unvaccinated and untreated |
Ebola | Viral | 40-60% | Unvaccinated and untreated |
Plague, septicemic | Bacterial | 30-60% | Unvaccinated and untreated |
Anthrax, pulmonary | Bacterial | >85% | Unvaccinated and untreated |
Cryptococcal meningitis | Fungal | 30-40% | Co-infection with HIV |
Marburg virus disease | Viral | 23-90% | Untreated |
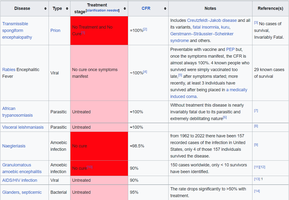
Extent of Host Involvement
Local Infection: Pathogens limited to a small area.
Systemic Infection: Spread throughout the body via blood and lymph.
Focal Infection: Systemic infection that began as a local infection.
Microbes or Toxins in the Blood
Sepsis: Toxic inflammatory condition from spread of microbes or toxins.
Bacteremia: Bacteria in the blood.
Septicemia: Growth of bacteria in the blood.
Toxemia: Toxins in the blood (e.g., preeclampsia).
Viremia: Viruses in the blood.
Primary vs Secondary Infection
Primary Infection: Acute infection causing initial illness.
Secondary Infection: Opportunistic infection following a primary infection (e.g., pneumonia after influenza).
Predisposing Factors
Factors that increase susceptibility to disease or alter its course.
Nutrition
Sex
Genetic inheritance
Climate
Environment
Vaccination
Age
Lifestyle/behaviors
Compromised host
Job
Development of Disease: Stages
Incubation Period: Interval between infection and first symptoms.
Prodromal Period: Early, mild symptoms.
Period of Illness: Disease is most severe.
Period of Decline: Symptoms subside.
Period of Convalescence: Recovery phase.
Spread of Infection: Reservoirs and Transmission
Reservoir: Continual source of infection (human, animal, nonliving).
Transmission: Movement of pathogen to susceptible host.
Invasion: Entry and multiplication in host.
Pathogenesis: Harm caused to host.
Reservoirs of Infection
Human Reservoirs: Symptomatic individuals, carriers (asymptomatic, incubating, convalescent, chronic, passive).
Animal Reservoirs: Zoonoses (e.g., rabies, malaria, Lyme disease).
Nonliving Reservoirs: Soil, water, food.
Transmission of Disease
Contact Transmission: Direct, indirect (fomites), droplet.
Vehicle Transmission: Airborne, waterborne, foodborne.
Vector Transmission: Arthropods (mechanical and biological transmission).
Healthcare-Associated Infections (HAIs)
HAIs are infections acquired during medical care.
Result from microorganisms in hospital environment, weakened hosts, and chain of transmission.
Compromised hosts are at higher risk.
Common sources: broken skin, suppressed immunity, invasive devices.
Control of HAIs
Universal Precautions: Reduce transmission in healthcare settings.
Standard Precautions: Basic practices for all patients (hand hygiene, PPE, disinfection).
Transmission-Based Precautions: Supplemental for highly transmissible infections (contact, droplet, airborne).
Reducing Pathogens: Handwashing, cleaning, disposable equipment.
Improving Resistance: Judicious antibiotic use, avoiding invasive procedures.
Emerging Infectious Diseases
Emerging diseases are new or increasing in incidence.
Contributing factors: genetic recombination, evolution, antibiotic resistance, climate change, transportation, ecological disruption, animal control, public health failure, bioterrorism.
R0 (“R naught”)
R0 is the basic reproduction number, indicating the average number of secondary cases produced by one infected individual.
R0 < 1: Disease will decline.
R0 = 1: Disease is stable.
R0 > 1: Disease is spreading.
Types of Epidemiology
Descriptive Epidemiology: Collection and analysis of data (e.g., John Snow and cholera).
Analytical Epidemiology: Determines probable cause or risk factors (e.g., Florence Nightingale).
Experimental Epidemiology: Hypothesis-driven, controlled experiments (e.g., Semmelweis).
Vaccine Efficacy
Vaccine efficacy is determined through clinical trials and epidemiological studies.
RSV vaccine: Pfizer and GSK trials.
COVID-19 vaccine: FDA approval based on large-scale trials.
Chicken pox vaccine: Tested in ~11,000 people prior to approval.
Summary Table: Modes of Transmission
Mode | Example | Description |
|---|---|---|
Direct Contact | COVID-19 | Person-to-person transmission |
Indirect Contact | Fomites | Transmission via objects |
Droplet | Influenza | Airborne droplets <1 meter |
Vehicle | Waterborne | Contaminated water |
Vector | Malaria | Biological transmission by mosquitoes |
Key Equations
Incidence Rate:
Prevalence Rate:
Case Fatality Ratio (CFR):
Infection Fatality Ratio (IFR):
Additional info: Academic context was added to clarify definitions, provide examples, and expand on brief points for completeness and self-contained study value.
