Back
BackPrinciples of Disease and Epidemiology: Study Notes
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Pathology and Disease Concepts
Pathology is the scientific study of disease, focusing on the cause (etiology), development (pathogenesis), and the structural and functional changes induced by disease. Understanding these concepts is fundamental to microbiology and epidemiology.
Etiology: The cause of a disease (e.g., Streptococcus pyogenes causes strep throat).
Pathogenesis: The process by which disease develops in the host.
Infection: Invasion or colonization of the body by pathogens; may not always result in disease.
Disease: An abnormal state in which the body is not functioning normally.
Normal Microbiota and the Human Microbiome
The human body is colonized by a vast array of microorganisms known as the normal microbiota. These microbes play essential roles in health and disease.
Normal microbiota: Permanently colonize the host without causing disease under normal conditions. Colonization begins at birth and changes with exposure to new environments.
Transient microbiota: Present for short periods (days to months).
Human Microbiome Project: Aims to analyze microbial communities on/in the human body and their relationship to health.

Factors Affecting Microbiota Distribution
Nutrients: Microbes require specific nutrients to colonize a region.
Physical and chemical factors: pH, temperature, and oxygen availability affect colonization.
Host defenses: Immune responses limit microbial growth.
Mechanical factors: Actions like chewing and flushing by urine remove microbes.
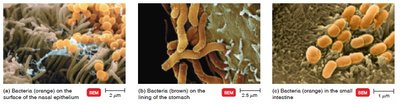
Germ-Free Animals in Research
Animals can be bred without microbiota for research purposes.
Such animals have underdeveloped immune systems, are more susceptible to disease, and require more calories and vitamins.
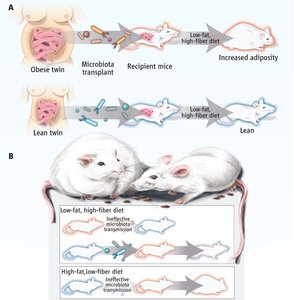
Relationships Between Microbiota and the Host
Normal microbiota interact with the host in various ways, including protection and competition with pathogens.
Microbial antagonism (competitive exclusion): Normal microbiota compete with pathogens for nutrients and produce substances harmful to invaders (e.g., E. coli produces bacteriocins).
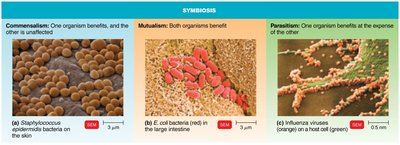
Symbiosis: The relationship between microbiota and host, which can be:
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit.
Parasitism: One organism benefits at the expense of the other.
Opportunistic pathogens: Normal microbiota that cause disease when introduced to new locations or when the host's defenses are compromised (e.g., C. difficile overgrowth after antibiotics).
Classifying Infectious Diseases
Communicable disease: Spread from one host to another (e.g., influenza, measles).
Contagious disease: Easily and rapidly spread (subset of communicable diseases).
Noncommunicable disease: Not spread from host to host (e.g., tetanus).
Occurrence of Disease
Incidence: Number of new cases during a specific time period.
Prevalence: Total number of cases (old and new) at a specific time.
Sporadic disease: Occurs occasionally.
Endemic disease: Constantly present in a population (e.g., common cold).
Epidemic disease: Many people acquire in a short time (e.g., influenza).
Pandemic disease: Worldwide epidemic (e.g., COVID-19).

Severity and Duration of Disease
Acute disease: Rapid onset, short duration (e.g., influenza).
Chronic disease: Develops slowly, lasts long (e.g., tuberculosis).
Subacute disease: Intermediate between acute and chronic.
Latent disease: Inactive for a time, then activates (e.g., herpes, shingles).
Extent of Host Involvement
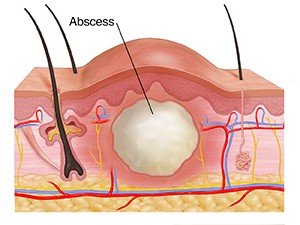
Local infection: Confined to a small area (e.g., abscess).
Systemic infection: Spread throughout the body (e.g., measles).
Focal infection: Systemic infection that began as a local infection.
Septicemia: Growth of bacteria in the blood (blood poisoning).
Sepsis: Toxic inflammatory response to infection in the blood.
Bacteremia: Bacteria in the blood.
Toxemia: Toxins in the blood.
Viremia: Viruses in the blood.
Primary infection: Acute infection causing initial illness.
Secondary infection: Opportunistic infection after a primary infection.
Subclinical disease: No noticeable symptoms (asymptomatic carriers).
Predisposing Factors
Factors that make the body more susceptible to disease include:
Gender
Inherited traits (e.g., sickle cell gene)
Climate and weather
Age (very young or old)
Fatigue, lifestyle, nutrition, chemotherapy, immune status
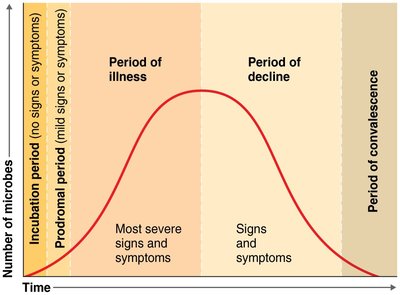
Development of Disease
The progression of disease typically follows these stages:
Incubation period: Time between infection and first symptoms.
Prodromal period: Mild, general symptoms.
Period of illness: Most severe signs and symptoms.
Period of decline: Symptoms subside.
Period of convalescence: Recovery and return to normal.
Reservoirs of Infection
Reservoirs: Continual sources of infection.
Human reservoirs: Carriers may have inapparent or latent infections.
Animal reservoirs: Zoonoses are diseases transmitted from animals to humans (e.g., rabies, Ebola).
Nonliving reservoirs: Soil and water.
Universal Precautions!!
• Standard: basic minimum practices applied every
time to prevent transmission of pathogens
• Handwashing, PPE (gloves, gowns, facemasks),
respiratory hygiene, cough etiquette
• Transmission-based: used with known or suspected
pathogens; supplement to standard precautions
• Contact precautions: for pathogens spread by
feces, urine, skin, vomit, wounds, or fomites
• Droplet precautions: for pathogens spread from
droplets from the respiratory system
• Airborne precautions: similar to droplet
precautions, but over larger distance
Transmission of Disease
Contact Transmission
Direct contact: Physical contact between infected and susceptible host (e.g., touching, kissing).
Indirect contact: Via nonliving object (fomite) such as toys, money, or syringes.
Droplet transmission: Via droplets that travel less than 1 meter (e.g., sneezing, coughing).

Vehicle Transmission
Waterborne: Contaminated water (e.g., cholera).
Foodborne: Improperly cooked or stored food, cross-contamination.
Airborne: Microorganisms travel more than 1 meter (e.g., tuberculosis).

Vector Transmission
Vectors: Arthropods (fleas, ticks, mosquitoes) transmit disease.
Mechanical transmission: Pathogen carried on vector's body (e.g., fly on food).
Biological transmission: Pathogen reproduces in vector and is transmitted via bites or feces.

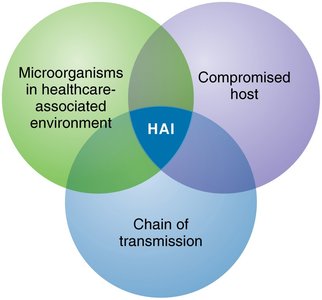
Healthcare-Associated Infections (HAIs)
HAIs are infections acquired while receiving treatment in a healthcare facility. They are a significant cause of morbidity and mortality.
Affect 1 in 25 hospital patients in the US.
Result from microorganisms in the hospital, compromised hosts, and chains of transmission.
Common pathogens: Clostridium difficile (currently #1), Staphylococcus aureus.
Prevention: Universal precautions, handwashing, PPE, and transmission-based precautions.
Emerging Infectious Diseases
Emerging infectious diseases are new, changing, or increasing in incidence. Most are viral, vector-borne, and zoonotic.
Causes: Genetic recombination, antibiotic resistance, changes in human behavior, ecological changes, public health failures, and bioterrorism.
Examples: E. coli O157:H7, avian influenza, MRSA, Zika virus.
Contributing factors:
• Modern transportation
• Chikungunya and West Nile virus
• Ecological disaster, war, and expanding human settlement
• Coccidioidomycosis – 10x increase in CA after
earthquake
• Animal control measures
• Lyme disease – deer predators killed which allow more
deer for the ticks to feed from
• Public health failure
• Diphtheria – adults not getting diphtheria boosters
caused outbreak in former Soviet states
• Bioterrorism
Epidemiology
Epidemiology is the study of where and when diseases occur and how they are transmitted in populations. Epidemiologists identify causes, risk factors, and methods for disease control.
Descriptive epidemiology: Collects data on disease occurrence (e.g., John Snow and cholera).
Analytical epidemiology: Compares affected and unaffected groups to find causes (e.g., Florence Nightingale).
Experimental epidemiology: Involves hypothesis testing and controlled experiments (e.g., Semmelweis and handwashing
John Snow 1848–1849 Mapped the occurrence of
cholera in London
Ignaz Semmelweis 1846–1848 Showed that handwashing
decreased the incidence of
peurperal sepsis
Florence
Nightingale
1858 Showed that improved
sanitation decreased the
incidence of epidemic
typhus
The Centers for Disease Control and Prevention (CDC)
Collects and analyzes epidemiological data in the US.
Publishes the Morbidity and Mortality Weekly Report (MMWR).
Morbidity: Incidence of a specific notifiable disease.
Mortality: Deaths from notifiable diseases.
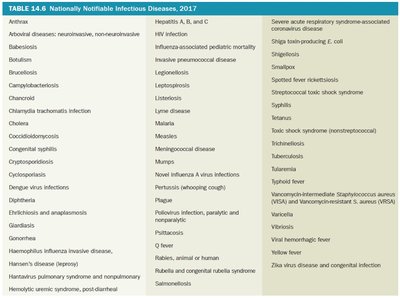
Notifiable infectious diseases: Diseases that must be reported by law to help control outbreaks.
Morbidity rate: Number of people affected relative to the population in a given time.
Mortality rate: Number of deaths relative to the population in a given time.
Morbidity: incidence of a specific notifiable
disease
• Mortality: deaths from notifiable diseases