 Back
BackPrinciples of Disease and Epidemiology – Study Notes
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Pathology, Infection, and Disease
Pathology is the scientific study of disease, including its causes, development, and effects on the body. Etiology refers to the cause of a disease, while pathogenesis describes the manner in which a disease develops. Diseases result in structural and functional changes in the body, which can be observed as signs and symptoms.
Infection: Invasion or colonization of the body by pathogenic microorganisms. Not all infections result in disease.
Disease: An abnormal state in which the body cannot perform normal functions.
Example: Escherichia coli is normally harmless in the intestines but can cause disease if it infects the urinary tract.
Human Microbiome Acquisition
The human microbiome is established as early as in the uterus and continues to develop through childbirth, feeding, and environmental exposure. The Human Microbiome Project studies these communities and their roles in health and disease.
Microbes colonize body sites with suitable nutrients, temperature, pH, and other factors.
Host defenses and mechanical forces (e.g., saliva flow, muscle movements) help regulate microbiome composition.
Microbial Interactions and Symbiosis
Normal microbiota can benefit the host by preventing the overgrowth of harmful organisms (microbial antagonism or competitive exclusion).
Symbiosis: Close association between two organisms.
Commensalism: One organism benefits, the other is unaffected (e.g., Staphylococcus epidermidis on skin).
Mutualism: Both organisms benefit (e.g., E. coli synthesizes vitamins K and B in the gut).
Parasitism: One organism benefits at the expense of the other (e.g., disease-causing bacteria, all viruses).
Normal, Transient, and Opportunistic Microbiota
Normal microbiota: Permanent residents, usually in a mutualistic relationship with the host.
Transient microbiota: Present for a short time.
Opportunistic microorganisms: Normally harmless but can cause disease in a different environment or in immunocompromised hosts.
Koch’s Postulates
Koch’s postulates are criteria used to establish a causative relationship between a microbe and a disease:
The same pathogen must be present in every case of the disease.
The pathogen must be isolated from the diseased host and grown in pure culture.
The pathogen from the pure culture must cause the disease when inoculated into a healthy, susceptible animal.
The pathogen must be re-isolated from the inoculated animal and shown to be the original organism.
Symptoms vs. Signs
Symptoms: Subjective changes (e.g., pain, discomfort) not apparent to outsiders.
Signs: Objective changes that can be observed and measured (e.g., fever, lesions, edema).
Types of Diseases
Communicable disease: Spread from one host to another (e.g., COVID-19, influenza).
Contagious disease: Easily and rapidly spread (e.g., measles).
Noncommunicable disease: Not spread from host to host (e.g., tetanus).
Incidence and Prevalence
Incidence: Number of new cases in a population during a specific time period.
Prevalence: Total number of cases (old and new) at a specific time.
Frequency and Severity of Disease
Sporadic: Occurs occasionally (e.g., typhoid fever).
Endemic: Constantly present (e.g., common cold).
Epidemic: Many people acquire in a short time (e.g., influenza).
Pandemic: Worldwide epidemic.
Acute: Rapid onset, short duration (e.g., influenza).
Chronic: Develops slowly, lasts long (e.g., tuberculosis).
Latent: Inactive for a time, then becomes active (e.g., shingles).
Severity and Fatality Ratios
Infection Fatality Ratio (IFR):
Case Fatality Ratio (CFR):
Herd Immunity
Herd immunity occurs when enough individuals in a population are immune to a disease, limiting its spread and protecting those who are not immune.
Extent of Host Involvement
Local infection: Limited to a small area (e.g., boils).
Systemic infection: Spread throughout the body (e.g., measles).
Focal infection: Local infection spreads to other parts (e.g., from teeth or tonsils).
Sepsis: Toxic inflammatory condition from spread of microbes.
Bacteremia: Bacteria in blood; toxemia: toxins in blood; viremia: viruses in blood.
Predisposing Factors
Factors that make the body more susceptible to disease include nutrition, sex, genetic inheritance, climate, age, environment, behavioral practices, vaccination status, and immune system status.
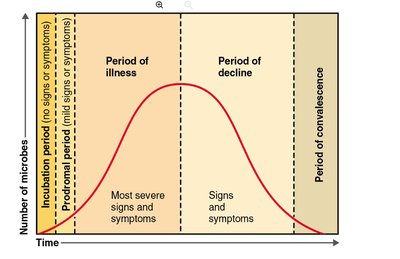
Stages in the Pattern of Disease
The progression of disease typically follows these stages:
Incubation period: Interval between initial infection and first appearance of signs or symptoms.
Prodromal period: Short period of early, mild symptoms.
Period of illness: Most severe signs and symptoms.
Period of decline: Signs and symptoms subside.
Period of convalescence: Recovery occurs.
Reservoirs of Infection
A reservoir of infection is a living or nonliving source that provides a pathogen with adequate conditions for survival and multiplication and an opportunity for transmission.
Human reservoirs: People with active infections or carriers (e.g., asymptomatic, incubating, convalescent, chronic, passive).
Animal reservoirs: Wild or domestic animals (e.g., rabies in bats, Lyme disease in mice).
Nonliving reservoirs: Soil and water (e.g., fungi, mycoses, ringworm).
Methods of Disease Transmission
Contact transmission: Direct (person-to-person), indirect (via fomites), or droplet (short-range airborne).
Vehicle transmission: By a medium such as air, water, or food.
Vector transmission: Animals (especially arthropods) transmit pathogens by mechanical or biological means.
Healthcare-Associated Infections (HAIs)
HAIs are infections acquired while receiving treatment in a healthcare facility. They are significant because they often involve resistant microorganisms and occur in compromised hosts.
Transmission can occur via direct contact (staff to patient, patient to patient) or indirect contact (fomites, ventilation systems).
Prevention includes handwashing, standard precautions (PPE, hygiene, disinfection), and transmission-based precautions (contact, droplet, airborne).
Emerging Infectious Diseases
Emerging diseases arise due to new strains, evolution of microbes, resistance, environmental changes, global travel, failures in public health, and bioterrorism.
Examples: New E. coli strains, avian influenza, Zika virus, antibiotic-resistant bacteria.
Epidemiology and the Role of the CDC
Epidemiology studies when and where diseases occur and how they are transmitted. The CDC is the central source of epidemiological information in the U.S.
Descriptive epidemiology: Collects data on disease occurrence.
Analytical epidemiology: Determines probable cause or risk factors (case-control and cohort methods).
Experimental epidemiology: Tests hypotheses (e.g., Semmelweis’s handwashing).
Case reporting: Tracks disease transmission chains.
Morbidity, Mortality, and Notifiable Diseases
Morbidity: Incidence of specific notifiable diseases.
Mortality: Number of deaths from these diseases.
Morbidity rate:
Mortality rate:
Notifiable infectious diseases: Diseases that must be reported by law to public health authorities (e.g., pertussis, salmonellosis, botulism).
