 Back
BackPrinciples of Disease and Epidemiology: Study Notes
Study Guide - Smart Notes

Principles of Disease and Epidemiology
Pathology, Infection, and Disease
Pathology is the scientific study of disease, focusing on the causes, development, and effects of diseases on the body. Understanding pathology is essential for diagnosing, treating, and preventing diseases.
Etiology: The cause of a disease.
Pathogenesis: The manner in which a disease develops.
Structural and Functional Changes: The effects of disease on body structure and function.
Disease: An abnormal state in which the body is not performing normal functions.
Infection: The invasion and growth of pathogens in the body, which may or may not result in disease.
The Human Microbiome
The human microbiome consists of all the microorganisms that reside on and within the human body. These microbial populations begin to establish themselves before birth and change rapidly during early life.
Placental microbiome: Contains few bacteria, mainly Enterobacteriaceae and Propionibacterium.
Vaginal delivery: Newborns are colonized by Lactobacillus.
Cesarean delivery: Microbiome resembles human skin, with Staphylococcus aureus being common.
Normal microbiota: Permanently colonize the host without causing disease under normal conditions.
Transient microbiota: Present temporarily.


Distribution and Composition of Normal Microbiota
The composition of normal microbiota varies by body region and is influenced by factors such as nutrients, physical and chemical conditions, host defenses, and mechanical factors.
Factors affecting microbiota: Age, diet, health status, hygiene, climate, geography, occupation, and lifestyle.

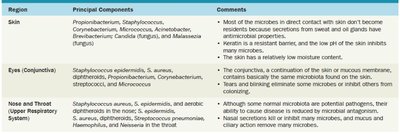
Relationships Between Normal Microbiota and the Host
Normal microbiota interact with the host in various ways, including competition and symbiosis.
Microbial antagonism (competitive exclusion): Normal microbiota compete with pathogens for nutrients and produce substances harmful to invaders.
Symbiosis: The relationship between microbiota and host, which can be:
Commensalism: One organism benefits, the other is unaffected.
Mutualism: Both organisms benefit.
Parasitism: One organism benefits at the expense of the other.
Some normal microbiota are opportunistic pathogens, causing disease under certain conditions.

Etiology of Infectious Disease
Koch’s Postulates
Koch’s postulates are a set of criteria used to establish that a specific microbe causes a specific disease. They are fundamental in identifying the etiology of infectious diseases.
The same pathogen must be present in every case of the disease.
The pathogen must be isolated from the diseased host and grown in pure culture.
The pathogen from the pure culture must cause the disease when inoculated into a healthy, susceptible animal.
The pathogen must be re-isolated from the inoculated animal and shown to be the original organism.
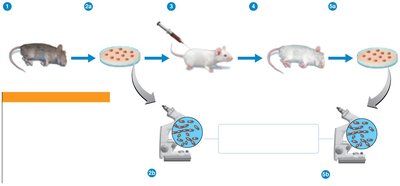
Exceptions: Some pathogens cannot be cultured, cause multiple diseases, or only infect humans.
Classifying Infectious Diseases
Diseases are classified based on their symptoms, signs, and syndromes, as well as their behavior in populations.
Symptoms: Subjective changes felt by the patient (e.g., pain, fatigue).
Signs: Objective changes observable by others (e.g., fever, rash).
Syndrome: A specific group of signs and symptoms that accompany a disease.
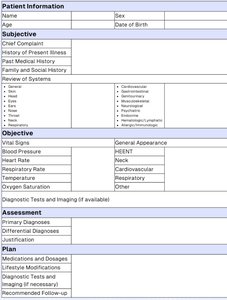

Communicable disease: Spread from one host to another.
Contagious disease: Easily and rapidly spread.
Noncommunicable disease: Not spread from host to host (e.g., tetanus).
Occurrence of Disease
The occurrence of disease is measured by incidence and prevalence, which help epidemiologists understand disease dynamics.
Incidence: Number of new cases in a specific time period.
Prevalence: Total number of cases (new and existing) at a given time.
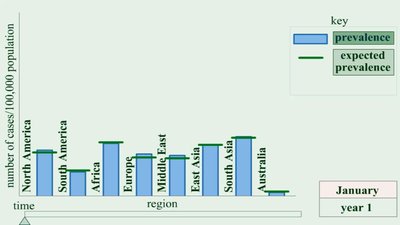
Sporadic disease: Occurs occasionally.
Endemic disease: Constantly present in a population.
Epidemic disease: Acquired by many people in a short time.
Pandemic disease: Worldwide epidemic.
Severity or Duration of Disease
Acute disease: Rapid onset, short duration (e.g., influenza).
Chronic disease: Develops slowly, lasts long (e.g., hepatitis C).
Subacute disease: Intermediate between acute and chronic.
Latent disease: Inactive for a time, then activates (e.g., shingles).
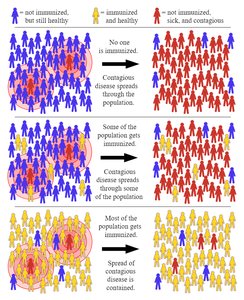
Herd immunity: Immunity in most of a population, reducing disease spread.
Extent of Host Involvement
Local infection: Pathogens limited to a small area.
Systemic infection: Infection throughout the body.
Focal infection: Systemic infection that began as local.
Sepsis: Toxic inflammatory condition from spread of microbes or toxins.
Bacteremia: Bacteria in the blood.
Septicemia: Growth of bacteria in the blood.
Toxemia: Toxins in the blood.
Viremia: Viruses in the blood.
Primary infection: Acute infection causing initial illness.
Secondary infection: Opportunistic infection after primary infection.
Subclinical disease: No noticeable signs or symptoms.
Development of Disease
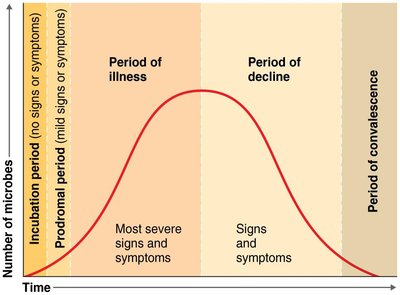
The development of disease follows a typical sequence of stages:
Incubation period: Interval between infection and first symptoms.
Prodromal period: Early, mild symptoms.
Period of illness: Disease is most severe.
Period of decline: Signs and symptoms subside.
Period of convalescence: Body returns to prediseased state.
Reservoirs and Transmission of Infection
Reservoirs of Infection
Reservoirs are continual sources of infection, which may be living or nonliving.
Human reservoirs: People with active disease or carriers (asymptomatic, incubating, convalescent, chronic, passive).
Animal reservoirs: Wild and domestic animals (zoonoses).
Nonliving reservoirs: Soil (e.g., Clostridium species), water (e.g., Vibrio cholerae), and contaminated objects.
Transmission of Disease
Pathogens are transmitted from reservoirs to susceptible hosts by various routes:
Contact transmission:
Direct contact: Physical contact between infected and susceptible host.
Indirect contact: Via fomites (nonliving objects).
Droplet transmission: Airborne droplets less than 1 meter.
Congenital transmission: Mother to fetus or newborn at birth.

Vehicle transmission: Transmission by inanimate reservoirs (air, water, food).

Vector transmission: Arthropods (e.g., fleas, ticks, mosquitoes) transmit pathogens by:
Mechanical transmission: Pathogen carried on vector's body.
Biological transmission: Pathogen reproduces in vector, transmitted via bites or feces.

Healthcare-Associated Infections (HAIs)
Overview of HAIs
Healthcare-associated infections (HAIs), also known as nosocomial infections, are acquired while receiving treatment in a healthcare facility. They affect a significant proportion of patients and can be life-threatening.
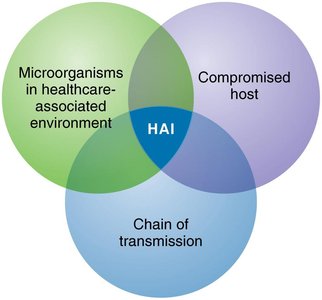
Result from microorganisms in the hospital, weakened host defenses, and the chain of transmission.
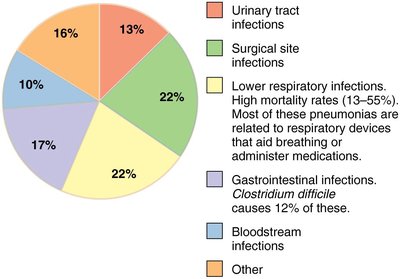
Common sites: Urinary tract, surgical sites, respiratory tract, gastrointestinal tract, bloodstream.

Microorganisms Involved in HAIs
Microorganism | Most Common Infection Type | Percentage of Total Infections | Percentage Resistant to Antibiotics |
|---|---|---|---|
Coagulase-negative staphylococci | Bloodstream | 11% | Not reported |
Staphylococcus aureus | Surgical wound | 16% | 55% |
Clostridium difficile | Diarrhea after abdominal surgery | 15% | 83% |
Enterococcus spp. | Bloodstream | 14% | 83% |
Candida spp. (fungus) | Urinary tract infections | 12% | Not reported |
Pseudomonas aeruginosa | Urinary tract and pneumonia | 11% | 28% |
Klebsiella pneumoniae | All sites | 8% | 29% |
Escherichia coli | Urinary tract infections | 12% | 20% |
Acinetobacter baumannii | All sites | 2% | 68% |
Control of Healthcare-Associated Infections
Prevention and control of HAIs involve strict adherence to infection control practices.
Universal and standard precautions: Basic practices for all patients.
Transmission-based precautions: Additional measures for known or suspected infections (contact, droplet, airborne).
Handwashing, disinfection, proper instrument cleaning, and use of disposables are critical.
Infection control committees oversee protocols and compliance.
Epidemiology
Principles of Epidemiology
Epidemiology is the study of where and when diseases occur and how they are transmitted in populations. Epidemiologists play a key role in disease control and prevention.
Determine etiology and factors influencing disease spread.
Develop methods for disease control.
Collect and analyze data to track disease incidence and prevalence.
The Centers for Disease Control and Prevention (CDC)
Collects and analyzes epidemiological data in the U.S.
Publishes the Morbidity and Mortality Weekly Report (MMWR).
Morbidity: Incidence of a specific notifiable disease.
Mortality: Deaths from notifiable diseases.
Morbidity rate: Number of people affected in relation to the total population in a given time period.
Mortality rate: Number of deaths from a disease in relation to the population in a given time.
