 Back
BackPrinciples of Infectious Disease, Epidemiology, and Immunity: Study Notes for Microbiology
Study Guide - Smart Notes

Principles of Infectious Disease and Epidemiology
Basic Disease Terminology
Understanding infectious diseases and their spread is foundational in microbiology. Epidemiology is the study of disease occurrence and control in populations.
Infectious disease: Illness caused by a pathogen (e.g., bacteria, viruses, fungi, protozoa, helminths, prions).
Epidemiology: The science of monitoring and controlling disease to promote public health.
Pathogen: Any microorganism capable of causing disease.
Opportunistic pathogen: Causes disease only in weakened hosts.
True pathogen: Can cause disease in healthy hosts
Communicable vs. Noncommunicable Diseases
Communicable: Transmitted from human to human.
Contagious: Easily transmitted between hosts.
Latent infection: Pathogen is present but patient is asymptomatic.
Acute disease: Rapid onset and progression.
Chronic disease: Slow onset and progression.
Koch’s Postulates
Koch’s postulates are criteria for linking a specific microbe to a specific disease:
The same organism must be present in every case of the disease.
The organism must be isolated and grown in pure culture.
The cultured organism must cause disease when introduced into a healthy host.
The organism must be re-isolated from the experimentally infected host.
Limitations: Not all pathogens can be cultured, some only infect humans, and latent infections complicate application.
Reservoirs and Sources of Infection
Reservoir: Natural habitat of a pathogen (animate or inanimate).
Source: Immediate origin from which a host acquires the pathogen.
Endogenous source: Pathogen originates from the host’s own body.
Exogenous source: Pathogen comes from outside the host.
Stages of Infectious Disease
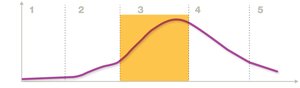
Infections progress through five general stages:
1. Incubation period: Time between infection and appearance of symptoms.
2. Prodromal phase: Early, mild symptoms develop.
3. Acute phase: Peak of disease; most severe symptoms.
4. Period of decline: Symptoms begin to resolve as pathogen is controlled.
5. Convalescent phase: Recovery; pathogen may remain latent.
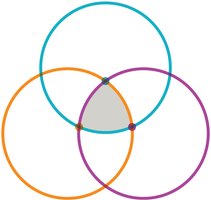
Epidemiological Triangle
The epidemiological triangle illustrates the interaction between the host, the etiological agent, and the environment in disease development.
Host factors: General health, age, sex, lifestyle, genetics.
Etiological agent: Type of microbe (bacteria, virus, fungus, parasite, prion).
Environmental factors: Climate, geography, vectors, water/food sources.
Breaking the Epidemiological Triangle
Public health strategies: Education, quarantine, vector control.
Personal habits: Hand washing, clean water, avoiding risky behaviors.
Host–Microbe Interactions and Pathogenesis
Normal Microbiota and Pathogenicity
Normal microbiota colonize various body sites and usually do not cause disease. Pathogens have adaptations for host interaction and can disrupt this balance (dysbiosis).
Opportunistic pathogens: Cause disease when host defenses are compromised.
Tropism: Pathogen preference for specific host tissues.
Virulence and Virulence Factors
Pathogenicity: Ability to cause disease.
Virulence: Degree of pathogenicity (severity of disease).
Virulence factors: Mechanisms that help pathogens adhere, invade, evade immunity, and damage host cells.

Attenuation
Attenuated pathogens: Weakened but still infectious; often used in vaccines.
Toxins as Virulence Factors
Toxins: Molecules that damage host tissues or suppress immune responses.
Toxigenic: Microbes that produce toxins.
Toxemia: Toxins in the bloodstream.
Cytopathic Effects
Cytocidal: Kill host cells.
Noncytocidal: Damage but do not kill host cells.
Mechanisms: Invasion, toxin release, nutrient exploitation, disruption of cell function, transformation to cancer cells.
Immune Evasion Strategies
Intracellular lifestyle: Hiding inside host cells (e.g., viruses, Mycobacterium tuberculosis).
Latency: Remaining dormant in host tissues (e.g., herpesviruses, HIV).
Antigenic masking/mimicry/variation: Concealing or altering surface molecules to avoid immune detection.
Interference with phagocytosis: Capsules, escaping phagosomes, neutralizing enzymes.
Immune suppression: Targeting immune cells, degrading antibodies, interfering with signaling.
Lymphoid Tissues and Leukocytes
Primary lymphoid tissues: Bone marrow and thymus (leukocyte production and maturation).
Secondary lymphoid tissues: Lymph nodes, spleen, MALT (filter lymph, sample antigens).
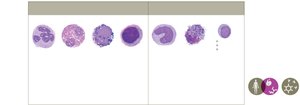
Leukocytes: White blood cells essential for immune responses (granulocytes and agranulocytes).
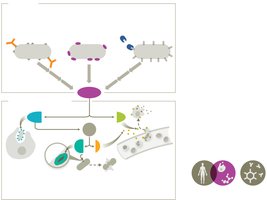
Cytokines and Complement System
Cytokines: Signaling proteins coordinating immune actions; can be diagnostic markers.
Complement system: Cascade of proteins that opsonize pathogens, promote inflammation, and lyse cells.
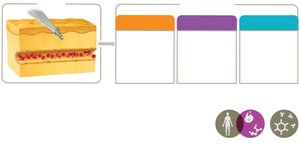
Inflammation
Inflammation is a key innate response to tissue injury or infection, occurring in three phases:
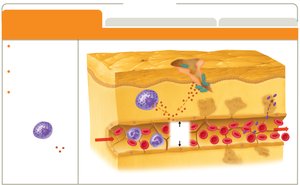
Vascular changes: Increased blood flow and vessel permeability.
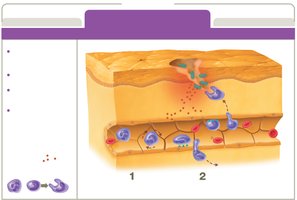
Leukocyte recruitment: Neutrophils and monocytes migrate to the site, phagocytize invaders.
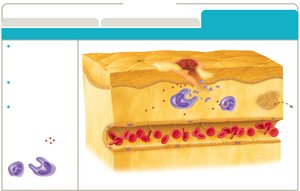
Resolution: Inflammation subsides, tissue repair begins.
Immune System Disorders
Autoimmunity and Hypersensitivities
Autoimmunity: Immune attack against self-tissues (e.g., lupus, rheumatoid arthritis, type I diabetes).
Hypersensitivities: Inappropriate immune responses classified as:
Type | Mechanism | Examples |
|---|---|---|
I (Allergy) | IgE-mediated, immediate | Allergic rhinitis, anaphylaxis |
II (Cytotoxic) | IgG/IgM to cell-bound antigens | Hemolytic anemia, transfusion reactions |
III (Immune Complex) | IgG/IgM to soluble antigens | Lupus, serum sickness |
IV (Delayed) | T cell-mediated | Contact dermatitis, tuberculin test |
Transplantation and Graft Rejection
Autograft: From self; no rejection.
Isograft: From identical twin; minimal rejection.
Allograft: From same species; possible rejection.
Xenograft: From different species; high rejection risk.
Graft-versus-host disease: Donor immune cells attack recipient tissues (e.g., after bone marrow transplant).
