 Back
BackPrinciples of Infectious Disease, Immunity, and Antimicrobial Drugs: Study Notes
Study Guide - Smart Notes

Principles of Infectious Disease
Transmission of Infectious Diseases
Understanding how infectious diseases spread is crucial for prevention and control. Transmission can occur through various routes:
Contact Transmission: Direct (physical contact, including congenital transmission from mother to child) or indirect (via fomites).
Droplet Transmission: Spread via respiratory droplets over short distances.
Vehicle Transmission: Through air (airborne, >1 meter), water (waterborne), or food (foodborne).
Vector Transmission: Via animals such as fleas and ticks, either mechanically (carrying pathogens externally) or biologically (pathogen reproduces inside vector).
Epidemiology
Epidemiology is the study and analysis of disease patterns in populations. It includes:
Analytical Studies: Comparing diseased and healthy groups.
Experimental Studies: Controlled experiments, including blind and double-blind studies.
Case Reporting: Healthcare workers report notifiable diseases (e.g., AIDS, measles, rabies) to authorities.
Microbial Pathogenicity
Pathogenicity and Virulence
Pathogenicity is the ability of a microbe to cause disease, requiring entry, growth, damage, and evasion of host defenses. Virulence refers to the degree of damage caused.
Factors include microbial structures, toxins, replication rate, and immune evasion.
Chain of Infection
Portals of Entry: Mouth, skin, eyes, mucosal membranes, parenteral route.
Susceptible Host: Individuals with weakened or immature immune systems.
Infectious Dose vs. Lethal Dose
ID50: Infectious dose for 50% of the population.
LD50: Lethal dose for 50% of the population.
Virulence Factors
Adhesins: Surface molecules (glycocalyx, fimbriae, pili) that help microbes attach to host cells.
Capsules: Inhibit phagocytosis.
Cell Wall Components: E.g., mycolic acid in Mycobacterium tuberculosis resists immune attack.
Antigenic Variation: Changing surface proteins to evade immune detection.
Exoenzymes: Coagulases, kinases, hyaluronidase, collagenase—aid in spreading and evading host defenses.
Invasins: Facilitate entry into host cells via receptor-mediated endocytosis.
Siderophores: Steal iron from host proteins.
Toxins: Exotoxins (secreted proteins, often enzymes) and endotoxins (part of Gram-negative cell wall).
Phagocytosis and Innate Immunity
Phagocytosis
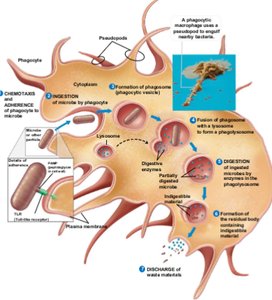
Phagocytosis is the process by which cells (e.g., neutrophils, monocytes) ingest and destroy microbes.
Steps: Chemotaxis, adherence, ingestion, formation of phagosome, fusion with lysosome, digestion, discharge of waste.
Inflammation and Fever
Inflammation: Redness, pain, heat, swelling; acute (short-term) or chronic (long-term).
Fever: Systemic increase in body temperature, mediated by cytokines (e.g., interleukins, TNF).
Interferons and Antimicrobial Peptides
Interferons: Cytokines produced by virus-infected cells to inhibit viral replication in neighboring cells.
Antimicrobial Peptides: Short peptides that disrupt microbial membranes or neutralize endotoxins.
Complement System
Serum proteins that act in a cascade to cause cytolysis, opsonization, and inflammation.
Adaptive Immune System
Humoral and Cellular Immunity
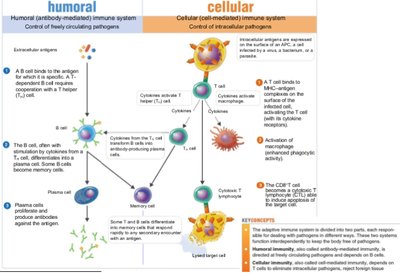
The adaptive immune system provides specific defense against pathogens and has memory for future responses.
Humoral Immunity: Mediated by B cells producing antibodies against extracellular antigens.
Cellular Immunity: Mediated by T cells targeting intracellular pathogens.
Antigens and Antibodies
Antigen: Any substance that induces an immune response.
Antibody (Immunoglobulin, Ig): Globular proteins produced by B cells, specific for antigens.
B Cells and Antigen Presentation
B cells display antigen fragments on MHC proteins for recognition by other immune cells.
Activation occurs via antigen binding and cytokine signaling.
Antigen Presenting Cells (APCs)
Examples: Macrophages, dendritic cells.
Present antigens to T helper cells to initiate immune response.
Classes of T Cells
T Helper Cells: Activate B cells and other immune cells.
Cytotoxic T Cells: Kill infected cells.
Regulatory T Cells: Regulate immune response.
Immunological Memory
Adaptive immunity provides long-term protection via memory cells.
Types of Adaptive Immunity
Naturally Acquired Active Immunity: From infection and recovery.
Naturally Acquired Passive Immunity: Maternal antibodies transferred to infant.
Artificially Acquired Active Immunity: Vaccination.
Artificially Acquired Passive Immunity: Injection of antibodies.
Vaccines
Types of Vaccines
Live Attenuated: Weakened pathogens, robust immunity.
Inactivated/Killed: Killed pathogens, weaker response, may need boosters.
Subunit: Toxoids, antigenic fragments, recombinant proteins.
Conjugated: Linked antigens for better response.
Recombinant Vector: Use avirulent organisms to deliver antigen genes.
Nucleic Acid (mRNA): Lipid nanoparticles deliver mRNA encoding antigen.
Immunological-Based Tests
Monoclonal Antibodies and ELISA
Monoclonal Antibodies: Highly specific, used for diagnostics.
ELISA: Detects presence of antigen or antibody using enzyme-linked antibodies.
Antimicrobial Drugs
Antibiotics and Selective Toxicity
Antibiotics: Substances produced by microbes to inhibit other microbes (e.g., penicillin).
Selective Toxicity: Targeting microbes without harming host.
Bactericidal: Kill microbes directly.
Bacteriostatic: Inhibit growth, allowing immune system to clear infection.
Targets of Antimicrobial Drugs
Cell wall synthesis (e.g., peptidoglycan in bacteria).
Protein synthesis (bacterial 70S ribosomes vs. eukaryotic 80S).
Nucleic acid replication and transcription.
Plasma membrane integrity.
Essential metabolite synthesis.
Drug Synergy and Antagonism
Synergy: Two drugs enhance each other's effects.
Antagonism: One drug interferes with the action of another (e.g., penicillin and tetracycline).
Antifungal and Antiviral Drugs
Antifungals target ergosterol in fungal membranes.
Antivirals often target viral genome replication.
Antibiotic Resistance
Misuse of antibiotics selects for resistant mutants.
Mechanisms: Blocking entry, inactivation by enzymes, target alteration, efflux pumps.
Table: Mechanisms of Antibiotic Resistance
Mechanism | Description |
|---|---|
Blocking Entry | Prevents antibiotic from entering the cell |
Enzymatic Inactivation | Bacterial enzymes degrade or modify the antibiotic |
Target Alteration | Mutation changes the antibiotic's binding site |
Efflux Pumps | Pumps antibiotic out of the cell |
Additional info: E. coli can adapt to high antibiotic concentrations rapidly, demonstrating the importance of prudent antibiotic use.
