 Back
BackRespiratory System Infections: Microbiology Study Guide (Ch. 16)
Study Guide - Smart Notes

Respiratory System Infections
Overview of the Respiratory System
The human respiratory system is responsible for gas exchange, bringing oxygen into the body and removing carbon dioxide. It is divided into the upper and lower respiratory tracts, each with distinct anatomical features and functions. The respiratory tract is a common portal of entry for pathogens, making it a frequent site of infection.
Upper respiratory tract: Includes the mouth, nasal passages, paranasal sinuses, pharynx, and epiglottis. Functions to warm, humidify, and filter air.
Lower respiratory tract: Comprises the larynx, trachea, bronchi, bronchioles, lungs, and alveoli. Directs air to the lungs, where gas exchange occurs.
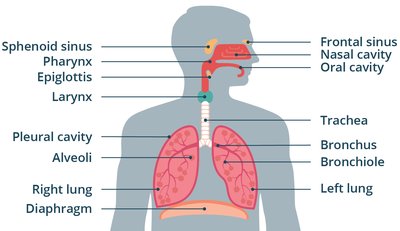
Upper Respiratory Tract Anatomy and Defenses
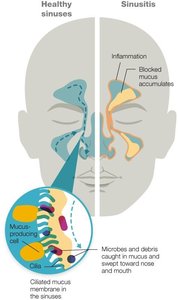
The upper respiratory tract contains several pairs of paranasal sinuses, which are hollow cavities lined with mucous membranes. These membranes secrete mucus to trap microbes and debris, which are then swept toward the nose and mouth by cilia.
Sinusitis: Inflammation of the sinuses, often caused by viruses or allergens, leading to mucus accumulation and potential secondary bacterial infection.
Lower Respiratory Tract Anatomy and Defenses
The lower respiratory tract is protected by the mucociliary escalator, a system of ciliated mucous membranes that trap and move debris out of the lungs. Alveolar macrophages reside in the alveoli and clear out pathogens not trapped by the mucociliary escalator.
Mucociliary escalator: Prevents inhaled debris from reaching the lungs.
Alveolar macrophages: Engulf and destroy pathogens in the alveoli.
Common Respiratory Tract Infections and Symptoms
Respiratory tract infections can affect both the upper and lower tracts, leading to a range of symptoms:
Upper tract: Sinusitis, pharyngitis (sore throat)
Lower tract: Laryngitis, tracheitis, bronchitis, croup (laryngotracheobronchitis- respiratory stridor), pneumonia (most severe, inflammation of lung tissue)
Common symptoms: Coughing, stridor (abnormal noisy breathing), dyspnea (shortness of breath), fatigue, sneezing, sore throat, fever
Transmission and Prevention of Respiratory Infections
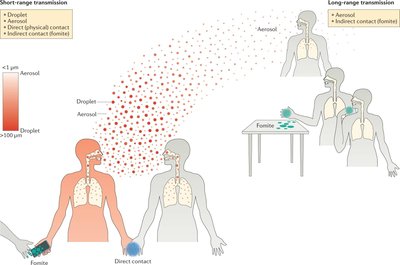
Respiratory infections are commonly transmitted long vs. short-range via respiratory droplets, aerosols, direct contact, and indirect contact (fomites).
Preventive measures include good hygiene practices such as covering the mouth and nose when coughing or sneezing, proper disposal of tissues, and frequent handwashing.
Respiratory Tract Microbiome
Normal Microbiota and Its Impact
The respiratory tract is colonized by a diverse community of microorganisms, known as the normal microbiota. These microbes are generally beneficial, competing with potential pathogens and sometimes producing antimicrobial substances. A healthy respiratory microbiome is associated with high species diversity, while dysbiosis (microbial imbalance) is linked to respiratory diseases such as asthma and COPD.
Viral Infections of the Respiratory Tract
Viral infections of the respiratory tract
ARI
RSV
Influenza (IAV IBV)
SARS-CoV2
1. Acute Respiratory Infection (ARI) / Upper Respiratory Infections (URI)– The Common Cold
The common cold is an acute respiratory infection (ARI) caused by over 200 genetically distinct viruses, primarily rhinoviruses and coronaviruses. It is highly communicable and usually self-limiting, but can lead to secondary bacterial infections.
Eitiologic agent:
Serovars of rhinoviruses and coronaviruses cause 60-80% of colds
Other viruses that cause colds include
Parainfluenza, adenoviruses, nonpolio-type enteroviruses
Transmission: Personal contact, respiratory droplets, fomites
Symptoms: Runny nose, sore throat, cough/sneezing, fatigue, low-grade fever- children, thickened mucus
At-risk groups: Children (average 6 colds/year), adults (average 3 colds/year)
Treatment: Antibiotics are ineffective; supportive care is recommended
Secondary bacterial infections may require antibiotics
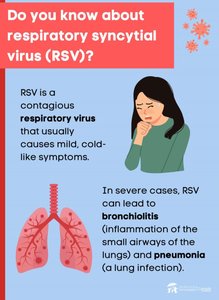
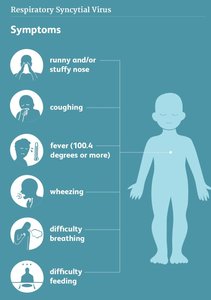
Respiratory Syncytial Virus (RSV)
RSV is a major cause of severe respiratory illness, especially in infants, the elderly, and immunocompromised individuals. It is an enveloped, single-stranded RNA virus transmitted via respiratory aerosols and direct contact.
Etiologic agent: enveloped single-stranded (SS) RNA virus
Epidemiology: all age groups, common in winter, severe in infants, elderly, immune or lung-compromised, and community outbreaks and HAI.
Transmission: respiratory aerosols, direct contact with eyes/nose
Symptoms: Coughing, sneezing, fever, wheezing
Prevention: Handwashing, avoiding sick individuals, vaccination for high-risk groups
Treatment: Supportive care; antiviral drugs in severe cases

Influenza Viruses- Cause of Flu Infections
Influenza viruses (Types A, B, and C) are enveloped, segmented RNA viruses that cause seasonal flu epidemics and occasional pandemics. Type A is the most severe and can infect multiple species, while Type B primarily affects humans, especially children.
Etiologic Agent
Enveloped SS 8-segmented RNA virus
Most common severe respiratory virus – “the flu.”
Signs and symptoms: Resembles a severe cold, may not present with sneezing
Mechanism of disease
Most strains bind ciliated cells in the upper respiratory tract
Some strains can directly affect the lungs
Complications
Secondary bacterial infections
Pneumonia
Can be deadly in those with pre-existing conditions
3 related types of influenza viruses infect humans – tropism differences:
A. Type A (IAV) • Moderate to severe illness • All age groups • Avian and mammalian • Pandemics
B. Type B (IBV) • Mild to moderate disease • All ages, but primarily children • Epidemics
C. Type C • Rare in humans; no epidemics (yet)
Virulence factors: Hemagglutinin (HA) and neuraminidase (NA) glycoproteins
1. Hemagglutinin (HA) and neuraminidase (NA) are glycoprotein spikes on the surface of the influenza virus
2. HA allows influenza to attach and invade target cells in the respiratory tract
3. NA helps newly formed viral particles escape the host cell
Antigenic drift: Minor changes in HA and NA spikes due to mutations, leading to seasonal epidemics
Antigenic shift: Major genetic change, potentially causing pandemics
Prevention: Annual vaccination, hygiene practices

SARS-CoV2- Severe Acute Respiratory Syndrome- Coronacirus 2
1. Enveloped virus
2. Single-stranded RNA genome
3. Spike proteins (S proteins)
4. Disease: COVID-19
5. Global pandemic: 2020 – 2025 • 7.1 million reported deaths • Actual estimated deaths: 18.5 – 33.5 M
6. 2025 – present: endemic
SARS-CoV-2 → Mechanism of disease
1. Spreads via respiratory droplets and aerosols
2. Binds to ACE2 on host cells
3. Symptoms can develop within 2 to 14 days
4. Degree of disease severity varies greatly by patient factors and underlying conditions
5. COVID-19 kills patients due to a sudden and marked reduction in blood oxygenation: Acute respiratory distress syndrome (ARDS)
SARS-CoV-2 Variants and Strains
1. RNA viruses tend to mutate more frequently than DNA viruses leading to viral variants
2. If viral functions are altered, the variant is a new viral strain
3. Emerging SARS-CoV-2 variants are categorized by the risk: •Variants of interest •Variants of concern •Variants of high consequence
Bacterial Infections of the Respiratory Tract Refer to slides 47-89
Streptococcus pyogenes (Group A Strep)
Streptococcus pyogenes is a Gram-positive, catalase-negative coccus that causes pharyngitis (strep throat), scarlet fever, and other diseases. It is transmitted via respiratory droplets and can lead to serious complications if untreated.
Virulence factors: Hyaluronic acid capsule, M protein, exotoxins
Complications: Rheumatic fever, glomerulonephritis, PANDAS
Diagnosis: Rapid strep test, culture
Treatment: Penicillin-based antibiotics
Bordetella pertussis (Whooping Cough)
Bordetella pertussis is a Gram-negative, aerobic coccobacillus that causes pertussis (whooping cough). It is highly contagious and characterized by severe coughing fits. Vaccination (DTaP/Tdap) is the most effective prevention.
Stages: Catarrhal (cold-like), paroxysmal (severe cough), convalescent (recovery)
Treatment: Early antibiotics, supportive care
Mycobacterium tuberculosis (Tuberculosis)
Mycobacterium tuberculosis is an acid-fast bacillus with a waxy mycolic acid cell wall, making it resistant to many antibiotics and immune defenses. TB can be latent or active, with the latter being infectious and potentially fatal if untreated.
Transmission: Inhalation of contaminated droplets
Diagnosis: Tuberculin skin test, chest X-ray, sputum analysis
Treatment: Multi-drug therapy for several months
Prevention: BCG vaccine (for children in high-prevalence areas), infection control
Pneumonia
Pneumonia is an infection of the lower respiratory tract, leading to inflammation and fluid accumulation in the alveoli. It can be caused by bacteria, viruses, or fungi, with Streptococcus pneumoniae being the most common bacterial cause of typical pneumonia.
Typical pneumonia: Sudden onset, high fever, productive cough, lobar consolidation
Atypical pneumonia: Gradual onset, milder symptoms, non-productive cough
Prevention: Vaccination (pneumococcal vaccines), healthy living practices
Clinical Feature | Typical Pneumonia | Atypical Pneumonia |
|---|---|---|
Onset | Sudden, severe | Gradual, milder |
Fever | High | Lower |
Cough | Productive (sputum) | Non-productive |
Chest X-ray | Lobar consolidation | Patchy or diffuse infiltrates |
Common agents | S. pneumoniae | Mycoplasma pneumoniae, Legionella pneumophila |
Fungal Infections of the Respiratory Tract
Overview and Epidemiology
Fungal respiratory infections are rare in healthy individuals but are becoming more common due to increased numbers of immunocompromised patients and environmental changes. Fungi can be opportunistic or endemic pathogens.
Opportunistic fungi: Infect immunocompromised hosts (e.g., Aspergillus, Pneumocystis)
Endemic fungi: Cause disease in healthy hosts in specific geographic regions (e.g., Blastomyces dermatitidis)
Blastomycosis
Blastomyces dermatitidis is a dimorphic fungus endemic to certain regions of North America. Infection occurs via inhalation of spores from disturbed soil. The disease can present with pneumonia-like symptoms and may disseminate if untreated.
Transmission: Inhalation of airborne spores
Symptoms: Fever, cough, night sweats, muscle aches, weight loss
Treatment: Long-term antifungal therapy
Prevention: Avoiding exposure to contaminated soil
Summary
Respiratory system infections encompass a wide range of viral, bacterial, and fungal diseases, each with unique epidemiology, pathogenesis, and prevention strategies. Understanding the anatomy, normal microbiota, and immune defenses of the respiratory tract is essential for recognizing, diagnosing, and managing these infections effectively.
