 Back
BackSkin and Eye Infections: Microbiology Study Notes
Study Guide - Smart Notes

Skin and Eye Infections
Overview
This chapter explores the major microbial diseases affecting the skin and eyes, including their causative agents, pathogenesis, clinical features, and prevention/treatment strategies. Both viral, bacterial, and fungal pathogens are discussed, as well as the anatomical and immunological defenses of these organs.
Anatomical Features and Defenses of the Skin
Structure of the Skin
The skin is the largest organ of the body and serves as a primary barrier against infection. It consists of multiple layers, each with specialized cells and functions.
Epidermis: Outermost layer, composed of tightly packed dead cells (stratum corneum) and living keratinocytes filled with keratin.
Dermis: Inner layer made of connective tissue, containing macrophages, mast cells, nerves, blood vessels, and lymphatics.
Subcutaneous Layer: Contains fat and connective tissue, providing insulation and cushioning.
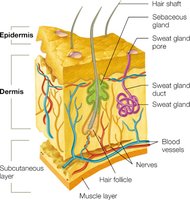
Defenses of the Skin
Keratinized surface: Provides a tough, water-resistant barrier.
Melanin: Has antimicrobial properties.
Perspiration: Acidic pH and high salt content inhibit microbial growth.
Lysozyme: Enzyme in sweat that breaks down bacterial peptidoglycan.
Sebum: Oily secretion with low pH and antimicrobial lipids.
Skin Microbiome
The skin hosts a diverse microbiome that provides protection against pathogens. Factors influencing the skin microbiome include:
Environmental exposure
Occupation
Antibiotic usage
Age
Cosmetics, moisturizers, soaps
Clothing
Hormone levels
Viral Skin Infections
Chickenpox and Shingles (Varicella-Zoster Virus, HHV-3)
Chickenpox is a highly contagious disease caused by the varicella-zoster virus, transmitted via respiratory droplets and direct contact with lesions. After initial infection, the virus can become latent in peripheral nerves and reactivate later in life as shingles.
Chickenpox: Fever, itchy vesicular rash; prevented by live attenuated vaccine.
Shingles: Reactivation in adults, often with chronic pain (postherpetic neuralgia); prevented by Shingrix vaccine.
Herpes Simplex Virus 1 (HSV-1)
HSV-1 causes oral herpes (cold sores) and can establish latency in the trigeminal nerve. Reactivation is triggered by stress, UV light, or hormonal changes. Transmission occurs via saliva, respiratory droplets, or contaminated fomites.
No cure or vaccine; antiviral medications reduce symptoms.
Whitlow is a rare HSV-1 infection of the fingers, more common in healthcare workers.
Measles (Rubeola)
Measles is a highly contagious viral disease characterized by a maculopapular rash and Koplik’s spots. It can cause severe complications, including secondary infections and subacute sclerosing panencephalitis (SSPE).
Transmission: Respiratory droplets.
Prevention: MMR vaccine (live attenuated).
Complications: Hospitalization, brain swelling, death.
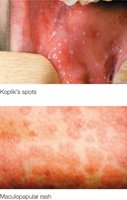
Rubella (German Measles)
Rubella virus causes a mild rash disease but can lead to severe congenital defects if contracted during pregnancy (Congenital Rubella Syndrome, CRS).
Transmission: Respiratory droplets.
Prevention: MMR vaccine (not for pregnant women, infants <1 year, or immunosuppressed).
CRS: Stillbirth, miscarriage, birth defects (blindness, deafness, heart defects).
Warts (Human Papillomaviruses, HPV)
HPV causes benign epithelial growths (warts) that are usually harmless and self-limiting.
Transmission: Direct/indirect contact, fomites.
Treatment: Cauterization, chemicals, cryosurgery, laser.
Bacterial Skin Infections
Staphylococcus aureus Infections
Staphylococcus aureus is a highly virulent, gram-positive coccus that causes a range of skin infections.
Virulence factors: Coagulase, hyaluronidase, staphylokinase, DNAse, superantigens.
Impetigo: Superficial, pus-filled, itchy vesicles; highly contagious; treated with topical antibiotics.
Staphylococcal Scalded Skin Syndrome (SSSS): Exfoliative toxins cause blistering and sloughing of skin, mainly in newborns.
MRSA: Methicillin-resistant S. aureus, resistant to multiple antibiotics.
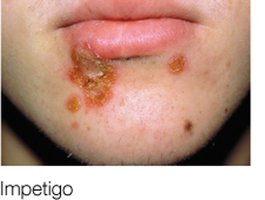
Streptococcus pyogenes Infections
Streptococcus pyogenes is a gram-positive coccus responsible for various skin and systemic infections.
Virulence factors: M-protein, beta hemolysin, hyaluronidase, streptokinase, capsule.
Erysipelas: Painful, inflamed skin with blisters and fever, often on the face.
Necrotizing fasciitis: Rapidly spreading infection that destroys connective tissue; high mortality rate (~40%).
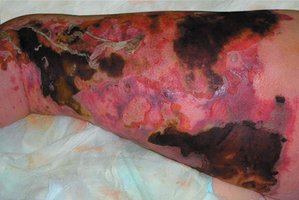
Gas Gangrene (Clostridium perfringens)
Gas gangrene is a severe infection caused by Clostridium perfringens, an anaerobic, endospore-forming bacillus.
Virulence factors: Endospores, collagenase, hyaluronidase, DNase.
Transmission: Introduction of endospores into wounds.
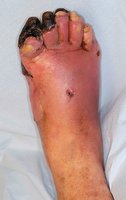
Symptoms: Pain, edema, bloody exudate, black necrotic tissue with gas bubbles.
Treatment: Debridement, antibiotics, hyperbaric oxygen, amputation.
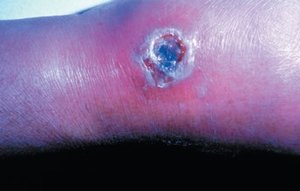
Cutaneous Anthrax (Bacillus anthracis)
Bacillus anthracis causes cutaneous anthrax, a zoonotic disease acquired through contact with infected animals or animal products.
Signs: Black eschar formation, tissue necrosis.
Treatment: Penicillin or ciprofloxacin.
Fungal Skin Infections
Tinea Infections (Ringworm)
Dermatophytes (Trichophyton, Epidermophyton, Microsporum) cause superficial mycoses of the skin, hair, and nails. These infections are named by location (e.g., tinea capitis, tinea pedis).
Virulence factors: Keratinase, persistent spores.
Transmission: Direct/indirect contact with infected humans, animals, or soil.
Treatment: Topical/oral antifungals (miconazole, terbinafine, griseofulvin).
Cutaneous Sporotrichosis
Sporothrix schenckii causes "rose gardener’s disease" after inoculation through skin breaks from contaminated plant matter.
Symptoms: Red, pink, or purple bump at site of entry.
Treatment: Supersaturated potassium iodide (SSKI), itraconazole.
Prevention: Gloves, long sleeves when gardening.
Eye Infections
Normal Biota and Defenses of the Eye
The eye’s normal biota resembles that of the skin. Defenses include tears (lysozyme, lactoferrin), blinking, and mucous membranes.
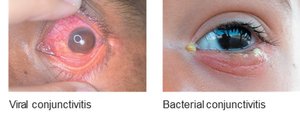
Conjunctivitis (Pink Eye)
Conjunctivitis is inflammation of the conjunctiva, caused by bacteria (Staphylococcus, Streptococcus, Haemophilus influenzae, Neisseria gonorrhoeae, Chlamydia trachomatis) or viruses (adenoviruses, respiratory viruses, HSV in neonates).
Transmission: Highly contagious via direct/indirect contact.
Symptoms: Red/pink sclera, inflammation, discharge (clear in viral, milky in bacterial).
Treatment: Good hygiene, antibiotics for bacterial cases.
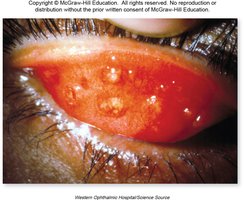
Trachoma
Trachoma is a chronic eye infection caused by Chlamydia trachomatis, leading to blindness if untreated. It is endemic in many developing regions.
Transmission: Contaminated fingers, fomites, flies, hot dry climates.
Symptoms: Pebbled inner eyelid, scarring, inward-turning lashes (trichiasis).
Treatment: Azithromycin or doxycycline; prevention by hygiene and vector control.
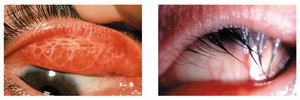
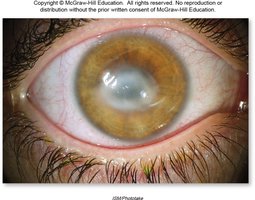
Keratitis
Keratitis is a serious infection of the cornea, caused by HSV-1 or Acanthamoeba (especially in contact lens wearers).
Symptoms: Gritty sensation, conjunctivitis, sharp pain, light sensitivity.
Transmission: HSV-1 reactivation, improper contact lens hygiene, exposure to contaminated water.
Summary Table: Major Skin and Eye Pathogens
Pathogen | Disease | Transmission | Key Features | Treatment/Prevention |
|---|---|---|---|---|
Varicella-Zoster Virus (HHV-3) | Chickenpox, Shingles | Respiratory droplets, direct contact | Vesicular rash, latency | Live vaccine, antivirals |
HSV-1 | Oral herpes, keratitis | Saliva, fomites | Latency, reactivation | Antivirals |
Measles virus | Measles (Rubeola) | Respiratory droplets | Koplik’s spots, rash | MMR vaccine |
Staph. aureus | Impetigo, SSSS | Direct contact, fomites | Pus-filled vesicles, exfoliative toxins | Antibiotics, hygiene |
Strep. pyogenes | Erysipelas, necrotizing fasciitis | Damaged skin | Rapid tissue destruction | IV antibiotics, debridement |
Clostridium perfringens | Gas gangrene | Wounds, trauma | Necrosis, gas bubbles | Debridement, antibiotics |
Bacillus anthracis | Cutaneous anthrax | Contact with animals/products | Black eschar | Penicillin, ciprofloxacin |
Chlamydia trachomatis | Trachoma | Fingers, fomites, flies | Pebbled eyelid, scarring | Azithromycin, hygiene |
Dermatophytes | Tinea (ringworm) | Direct/indirect contact | Itchy, scaly lesions | Antifungals |
