 Back
BackSpecific (Adaptive) Immunity: Mechanisms, Cells, and Responses
Study Guide - Smart Notes

Specific Immunity (Adaptive Immunity)
Overview of Adaptive Immunity
Specific (adaptive) immunity is the branch of the immune system that targets particular pathogens with high specificity and memory. It enables the body to recognize, respond to, and remember specific antigens, providing long-lasting protection. Adaptive immunity is divided into two main branches: humoral (B cell-mediated) and cellular (T cell-mediated) immunity, both of which require the lymphatic system for optimal function.
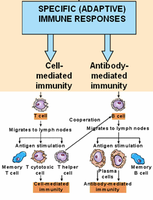
Key Features of Adaptive Immunity
Specificity: Targets unique antigens found on pathogens.
Memory: Generates memory cells that provide faster and stronger responses upon re-exposure to the same antigen.
Systemic Response: Involves the entire body, not just the site of infection.
Self/Non-self Recognition: Distinguishes between the body’s own cells and foreign invaders.
Cells and Organs of Adaptive Immunity
Lymphocytes: B Cells and T Cells
Lymphocytes are the primary cells of adaptive immunity. They originate from stem cells in the bone marrow and differentiate into B cells and T cells. B cells mature in the bone marrow, while T cells mature in the thymus. Both cell types circulate through the lymphatic system and reside in lymph nodes, where they encounter antigens.
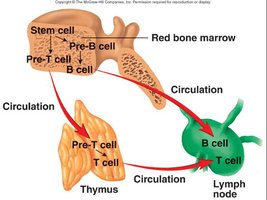
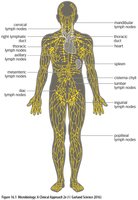
Lymphatic System
The lymphatic system is essential for immune surveillance and the transport of lymphocytes. It includes lymph nodes, the spleen, and mucosa-associated lymphoid tissues (MALT, GALT, BALT), which trap antigens and facilitate their presentation to lymphocytes.
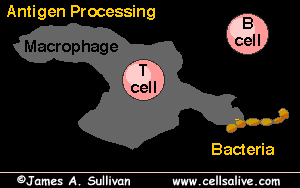
Antigen Recognition and Presentation
Antigen Presenting Cells (APCs)
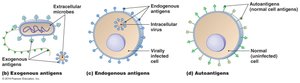
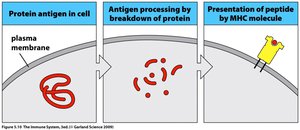
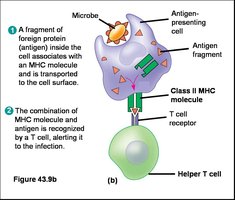
APCs such as dendritic cells, macrophages, and B cells capture antigens, process them, and present antigen fragments on their surface using major histocompatibility complex (MHC) molecules. This presentation is crucial for the activation of T cells.
Major Histocompatibility Complex (MHC)
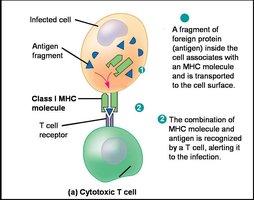
MHC Class I: Found on all nucleated cells; presents endogenous antigens (from within the cell) to CD8+ cytotoxic T cells.
MHC Class II: Found on APCs; presents exogenous antigens (from outside the cell) to CD4+ helper T cells.
Lymphocyte Activation and Differentiation
B Cell and T Cell Receptors
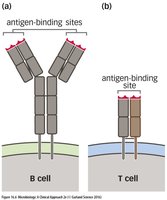
B cells and T cells express unique antigen receptors generated through gene rearrangement. B cell receptors (BCRs) are immunoglobulins with two antigen-binding sites, while T cell receptors (TCRs) have a single antigen-binding site.
Clonal Selection and Central Tolerance
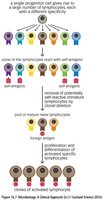
During development, lymphocytes undergo selection to eliminate self-reactive cells (central tolerance). Upon encountering their specific antigen, lymphocytes proliferate and differentiate into effector and memory cells—a process known as clonal selection.
Cell-Mediated Immunity
T Lymphocytes and Their Subtypes
Cell-mediated immunity is primarily carried out by T lymphocytes. Major subtypes include:
Helper T cells (CD4+): Activate B cells and other immune cells via cytokine secretion.
Cytotoxic T cells (CD8+): Kill infected or abnormal cells presenting antigen with MHC I.
Regulatory T cells: Suppress immune responses to maintain tolerance.
Memory T cells: Provide rapid response upon re-exposure to antigen.
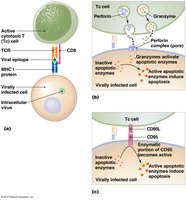
Mechanisms of Cytotoxicity
Cytotoxic T cells induce apoptosis in target cells by releasing perforin and granzymes. This process is essential for eliminating cells infected with intracellular pathogens (e.g., viruses) and cancer cells.
Natural Killer (NK) Cells vs. Cytotoxic T Cells
TC cells: Require antigen presentation via MHC I for activation.
NK cells: Kill cells lacking MHC I or displaying abnormal antigens; activated by cytokines and interferons.
Humoral Immunity
B Cells and Antibody Production
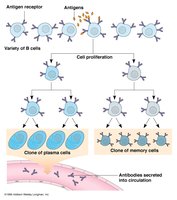
B cells, upon activation by antigen and helper T cells, differentiate into plasma cells that secrete antibodies. Memory B cells are also generated for long-term immunity. Humoral immunity is especially important for defense against extracellular pathogens.
Antibody Structure and Classes
Antibodies (immunoglobulins) are Y-shaped proteins with variable regions for antigen binding and constant regions for effector functions. There are five main classes:
IgM: First antibody produced; effective at complement activation.
IgG: Most abundant in serum; crosses placenta; good at neutralization and opsonization.
IgA: Found in mucosal areas; protects body surfaces.
IgD: Functions mainly as a B cell receptor.
IgE: Involved in allergic responses and defense against parasites.
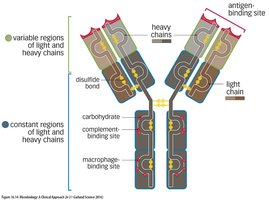
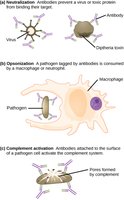
Functions of Antibodies (NIAAO)
Neutralization: Block pathogen binding or toxin activity.
Immobilization: Prevent motility of pathogens.
Agglutination: Clump pathogens for easier clearance.
Activation of Complement: Trigger complement cascade for pathogen lysis.
Opsonization: Enhance phagocytosis by marking pathogens.
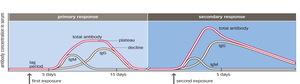
Primary and Secondary Immune Responses
Primary Response
The first exposure to an antigen triggers a primary immune response, characterized by a lag phase and initial production of IgM, followed by IgG. The response is slower and less robust.
Secondary Response
Upon re-exposure to the same antigen, memory cells mount a faster and stronger secondary response, predominantly producing IgG. This principle underlies the effectiveness of vaccination.
Take Home Points
Understand the structure and classes of antibodies, mechanisms of diversity, and clonal selection.
Know the roles and interactions of B cells, T cells, and antigen-presenting cells in humoral and cell-mediated immunity.
Recognize the importance of memory cells in secondary immune responses and the basis of immunization.
Distinguish between passive and active immunization.
