 Back
BackVaccination and Immunization: Principles, Types, and Strategies
Study Guide - Smart Notes

Vaccination and Immunization
Introduction to Vaccination
Vaccination is a cornerstone of modern microbiology and immunology, aiming to generate a protective immune response against pathogens that cause severe illness, disability, or death. By preventing life-threatening infectious diseases, vaccination is estimated to avert 2-3 million deaths per year worldwide.
Active vs. Passive Immunization
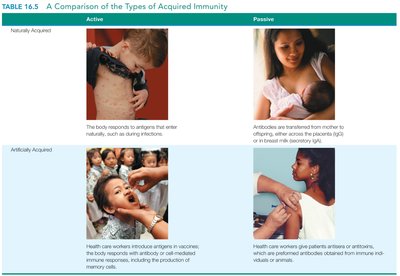
Immunization can be achieved through active or passive means, each with distinct mechanisms and outcomes.
Active Immunization: Administration of antigens to induce an adaptive immune response. The body produces its own antibodies and memory cells, leading to long-term protection.
Passive Immunization: Transfer of antibodies formed by an immune individual or animal. Provides immediate, but temporary, protection.
Examples: Active immunization includes vaccination and natural infection; passive immunization includes maternal antibody transfer and antibody therapy.
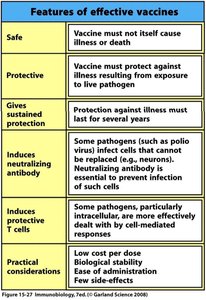
Features of an Effective Vaccine
An effective vaccine must possess several key features to ensure safety and efficacy:
Safe: Must not cause illness or death.
Protective: Must protect against illness resulting from exposure to the live pathogen.
Gives Sustained Protection: Protection should last for several years.
Induces Neutralizing Antibody: Essential for pathogens infecting irreplaceable cells (e.g., neurons).
Induces Protective T Cells: Important for intracellular pathogens.
Practical Considerations: Low cost, biological stability, ease of administration, and few side effects.
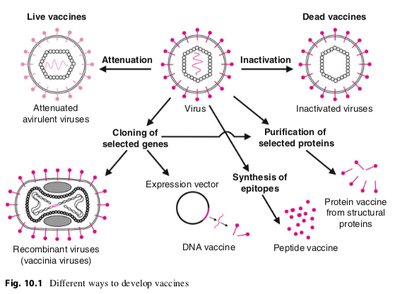
Types of Vaccines
Overview of Vaccine Types
Vaccines are classified based on their composition and method of preparation. The main types include:
Inactivated/Killed Vaccines
Live, Attenuated Vaccines
Toxoid (Inactivated Toxin) Vaccines
Subunit and Conjugate Vaccines
DNA Vaccines
Inactivated/Killed Vaccines
These vaccines are made by inactivating the whole pathogen using heat or chemicals. They are safe, with no risk of reactivation, and can be produced quickly.
Examples: Polio (IPV), Hepatitis A, Rabies
Toxoid Vaccines
Toxoid vaccines are made from toxins produced by bacteria that have been inactivated by heat or chemical treatment. They require intermittent boosters to maintain protective antibody levels.
Examples: Tetanus, Diphtheria
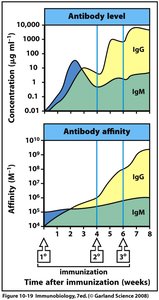
Mechanism: Antibody amount and affinity increase with multiple exposures to the same antigen.

Subunit Vaccines
Subunit vaccines use specific components of a pathogen, such as proteins or polysaccharides, to elicit an immune response. Adjuvants may be added to enhance immunogenicity.
Examples: Hepatitis B, HPV, Pertussis, Influenza (shot), Pneumococcal polysaccharide, Meningococcal polysaccharide
Hepatitis B: Uses recombinant surface antigen protein (HBsAg) expressed in yeast.
Pneumococcal Polysaccharide: Contains mixed polysaccharides from the capsule of multiple Streptococcus pneumoniae serotypes.
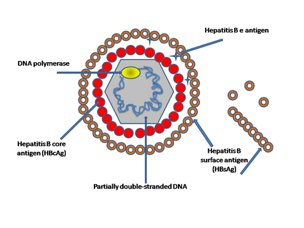
Conjugate Vaccines
Conjugate vaccines are designed to enhance immune responses to carbohydrate antigens by linking them to a carrier protein, such as diphtheria toxoid. This is especially important for infants and others with weak responses to carbohydrates.
Examples: Haemophilus influenzae (HiB), Pneumococcal conjugate, Meningococcal conjugate
Live, Attenuated Vaccines
Live, attenuated vaccines contain organisms that have been weakened so they no longer cause disease but still elicit a strong immune response. Attenuation is achieved by growing pathogens in non-human cells or by recombinant DNA techniques.
Examples: Measles, Mumps, Rubella (MMR), Varicella, Rotavirus, Influenza (nasal spray), Polio (oral – OPV), Yellow Fever, BCG
Risks: Can cause disease in immunocompromised individuals; may revert to wild-type.
Recombinant DNA Attenuation: Deliberate mutations to virulence genes prevent reversion.

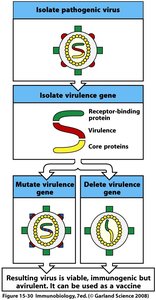
DNA Vaccines
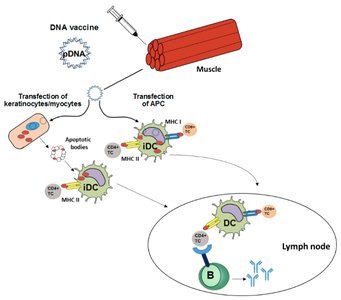
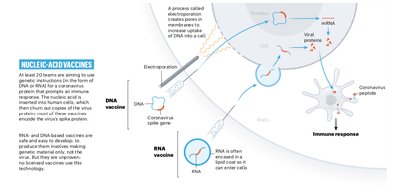
DNA vaccines use plasmid DNA encoding pathogen-specific antigens. The DNA is expressed in antigen-presenting cells (APCs), which present the protein to lymphocytes, inducing adaptive immunity.
Mechanism: Plasmid DNA is injected, taken up by cells, and expressed as antigen.
Vaccine Terminology
Vaccine Antigen: The molecule (protein or carbohydrate) in the vaccine that elicits an antibody response.
Adjuvant: Substance added to vaccines to enhance the immune response by non-specific activation.
Vaccine Titer: A measure of the amount of antibody produced against a vaccine antigen.
Adjuvants and Immune Stimulatory Complexes
Adjuvants
Adjuvants are substances that enhance the immunogenicity of antigens in vaccines. They work by various mechanisms, such as delayed release, enhanced uptake, or stimulation of cytokine production.
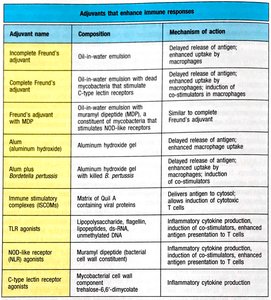
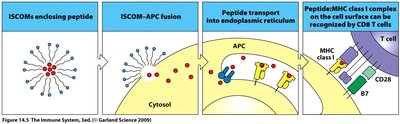
Immune Stimulatory Complexes (ISCOMs)
ISCOMs enhance cytotoxic T cell activation by delivering peptide antigens to the cytosol, facilitating presentation via MHC class I molecules.
Historical Impact and Safety Concerns
Historical Eradication of Smallpox
Vaccination with cowpox (vaccinia) led to the complete eradication of smallpox, demonstrating the power of vaccines in public health.
Vaccine Safety and Public Perception
Concerns over vaccine safety can lead to the resurgence of infectious diseases. It is crucial to communicate the benefits and safety of vaccines to the public.

Summary Table: Types of Acquired Immunity
Type | Active | Passive |
|---|---|---|
Naturally Acquired | Body responds to antigens during infection | Antibodies transferred from mother to offspring |
Artificially Acquired | Health care workers introduce antigens via vaccines | Health care workers give preformed antibodies |

Summary Table: Vaccine Types and Examples
Vaccine Type | Examples | Advantages | Disadvantages |
|---|---|---|---|
Inactivated/Killed | Polio (IPV), Hepatitis A, Rabies | Safe, quick to produce | May require boosters |
Live, Attenuated | MMR, Varicella, OPV, BCG | Strong, long-lasting immunity | Risk in immunocompromised, possible reversion |
Toxoid | Tetanus, Diphtheria | Targets toxin, not pathogen | Requires boosters |
Subunit | Hepatitis B, HPV, Pertussis | Safe, specific | May require adjuvant |
Conjugate | HiB, Pneumococcal conjugate | Enhanced response in infants | Complex production |
DNA | Experimental, COVID-19 | Rapid development, no pathogen | New technology, limited use |
Conclusion
Vaccination is a critical tool in controlling infectious diseases. Understanding the principles, types, and strategies of vaccination enables microbiology students to appreciate its impact on public health and the ongoing challenges in vaccine development and acceptance.
