 Back
BackViruses and Prions: Structure, Genetics, Replication, and Clinical Relevance
Study Guide - Smart Notes

Viruses and Prions
Introduction to Viruses
Viruses are submicroscopic, acellular infectious agents that require a host cell for replication. They are considered nonliving because they lack cellular structure and metabolism. Virology is the study of viruses, which can infect all forms of life, including bacteria (bacteriophages), animals, and plants.
Size: Viruses are extremely small (20–400 nm), much smaller than prokaryotic and eukaryotic cells.
Obligate Intracellular Pathogens: Viruses must infect a host cell to reproduce.
Host Range: Viruses can infect every branch in the tree of life.

Comparison of Viruses, Prokaryotes, and Eukaryotes
Viruses differ fundamentally from prokaryotic and eukaryotic cells in structure, replication, and metabolism.
Characteristic | Viruses | Prokaryotes | Eukaryotes |
|---|---|---|---|
Cells? | No | Yes | Yes |
Considered alive? | No | Yes | Yes |
Relative size | Smaller than prokaryotes | Bigger than viruses, smaller than eukaryotes | Bigger than prokaryotes and viruses |
Structure | Protein capsid, nucleic acid | Cells without nuclei | Cells with nuclei |
Replication | Hijack host machinery | Binary fission | Mitosis/Meiosis |
Metabolism | No | Yes | Yes |
Genome | DNA or RNA | DNA | DNA |
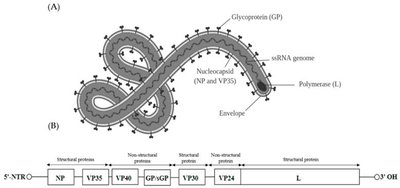
Viral Structure and Genomic Features
Virion Structure
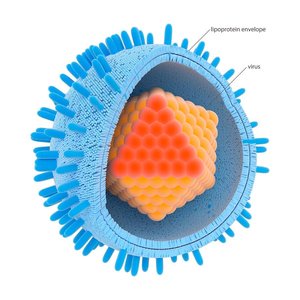
A virion is a single, infectious virus particle. It consists of a protective protein shell called a capsid, which encloses the viral genome (DNA or RNA). Some viruses also possess an outer lipid envelope derived from the host cell membrane.
Capsid Types
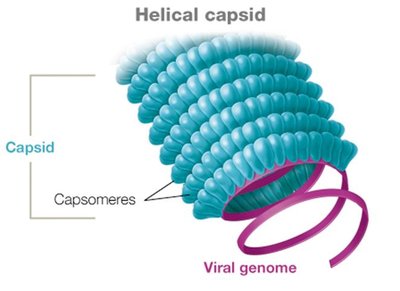
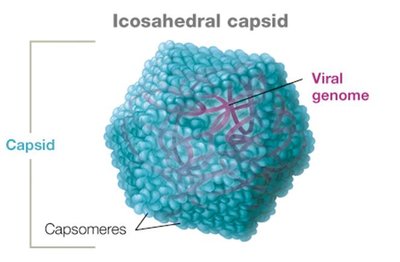
Capsids are made of protein subunits called capsomeres. The main capsid shapes are:
Helical: Hollow tube-like structure (e.g., tobacco mosaic virus).
Icosahedral: Three-dimensional polygon (e.g., adenovirus, coronavirus).
Complex: Irregular shapes, often seen in bacteriophages.
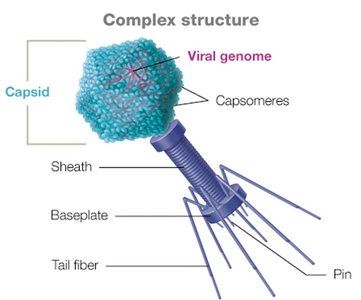
Bacteriophage Capsids
Bacteriophages often have complex capsids with icosahedral heads and additional structures (e.g., tail fibers) for injecting their genome into bacterial cells.
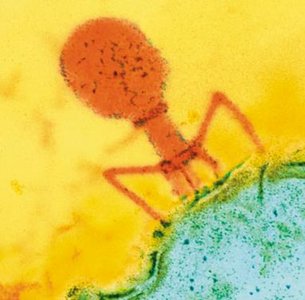
Viral Envelopes
Some viruses are enveloped, possessing a lipid membrane surrounding the capsid, acquired from the host cell during budding. Naked viruses lack this envelope and are released by cell lysis.
Enveloped viruses: e.g., coronaviruses, herpesviruses, influenza.
Naked viruses: e.g., human papillomavirus, poliovirus, all bacteriophages.
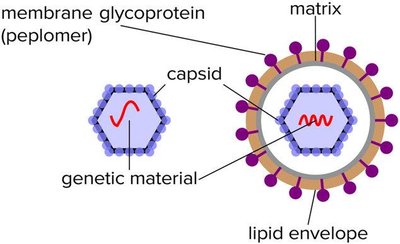
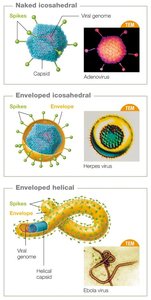
Viral Spikes (Peplomers)
Many viruses have glycoprotein spikes (peplomers) protruding from their surface, which mediate attachment and entry into specific host cells. These spikes are key antigens recognized by the immune system.
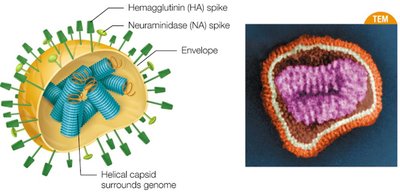
Viral Genomes
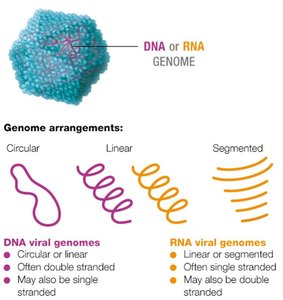
Viral genomes are highly variable and can be composed of DNA or RNA, which may be single- or double-stranded, linear, circular, or segmented. Most viruses have fewer than 300 genes, encoding structural proteins, enzymes for replication, and other factors.
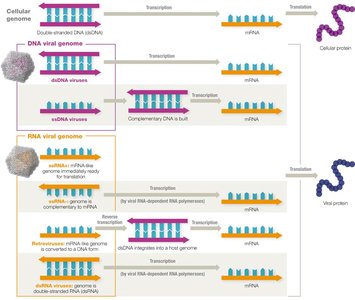
Making mRNA from Viral Genomes
The ultimate goal of all viruses is to direct the host cell to produce viral proteins and assemble new virions. The process of generating mRNA from viral genomes varies depending on the type of nucleic acid present.
Viral Evolution and Genetic Change
Mutation and Reassortment
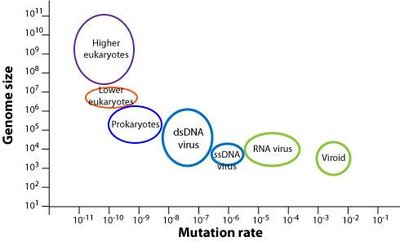
Viruses mutate rapidly due to their short replication cycles and large population sizes. RNA viruses mutate faster than DNA viruses because RNA polymerases lack proofreading ability. Genetic changes can be neutral, beneficial, or detrimental.
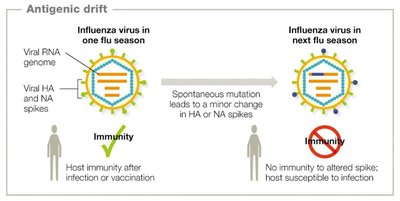
Antigenic drift: Minor changes in viral antigens due to point mutations (e.g., influenza HA and NA spikes).
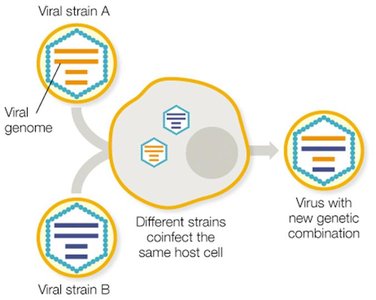
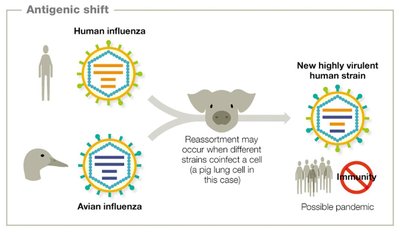
Antigenic shift: Major genetic reassortment, often resulting in new viral strains with pandemic potential.
Classification and Naming of Viruses
Classification Criteria
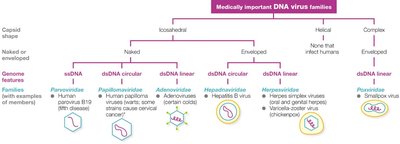
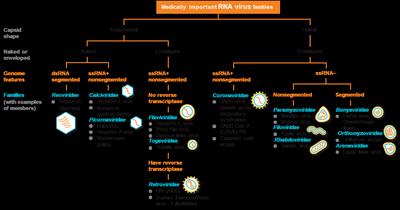
Viruses are classified based on:
Type of nucleic acid (DNA or RNA)
Capsid symmetry (helical, icosahedral, complex)
Presence or absence of an envelope
Genome architecture (e.g., ssDNA, dsRNA)
Naming Conventions
Taxon | Example | Notes |
|---|---|---|
Order | Herpesvirales | Ends in 'virales' |
Family | Herpesviridae | Ends in 'viridae' |
Subfamily | Alphaherpesvirinae | Ends in 'virinae' |
Genus | Simplexvirus | Ends in 'virus' |
Species | Human herpesvirus-1 | Italicized, capitalized |
Host Range and Tropism
Host Range
Host range is the spectrum of species a virus can infect. Some viruses are species-specific (e.g., measles virus infects only humans), while others have a broad host range (e.g., Ebola virus).
Tropism
Tropism refers to the specificity of a virus for particular host tissues or cell types, determined by viral surface factors.
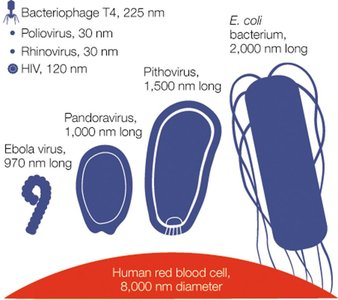
Virus Sizes
Viruses vary greatly in size, but are generally smaller than bacteria. For example, rhinoviruses are about 30 nm, while pithoviruses can reach 1,500 nm.
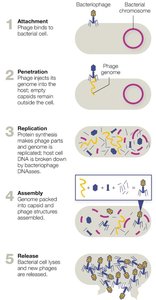
Viral Replication
Bacteriophage Replication
Bacteriophages replicate via the lytic or lysogenic cycle. The lytic cycle results in immediate production of new virions and host cell lysis. The lysogenic cycle involves integration of the phage genome into the host chromosome as a prophage, which can later reactivate.
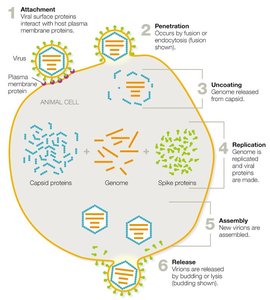
Animal Virus Replication
Animal viruses follow a general replication cycle:
Attachment: Virus binds to host cell receptors.
Penetration: Entry by endocytosis or membrane fusion.
Uncoating: Capsid is removed, releasing the genome.
Replication: Genome is replicated, viral proteins are synthesized.
Assembly: New virions are assembled.
Release: Enveloped viruses bud off; naked viruses lyse the cell.

Persistent Viral Infections and Oncogenesis
Types of Persistent Infections
Chronic: Continuous release of virions (e.g., HIV).
Latent: Periods of dormancy with intermittent flare-ups (e.g., herpesviruses).
Oncogenic Viruses
Oncogenic viruses can cause cancer by promoting uncontrolled cell division or inhibiting cell death. Examples include human papillomavirus (HPV), Epstein–Barr virus, and hepatitis B and C viruses.
Virus | Genome | Integrates? | Cancer Link | Mechanism |
|---|---|---|---|---|
HPV | DNA | Yes | Cervical, oropharyngeal, anal cancers | Uncontrolled cell division |
HTLV | RNA | Yes | Adult T-cell leukemia | Uncontrolled cell division |
Hepatitis B/C | DNA/RNA | No | Liver cancer | Chronic inflammation, DNA damage |
Virus Cultivation and Detection
Growing Viruses
Bacteriophages are grown on bacterial lawns, forming plaques. Animal viruses are grown in tissue culture, embryonated eggs, or live animals.
Diagnostic Methods
Latex agglutination tests: Detect viral antigens or antibodies using latex beads.
ELISA: Detects viral antigens or antibodies via enzyme-linked color change.
Nucleic acid detection: PCR, sequencing, and fluorescent probes for viral genetic material.
Antiviral Drugs and Vaccines
Antiviral Drug Targets
Antiviral drugs target various steps in the viral replication cycle, including attachment, penetration, uncoating, replication, assembly, and release. Most antivirals limit infection rather than cure it.
Nucleoside analogs: Mimic nucleotides, block replication (e.g., acyclovir, ribavirin).
Reverse transcriptase inhibitors: Block retroviral replication (e.g., AZT).
Entry inhibitors: Block viral attachment or fusion (e.g., docosanol, palivizumab).
Interferons: Signal uninfected cells to mount antiviral defenses.
Neuraminidase inhibitors: Block influenza virus release (e.g., oseltamivir).
Vaccines
Vaccines are crucial for preventing viral diseases by training the immune system to recognize and respond to specific viruses.
Prions
Prion Diseases
Prions are infectious proteins that lack genetic material. They cause transmissible spongiform encephalopathies (TSEs), which are fatal neurodegenerative diseases. Prions induce misfolding of normal proteins in the brain, leading to tissue degeneration and characteristic sponge-like holes.
Examples: Creutzfeldt-Jakob disease, mad cow disease.
Diagnosis: Detection of spongiform changes in brain tissue post-mortem.
Some neurodegenerative diseases (e.g., Alzheimer's, Parkinson's, ALS) exhibit prion-like mechanisms, where misfolded proteins propagate disease, but are not infectious in the same way as prions.
Clinical Application: Case Study Questions
Screening old blood samples for new viruses: Use nucleic acid detection methods (e.g., PCR, sequencing) to identify unknown viral genomes.
Classifying a new virus: Determine nucleic acid type, capsid structure, envelope presence, and genome architecture using molecular and microscopic techniques.
Isolating and growing a virus: Inoculate susceptible cell cultures or animal models with patient blood, monitor for cytopathic effects, and confirm viral presence with molecular assays.
Antiviral treatment for RNA viruses: Prescribe nucleoside analogs or reverse transcriptase inhibitors to block viral replication.
Shared genes and immune response: Strong immune reaction in vaccinated animals suggests antigenic similarity between the new virus and hepatitis C virus.
Low viral titers over time: Indicates a persistent, possibly latent or chronic infection with low-level viral replication.
Oncogenic potential: The absence of cancer in most infected individuals does not rule out oncogenicity; other factors (e.g., host genetics, co-infections) may influence cancer development.
