 Back
BackViruses, Disease, and Host Defenses: Study Notes for Microbiology
Study Guide - Smart Notes

Viruses: Structure, Classification, and Life Cycles
Definition and Distinctive Characteristics of Viruses
Viruses are acellular infectious agents that require a host cell to replicate. They are fundamentally different from prokaryotic and eukaryotic cells due to their unique structure and replication strategies.
Obligate intracellular parasites: Viruses cannot reproduce outside a host cell.
Genetic material: They contain either DNA or RNA, but never both.
No cellular structure: Viruses lack organelles, cytoplasm, and a plasma membrane.
Replication: They multiply by assembly of components, not by binary fission or mitosis.
Observation of Viruses
Viruses are much smaller than bacteria and require an electron microscope for visualization due to their size (typically 20–300 nm).
Host and Cellular Specificity
Host specificity: The range of host species a virus can infect, determined by the interaction between viral surface proteins and host cell receptors.
Cellular specificity: The preference of a virus for a particular cell type within a host (e.g., HIV targets CD4+ T cells).
Viral Morphology and Structure
Viruses exhibit several morphological forms, primarily determined by their capsid and presence or absence of an envelope.
Capsid: Protein coat that protects the viral genome.
Envelope: Lipid membrane derived from the host cell, present in some viruses.
Spikes: Glycoprotein projections involved in host cell recognition and attachment.
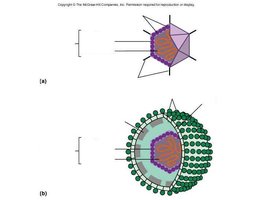
Viral Morphological Forms
Helical
Polyhedral (Icosahedral)
Enveloped
Complex
Viral Nucleic Acids
Viral genomes can be DNA or RNA, single- or double-stranded, linear or circular, and segmented or non-segmented. This diversity distinguishes them from cellular organisms, which have double-stranded DNA genomes.
Bacteriophages and Viral Life Cycles
Bacteriophage: A virus that infects bacteria.
Lytic cycle: Virus replicates and lyses the host cell.
Lysogenic cycle: Viral genome integrates into the host genome and replicates with it without immediate lysis.
Not all viruses are capable of both cycles.
Oncogenic and Oncolytic Viruses
Oncogenic virus: Can cause cancer by transforming normal cells into tumor cells.
Oncolytic virus: Specifically infects and kills cancer cells.
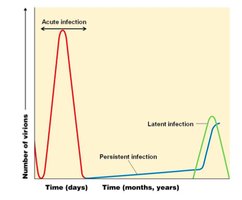
Types of Viral Infections
Acute infection: Rapid onset, short duration (e.g., influenza).
Latent infection: Virus remains dormant and can reactivate (e.g., herpes simplex).
Persistent infection: Virus is continuously present at low levels (e.g., HIV).
Antigenic Shift vs. Antigenic Drift
Antigenic drift: Minor changes in viral antigens due to point mutations (common in influenza).
Antigenic shift: Major changes due to genetic reassortment, leading to new viral subtypes.
Prions
Prion: Infectious protein particles that lack nucleic acids.
Cause diseases such as Creutzfeldt-Jakob disease and mad cow disease.
Prions are not viruses.
Principles of Disease and Epidemiology
Human Microbiome and Microbial Interactions
Human microbiome: The collection of all microorganisms living in and on the human body.
Distribution and composition are influenced by genetics, diet, environment, and antibiotic use.
Normal microbes: Permanently colonize the host.
Transient microbes: Present temporarily.
Symbiosis and Microbial Antagonism
Symbiosis: Close association between two organisms. Types include mutualism, commensalism, and parasitism.
Microbial antagonism: Normal microbiota inhibit the growth of pathogens, which is beneficial to the host.
Pathogenicity and Disease Transmission
Opportunistic pathogens: Cause disease when the host's defenses are compromised.
Etiology: The study of the cause of disease.
Communicable disease: Can be spread from person to person.
Non-communicable disease: Not spread between hosts.
Endemic: Constantly present in a population.
Epidemic: Sudden increase in cases.
Pandemic: Worldwide epidemic.
Types and Patterns of Disease
Acute: Rapid onset, short duration (e.g., influenza).
Chronic: Develops slowly, lasts a long time (e.g., tuberculosis).
Latent: Inactive for a period, then reactivates (e.g., herpes).
Systemic infection: Spread throughout the body.
Focal infection: Confined to a specific area.
Secondary infection: Occurs after a primary infection weakens the host.
Sepsis: Systemic inflammatory response to infection, not only caused by bacteria.
Reservoirs and Transmission of Disease
Reservoir: Source of infectious agents (humans, animals, environment).
Transmission routes: direct contact, indirect contact (fomites), droplet, vector-borne, etc.
Nosocomial (Healthcare-Associated) Infections
Acquired in healthcare settings; major concern due to antibiotic resistance.
Prevention: hand hygiene, sterilization, isolation procedures.
Microbial Mechanisms of Pathogenicity
Portals of Entry and Exit
Microorganisms enter the host via mucous membranes, skin, or parenteral routes (e.g., cuts, injections).
Portal of exit: Path by which pathogens leave the host (e.g., respiratory tract, feces, blood).
Virulence Factors
Virulence: Degree of pathogenicity.
Infectious dose (ID50): Number of microbes required to cause infection in 50% of hosts.
Adhesins: Surface molecules that help pathogens attach to host cells.
Fimbriae: Hair-like appendages for attachment, distinct from adhesins.
Capsules: Protect bacteria from phagocytosis, increasing virulence.
Exoenzymes and Toxins
Exoenzymes: Secreted enzymes that aid in invasion (e.g., coagulases, kinases, hyaluronidase).
Toxins: Poisonous substances produced by pathogens.
Exotoxins: Secreted proteins, often with specific effects (e.g., A-B toxins).
Endotoxins: Lipopolysaccharide components of Gram-negative bacteria, released upon cell death.
Superantigens: Toxins that provoke intense immune responses by stimulating large numbers of T cells.
Cytokines: Immune signaling molecules, can be overproduced in response to superantigens.
Siderophores: Bacterial proteins that scavenge iron from the host.
Comparison of Endotoxins and Exotoxins
Feature | Exotoxins | Endotoxins |
|---|---|---|
Chemical Nature | Proteins | Lipopolysaccharides |
Source | Mostly Gram-positive bacteria | Gram-negative bacteria |
Heat Stability | Unstable | Stable |
Specificity | Specific effects | General effects |
Toxicity | High | Low |
Fever Production | No | Yes |
Immune Evasion and Cytopathic Effects
Viruses evade immunity by antigenic variation, inhibiting antigen presentation, or infecting immune cells (e.g., HIV).
Cytopathic effects: Structural changes in host cells due to viral infection.
Epidemiology and Emerging Diseases
Epidemiology: Study of disease distribution and determinants in populations.
Emerging infectious diseases: New or increasing in incidence (e.g., COVID-19).
Innate Immunity: Nonspecific Defenses of the Host
Lines of Defense
First line: Physical and chemical barriers (skin, mucous membranes).
Second line: Innate immune cells, inflammation, fever, antimicrobial substances.
Third line: Adaptive immunity (specific, memory-based).
Innate vs. Adaptive Immunity
Innate immunity: Non-specific, immediate response.
Adaptive immunity: Specific, slower to develop, has memory.
Key Components of Innate Immunity
Toll-like receptors (TLRs): Recognize pathogen-associated molecular patterns (PAMPs) on microbes.
Cytokines: Mediate and regulate immunity, inflammation, and hematopoiesis.
Normal microbiota: Compete with pathogens, stimulate immune responses.
Leukocytes: White blood cells; include phagocytes (neutrophils, macrophages), lymphocytes, and others.
Phagocytosis: Ingestion and destruction of microbes by phagocytes.
Natural Killer (NK) cells: Destroy infected or abnormal cells; part of innate immunity.
Lymphatic system: Network for immune cell circulation and pathogen filtration.
Inflammation and Fever
Inflammation: Contains infection, removes pathogens, initiates repair.
Fever: Enhances immune response but can be harmful if excessive.
Antimicrobial Substances
Complement system: Cascade of proteins that enhance phagocytosis, lyse microbes, and promote inflammation.
Three outcomes: Opsonization, cytolysis, inflammation.
Interferons: Proteins that inhibit viral replication, especially effective against viruses.
Iron-binding proteins: Sequester iron to inhibit microbial growth.
Antimicrobial peptides: Short proteins that disrupt microbial membranes; microbes rarely develop resistance to them.
