 Back
BackAdaptive Immune System: Structure, Function, and Mechanisms
Study Guide - Smart Notes

Adaptive Immune System
Introduction to Adaptive Immunity
The adaptive immune system is a highly specialized defense mechanism that enables the body to recognize and eliminate specific pathogens and their products. Unlike the innate immune system, adaptive immunity is characterized by specificity, memory, and the ability to distinguish self from non-self.
Purpose: To provide targeted and long-lasting protection against pathogens.
Components: Lymphocytes (B cells and T cells), antigen-presenting cells (APCs), antibodies, and cytokines.
Organization: Adaptive responses are initiated in secondary lymphoid organs such as lymph nodes and the spleen.
Attributes of Adaptive Immunity
Specificity: Targets unique molecular structures (epitopes) on antigens.
Inducibility: Activated only in response to specific antigens.
Clonality: Proliferation of lymphocytes with receptors specific to the encountered antigen.
Unresponsiveness to Self: Normally does not react to self-antigens, preventing autoimmunity.
Memory: Generates a faster and stronger response upon subsequent exposures to the same antigen.
Key Characteristics of Adaptive Immunity
Specific: Recognizes and targets specific epitopes on antigens.
Tolerates Self: Avoids attacking the body's own cells.
Minimal Self-Damage: Regulates responses to minimize collateral tissue damage.
Immunological Memory: Remembers previous encounters for rapid future responses.
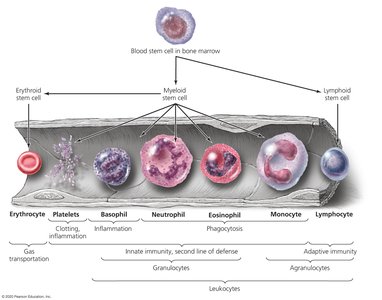
Cells of the Adaptive Immune System
Lymphocytes
Lymphocytes are the primary cells of adaptive immunity, divided into B cells, T cells, and natural killer (NK) cells.
B Cells: Mature in the bone marrow and produce antibodies that neutralize pathogens.
T Cells: Mature in the thymus and are subdivided into:
Helper T cells (CD4+): Coordinate immune responses by secreting cytokines.
Cytotoxic T cells (CD8+): Destroy infected or abnormal cells directly.
Natural Killer (NK) Cells: Part of the innate response, kill infected or cancerous cells without antigen specificity.
Dendritic Cells
Dendritic cells are professional antigen-presenting cells (APCs) that capture antigens in tissues and migrate to lymph nodes to initiate adaptive immune responses. They serve as a bridge between innate and adaptive immunity.
Organization of the Adaptive Immune Response
Secondary Lymphoid Organs
Adaptive immune responses are initiated in secondary lymphoid organs, including lymph nodes, spleen, and Peyer's patches. These organs are sites where antigen-presenting cells interact with and activate naïve lymphocytes.
Antigen Recognition and Specificity
The high specificity of the adaptive immune system is due to antigen-specific receptors on B cells (immunoglobulins) and T cells (T cell receptors). Each lymphocyte expresses receptors for a single antigen specificity.
Clonal Selection and Expansion
Clonal Selection Theory
Clonal selection is the process by which a specific lymphocyte clone is activated by its cognate antigen, leading to proliferation and differentiation into effector and memory cells.
Only lymphocytes with receptors specific to the encountered antigen are selected to expand.
This ensures a tailored and efficient immune response.

Effector Mechanisms of Adaptive Immunity
Helper T Cells (CD4+)
Helper T cells are essential for orchestrating immune responses. They differentiate into subsets based on the cytokines they produce:
Th1 cells: Produce IFN-γ, activate macrophages for intracellular pathogens (cell-mediated immunity).
Th2 cells: Produce IL-4 and IL-5, stimulate B cells for antibody production (humoral immunity).
Th17 cells: Produce IL-17, recruit neutrophils for defense against extracellular bacteria and fungi.
Cytotoxic T Cells (CD8+)
Cytotoxic T cells kill infected or abnormal cells via two main pathways:
Perforin-Granzyme Pathway: Releases perforin to form pores and granzymes to induce apoptosis in target cells.
CD95 Pathway: Engages the CD95 (Fas) receptor on target cells to trigger apoptosis.
B Cells and Antibody Production
B cells, upon activation, differentiate into plasma cells that secrete antibodies. Antibodies mediate several effector functions:
Neutralization: Block pathogen binding to host cells.
Opsonization: Enhance phagocytosis by marking pathogens for ingestion.
Agglutination: Clump pathogens together for easier clearance.
Complement Activation: Trigger the complement cascade for pathogen lysis.
Antibody-Dependent Cellular Cytotoxicity (ADCC): Recruit NK cells to destroy antibody-coated targets.

Classes of Antibodies
There are five main classes of antibodies (immunoglobulins): IgG, IgM, IgA, IgE, and IgD. Each class has distinct structures, functions, and locations in the body.
Class | Structure | Function | Location |
|---|---|---|---|
IgG | Monomer | Main serum antibody, complement activation, opsonization | Blood, extracellular fluid |
IgM | Pentamer | First antibody produced, agglutination, complement activation | Blood |
IgA | Dimer (secretory) | Mucosal immunity | Mucosal surfaces, secretions |
IgE | Monomer | Allergic responses, defense against parasites | Bound to mast cells |
IgD | Monomer | B cell receptor | B cell surface |
Induction of T-Dependent Antibody Immunity
T-dependent antibody responses require cooperation between B cells and helper T cells. The process involves:
Antigen presentation for Th activation and proliferation
Differentiation of helper T cells into Th2 cells
Activation of B cells
Proliferation and differentiation of B cells into plasma and memory cells
Immunological Memory
Memory Cells
Memory B and T cells are long-lived cells generated during the primary immune response. They enable a more rapid and robust response upon re-exposure to the same antigen (secondary response).
Primary Response: Slow, produces small amounts of antibody.
Secondary Response: Rapid, produces large amounts of antibody, mainly IgG.

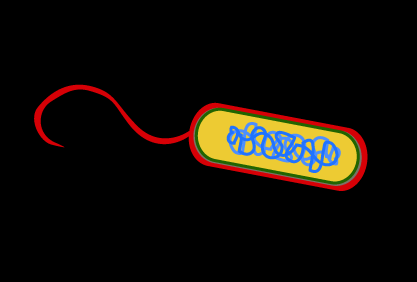
Types of Acquired Immunity
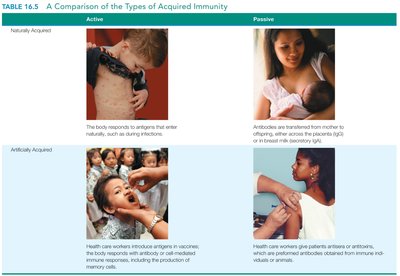
Active vs. Passive Immunity
Acquired immunity can be classified based on how it is obtained:
Active | Passive | |
|---|---|---|
Naturally Acquired | Exposure to pathogens (infection) | Maternal antibodies via placenta or milk |
Artificially Acquired | Vaccination | Injection of immune serum (antibodies) |
Immune Pathology and Autoimmunity
In some diseases, immune responses can cause tissue damage (immune pathology) or target self-antigens (autoimmunity). Examples include Type I diabetes, rheumatoid arthritis, lupus, and multiple sclerosis.
Summary Table: Key Steps in the Adaptive Immune Response
Step | Description |
|---|---|
Recognition | Antigen-presenting cells capture and present antigens to lymphocytes |
Activation | Lymphocytes are activated by antigen and co-stimulatory signals |
Clonal Expansion | Activated lymphocytes proliferate and differentiate |
Effector Function | Effector cells eliminate pathogens via cytotoxicity or antibody production |
Memory | Memory cells persist for rapid future responses |
