 Back
BackAdaptive Immunity: Specific Defenses of the Host (Chapter 17) - Study Guide
Study Guide - Smart Notes

Adaptive Immunity: Specific Defenses of the Host
Overview of Host Defenses
Host defenses against pathogens are divided into innate (nonspecific) and adaptive (acquired) immunity. Innate immunity is present at birth and provides immediate, general protection, while adaptive immunity develops throughout life and is highly specific to particular pathogens.
Susceptibility: Lack of resistance to a disease.
Immunity: The ability to resist a noxious agent, especially pathogens.
Innate Immunity: Genetically inherited, present at birth, includes barriers and specialized cells.
Acquired Immunity: Not present at birth, involves specialized cells and proteins developed in response to infection.
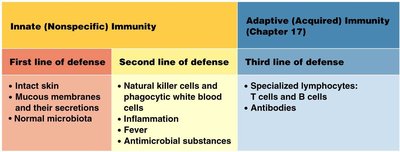
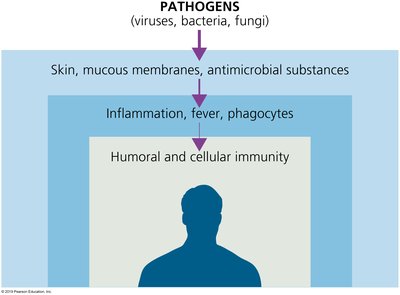
Adaptive Immunity: Key Concepts
Adaptive immunity is characterized by a specific lymphocyte response to antigens, involving B cells and T cells. It is acquired during an individual's lifetime and is divided into humoral and cell-mediated immunity.
Antigen (Ag): A substance that induces the production of specific antibodies or sensitized T cells.
Antibody (Ab): Proteins produced in response to antigens, capable of binding to them.
Humoral Immunity: Mediated by B cells and antibodies, mainly against bacteria, toxins, and viruses.
Cell-mediated Immunity: Mediated by T cells, effective against intracellular pathogens and transplanted tissues.
Cytokines: Chemical messengers that regulate immune responses.
Serology and Immunoglobulins
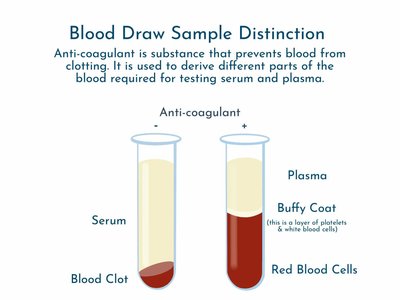
Serology is the study of antibody-antigen interactions. Antiserum refers to serum containing antibodies, and immunoglobulins are the scientific term for antibodies.
Serum: Plasma without fibrinogen.
Gamma globulin: Serum fraction rich in antibodies.
Types of Acquired Immunity
Acquired immunity can be naturally or artificially obtained, and can be active or passive.
Naturally Acquired Active Immunity: Resulting from infection (e.g., lifelong immunity to measles).
Naturally Acquired Passive Immunity: Transfer from mother to infant (transplacental or via breast milk).
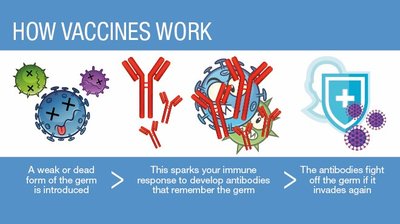
Artificially Acquired Active Immunity: Injection of antigens (vaccination).
Artificially Acquired Passive Immunity: Injection of antibodies from an immune individual or animal.
Antigenic Determinants and Haptens
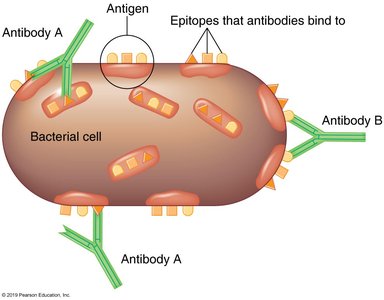
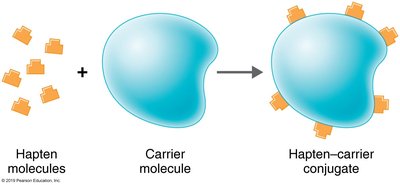
Antibodies recognize specific regions on antigens called epitopes or antigenic determinants. Haptens are small molecules that become antigenic only when attached to a carrier molecule.
Epitopes: Specific regions on antigens where antibodies bind.
Haptens: Low molecular weight compounds requiring a carrier to be antigenic.
Antibody Structure and Antigen-Antibody Binding
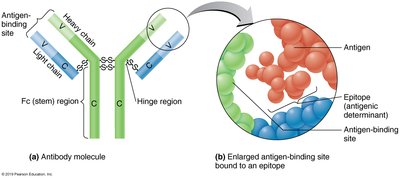
Antibodies are composed of two light chains and two heavy chains linked by disulfide bridges. The variable regions form antigen-binding sites, while constant regions are the same for all antibodies of a class.
Affinity: Strength of the bond between antibody and antigen.
Specificity: Ability of an antibody to recognize a specific epitope.
Protective Mechanisms of Antibodies
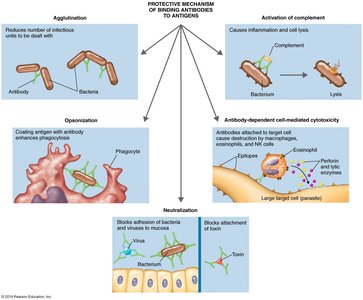
Antibodies protect the host by binding to foreign molecules and tagging them for destruction through various mechanisms.
Phagocytosis: Enhanced by opsonization.
Complement System: Activation leads to lysis of pathogens.
Neutralization: Blocks adhesion of bacteria and viruses to host cells.
Agglutination: Reduces the number of infectious units to be dealt with.
Antibody-dependent cell-mediated cytotoxicity: Targets large parasites.
Antibody Diversity and Self-Tolerance
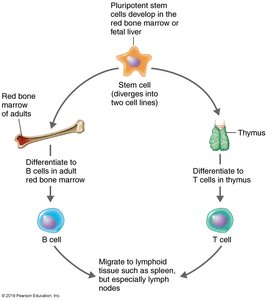
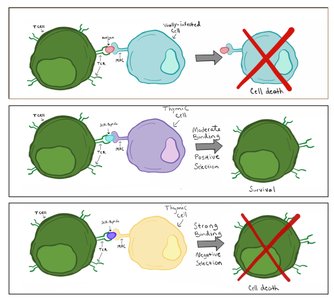
Antibody diversity is generated during embryonic development by combining variable and constant gene regions, resulting in over 1015 different antibodies. Self-tolerance is maintained by clonal deletion, which eliminates B and T cells that react to self-antigens.
Clonal Deletion: Occurs in bone marrow (B cells) and thymus (T cells).
Immunoglobulin Classes
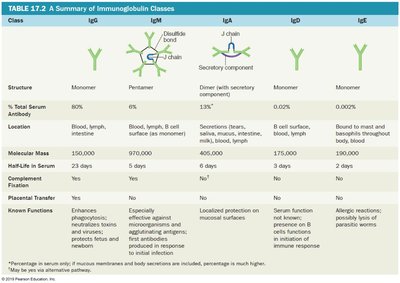
Immunoglobulins are classified into five major classes: IgG, IgM, IgA, IgD, and IgE. Each class has distinct structural and functional properties.
Class | Structure | Location | Half-life | Functions |
|---|---|---|---|---|
IgG | Monomer | Blood, lymph, intestine | 23 days | Enhances phagocytosis, neutralizes toxins, protects fetus |
IgM | Pentamer | Blood, lymph, B cell surface | 5 days | First antibody produced, agglutinates microbes |
IgA | Dimer (with secretory component) | Secretions, blood, lymph | 6 days | Localized protection in mucosal surfaces |
IgD | Monomer | B cell surface, blood, lymph | 3 days | Initiates immune response |
IgE | Monomer | Bound to mast cells, basophils, blood | 2 days | Allergic reactions, parasitic worms |
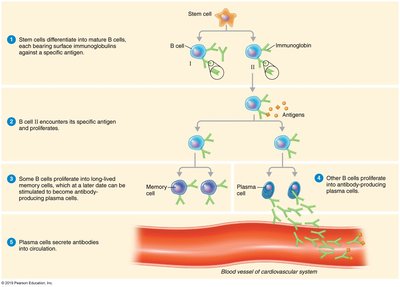
Clonal Selection and B Cell Activation
Clonal selection is the process by which B and T cells develop clones against specific antigens. Mature B cells migrate to lymphoid tissues and recognize epitopes using surface immunoglobulins (IgM and IgD).
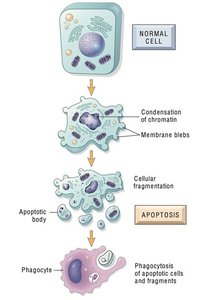
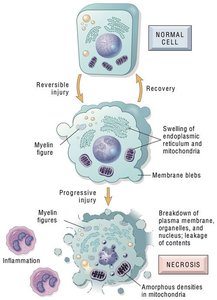
Apoptosis and Necrosis
Apoptosis is programmed cell death, characterized by cellular fragmentation and phagocytosis of cell debris. Necrosis is a violent, unregulated cell death that leads to inflammation.
Apoptosis: Tidy, prevents inflammation.
Necrosis: Messy, induces inflammatory response.
Natural Killer Cells and MHC
Natural killer (NK) cells are lymphoid cells that destroy tumor cells and virus-infected cells, especially those lacking MHC I molecules. MHC (major histocompatibility complex) is a self-antigen not immunologically specific.
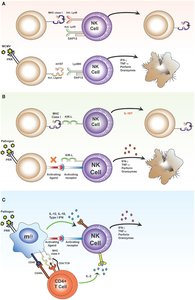
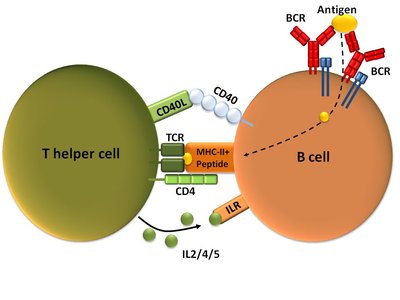
B Cell Activation: T-Dependent and T-Independent Antigens
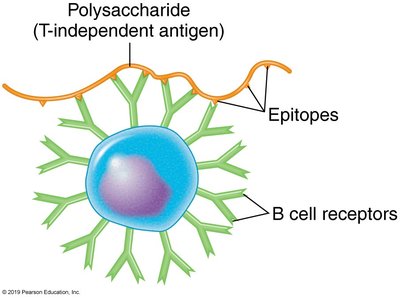
B cells are usually activated by T-dependent antigens, which require the help of T cells. Some antigens, such as capsular polysaccharides, can activate B cells directly (T-independent).
T-Dependent Antigens: Require antigen-presenting cells and T cell help.
T-Independent Antigens: Activate B cells directly, often through repeating epitopes.
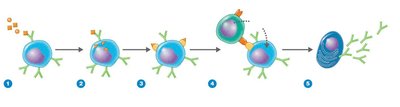
T Cells: Helper, Cytotoxic, and Regulatory
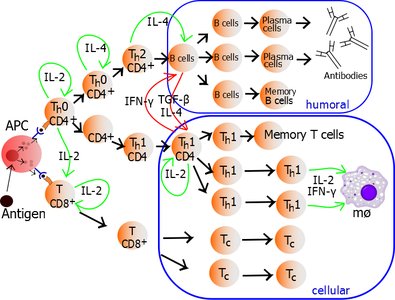
T cells are divided into several types based on their function:
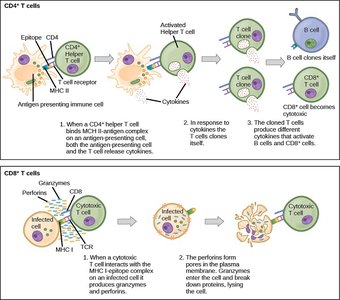
Helper T Cells (CD4): TH1 cells activate cell-mediated immunity and macrophages; TH2 cells activate B cells for antibody production and are important in allergic reactions.
Cytotoxic T Cells (CD8): Differentiate into cytotoxic T-lymphocytes (CTLs) that destroy target cells using perforin.
Regulatory T Cells (TR): Suppress other T cells to prevent autoimmunity.
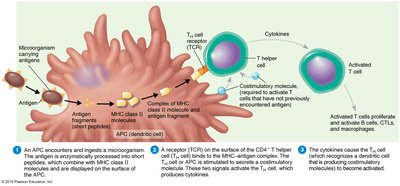
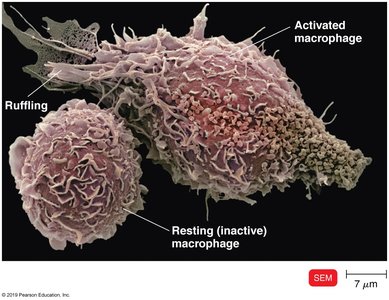
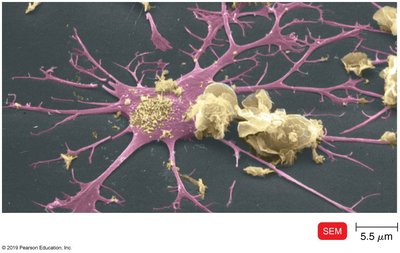
Antigen-Presenting Cells (APCs)
APCs such as dendritic cells and macrophages are essential for inducing immune responses by presenting antigens to T cells. Activated macrophages are stimulated by ingesting antigens or cytokines.
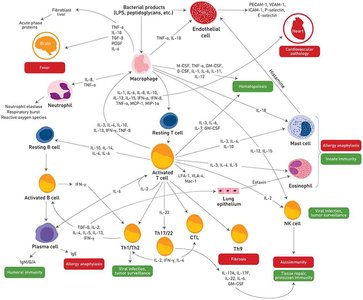
Cytokines and Chemokines
Cytokines are signaling molecules used by immune cells to communicate and regulate immune responses. Chemokines specifically attract leukocytes to sites of infection.
Interleukin-1: Stimulates TH cells.
Interleukin-2: Activates TH, B, TC, and NK cells.
Interleukin-8: Attracts phagocytes.
Interleukin-10: Interferes with TH1 cell activation.
Interleukin-12: Differentiation of CD4 cells.
γ-interferon: Increases activity of macrophages.
Chemokines: Cause leukocytes to move to infection.
 ----------------------------------------
----------------------------------------
