Back
BackAdaptive Immunity: Specific Defenses of the Host
Study Guide - Smart Notes

Adaptive Immunity: Specific Defenses of the Host
Overview of Adaptive Immunity
Adaptive immunity refers to the body's ability to recognize and specifically target particular pathogens through a highly specialized response. Unlike innate immunity, which provides general defense, adaptive immunity is acquired through exposure to antigens via infection or vaccination. It is characterized by a primary response (first exposure) and a more rapid, robust secondary response due to immunological memory.
Primary response: The initial immune reaction to a specific antigen.
Secondary response: Enhanced and faster response upon subsequent exposures to the same antigen, mediated by memory cells.
Dual Nature of the Adaptive Immune System
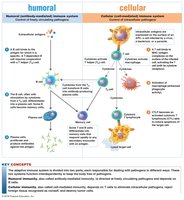
The adaptive immune system consists of two main branches: humoral immunity and cellular immunity, each targeting different types of pathogens.
Humoral immunity: Mediated by B lymphocytes (B cells) that produce antibodies to combat extracellular pathogens such as bacteria and toxins.
Cellular immunity: Mediated by T lymphocytes (T cells) that target intracellular pathogens, including viruses, some fungi, and parasites.
Additional info: B cells mature in the bone marrow, while T cells mature in the thymus. Both cell types originate from stem cells in the bone marrow or fetal liver.
Cytokines: Chemical Messengers of Immune Cells
Cytokines are signaling molecules that regulate the intensity and duration of immune responses. They are produced in response to stimuli and have various functions:
Interleukins: Mediate communication between leukocytes.
Chemokines: Induce migration of leukocytes to infection sites.
Interferons (IFNs): Inhibit viral replication in host cells.
Tumor necrosis factor (TNF): Involved in inflammation and autoimmune diseases.
Hematopoietic cytokines: Regulate the development of blood cells.
Overproduction of cytokines can result in a potentially harmful condition known as a cytokine storm.
Antigens and Antibodies
Antigens, Epitopes, and Haptens
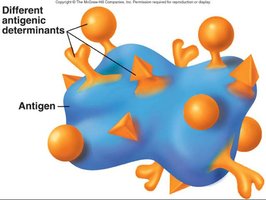
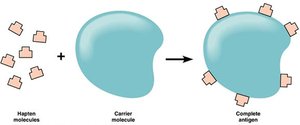
Antigens are substances that provoke an immune response, typically by stimulating the production of antibodies. Antibodies recognize specific regions on antigens called epitopes or antigenic determinants. Some small molecules, known as haptens, are not immunogenic by themselves but can elicit an immune response when attached to larger carrier molecules.
Antigen: Any substance that can induce an immune response.
Epitope: The specific part of an antigen recognized by an antibody.
Hapten: A small molecule that becomes antigenic only when attached to a carrier.
Structure and Function of Antibodies
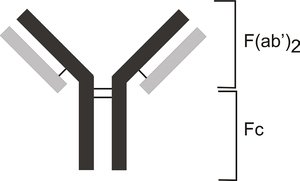
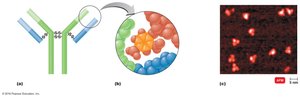
Antibodies, or immunoglobulins (Ig), are Y-shaped globular proteins composed of two identical heavy chains and two identical light chains, joined by disulfide bonds. The variable regions at the tips of the Y bind to specific epitopes, while the constant (Fc) region determines the antibody class and mediates effector functions.
Valence: Number of antigen-binding sites (bivalent antibodies have two).
Five classes of immunoglobulins: IgG, IgM, IgA, IgD, IgE, each with distinct functions.
Summary of Immunoglobulin Classes
Class | Main Function |
|---|---|
IgG | Most abundant; crosses placenta; enhances phagocytosis, neutralizes toxins and viruses |
IgM | First antibody produced in response; effective in agglutination |
IgA | Found in secretions (mucus, saliva, tears); protects mucosal surfaces |
IgD | Functions mainly as a B cell receptor |
IgE | Involved in allergic reactions and defense against parasitic worms |
Additional info: The valence of IgM is 10, IgA is 4 (dimeric form), and IgG, IgD, IgE are 2.
Antigen–Antibody Binding and Its Results
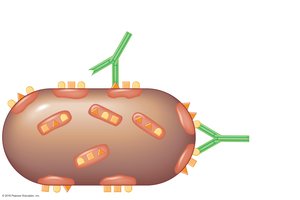
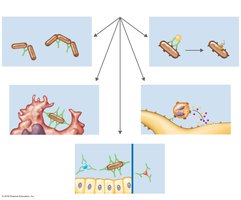
When antibodies bind to antigens, they form antigen–antibody complexes that protect the host by marking pathogens for destruction. The main outcomes include:
Agglutination: Clumping of pathogens for easier removal.
Opsonization: Coating of antigens to enhance phagocytosis.
Antibody-dependent cell-mediated cytotoxicity (ADCC): Destruction of large pathogens by immune cells.
Neutralization: Blocking pathogen attachment to host cells.
Activation of complement: Triggering a cascade that leads to cell lysis.
Humoral Immunity Response Process
Clonal Selection and Differentiation of B Cells
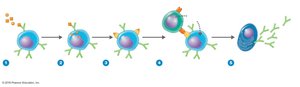
B cells recognize antigens via surface immunoglobulins. Upon antigen binding, B cells internalize and process the antigen, presenting fragments on MHC class II molecules. T helper cells (TH) recognize these fragments and secrete cytokines, activating B cells to proliferate and differentiate into plasma cells (which secrete antibodies) and memory cells (which provide long-term immunity).


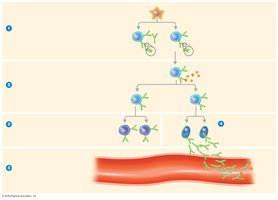
Major Histocompatibility Complex (MHC)
Class I MHC: Present on all nucleated cells; present endogenous antigens to cytotoxic T cells.
Class II MHC: Present on antigen-presenting cells (APCs); present exogenous antigens to helper T cells.
Cellular Immunity Response Process
Role of T Cells and Antigen-Presenting Cells (APCs)
T cells mature in the thymus and are responsible for combating intracellular pathogens. They recognize antigens presented by APCs via T-cell receptors (TCRs). Pathogens entering the gastrointestinal tract are sampled by M cells, which transfer antigens to lymphocytes and APCs.
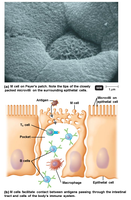
Types and Functions of T Cells
T helper cells (CD4+): Activate B cells, macrophages, and other T cells; recognize antigens presented with MHC class II.
T cytotoxic cells (CD8+): Destroy infected or abnormal self-cells; recognize antigens presented with MHC class I.
T regulatory cells (Treg): Suppress immune responses to maintain self-tolerance and prevent autoimmunity.
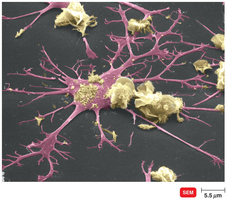
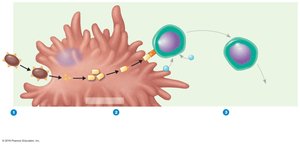
Subsets of T Helper Cells
TH1 cells: Activate macrophages and cytotoxic T cells; promote phagocytosis and cell-mediated immunity.
TH2 cells: Stimulate B cells to produce IgE; activate eosinophils for defense against parasites.
TH17 cells: Secrete IL-17; recruit neutrophils and promote inflammation against extracellular bacteria and fungi.
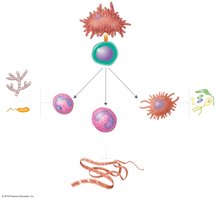
Mechanisms of Cytotoxic T Cell Action
Cytotoxic T lymphocytes (CTLs) recognize and kill infected or abnormal cells presenting endogenous antigens with MHC class I. Upon activation, CTLs release perforin and granzymes, inducing apoptosis in target cells.
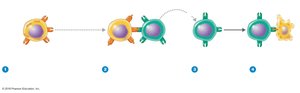
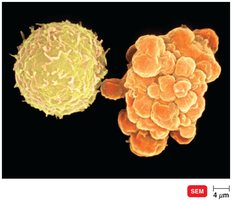
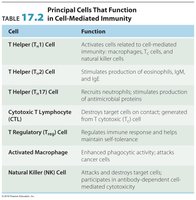
Principal Cells in Cell-Mediated Immunity
Cell | Function |
|---|---|
T Helper (TH1) | Activates cells related to cell-mediated immunity |
T Helper (TH2) | Stimulates production of eosinophils, IgM, and IgE |
T Helper (TH17) | Recruits neutrophils; stimulates production of antimicrobial proteins |
Cytotoxic T Lymphocyte (CTL) | Destroys target cells on contact |
T Regulatory (Treg) | Regulates immune response; maintains self-tolerance |
Activated Macrophage | Enhances phagocytic activity; attacks cancer cells |
Natural Killer (NK) Cell | Attacks and destroys target cells; participates in antibody-dependent cell-mediated cytotoxicity |
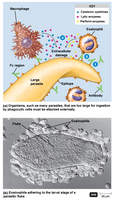
Antibody-Dependent Cell-Mediated Cytotoxicity (ADCC)
ADCC is a mechanism by which immune cells lyse large pathogens, such as protozoans and helminths, that are too large to be phagocytosed. Antibodies bind to the target cell, and immune cells attach to the Fc region, releasing cytotoxic substances to destroy the target.
Immunological Memory
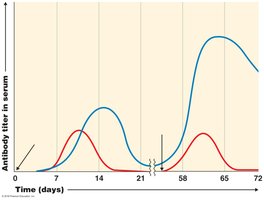
Primary and Secondary Immune Responses
The primary immune response occurs upon first exposure to an antigen and is characterized by a lag phase before antibody production. The secondary response is faster, stronger, and longer-lasting due to the presence of memory cells. IgM is produced first, followed by IgG.
Types of Adaptive Immunity
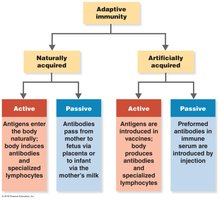
Classification of Adaptive Immunity
Naturally acquired active immunity: Immunity developed after exposure to antigens in daily life (e.g., infection).
Naturally acquired passive immunity: Transfer of antibodies from mother to fetus or infant (e.g., via placenta or breast milk).
Artificially acquired active immunity: Immunity developed after vaccination.
Artificially acquired passive immunity: Injection of preformed antibodies (e.g., antiserum).
Summary: Dual Nature of the Adaptive Immune System
The adaptive immune system is divided into humoral and cellular branches, each responsible for targeting different types of pathogens. Humoral immunity involves B cells and antibody production, while cellular immunity involves T cells that eliminate intracellular pathogens and regulate immune responses.