 Back
BackChapter 12: Adaptive Immunity – Mini-Textbook Study Notes
Study Guide - Smart Notes

Adaptive Immunity
Overview of Adaptive Immunity
The adaptive immune system is a highly specialized defense mechanism that provides specific and long-lasting protection against pathogens. Unlike innate immunity, adaptive responses take longer to develop but are highly specific to particular antigens and generate immunological memory, allowing for rapid and effective responses upon subsequent exposures.
Primary exposure: Response takes several days to a week; symptoms may occur.
Secondary exposure: Response is rapid and often prevents symptoms.
Two main branches: Cellular (T cell–mediated) and Humoral (antibody–mediated) immunity.
General Steps in an Adaptive Immune Response
Four Main Stages
Both cellular and humoral responses follow these stages to eliminate antigens and establish memory:
Antigen Presentation
Lymphocyte Activation
Lymphocyte Proliferation and Differentiation
Antigen Elimination and Memory
Cells of Adaptive Immunity
Lymphocytes: T Cells and B Cells
Lymphocytes are the primary leukocytes of adaptive immunity:
T cells: Produced in bone marrow, mature in thymus; involved in both cellular and humoral immunity.
B cells: Produced and mature in bone marrow; coordinate humoral response by producing antibodies.
Each lymphocyte expresses thousands of identical receptors, each specific for a single epitope.
Antigen Features
Definition and Properties
An antigen is any substance that can trigger an immune response. The immune system's response depends on the antigen's size, molecular complexity, and chemical composition. Most antigens are proteins or polysaccharides from pathogens.
Haptens: Incomplete antigens that require attachment to a larger molecule to elicit a response.
Epitopes: Specific regions of an antigen recognized by B or T cell receptors.
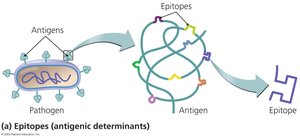
Receptors and Antigen Recognition
TCRs and BCRs
Each T cell receptor (TCR) or B cell receptor (BCR) is specific for a single epitope. The diversity of these receptors is generated by gene shuffling, allowing the immune system to recognize virtually any antigen.
TCR: Recognizes one epitope; involved in cellular immunity.
BCR: Recognizes one epitope; involved in humoral immunity.
Self-Tolerance in Lymphocytes
Screening for Self-Tolerance
To prevent autoimmunity, T and B cells undergo screening to ensure they do not react to self-antigens:
T cells: Screened in the thymus for recognition of self-MHC and non-reactivity to self-antigens.
B cells: Screened in the bone marrow to prevent production of self-reactive antibodies.
Cells failing self-tolerance undergo apoptosis.
Major Histocompatibility Complexes (MHC)
Classes and Functions
MHC molecules are glycoproteins on cell membranes that present antigenic epitopes to T cells. There are two main classes:
MHC I: Present on all nucleated cells (except RBCs); identifies cells as self and presents intracellular antigens to cytotoxic T cells.
MHC II: Present only on antigen-presenting cells (APCs) such as macrophages, B cells, and dendritic cells; presents extracellular antigens to helper T cells.
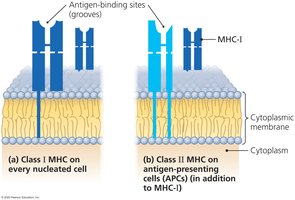
Antigen Location and MHC Presentation
Intracellular antigens: Presented by MHC I (e.g., viral proteins, cancer cell antigens).
Extracellular antigens: Presented by MHC II (e.g., bacterial, fungal, or parasitic antigens).
Cellular Response of Adaptive Immunity
Stages of T Cell Response
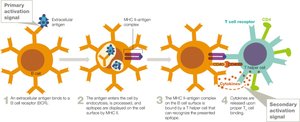
Stage 1: Antigen Presentation – Intracellular antigens are presented by MHC I to cytotoxic T cells; extracellular antigens are presented by MHC II to helper T cells.
Stage 2: T Cell Activation – Requires two signals: TCR-MHC interaction and co-stimulatory signals.
Stage 3: Proliferation and Differentiation – Activated T cells proliferate and differentiate into effector and memory cells.
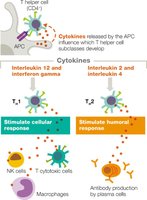
Stage 4: Antigen Elimination – Cytotoxic T cells induce apoptosis in infected or abnormal cells; helper T cells coordinate immune responses via cytokines.
MHC-I Presenting Intracellular Antigens
Intracellular antigens are processed and presented by MHC I to cytotoxic T cells, which then determine if the cell is self or infected.
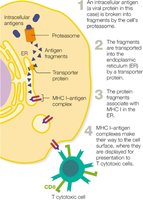
MHC-II Presenting Extracellular Antigens
APCs phagocytize extracellular antigens, process them, and present them via MHC II to helper T cells.
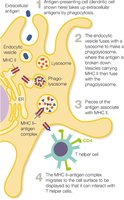
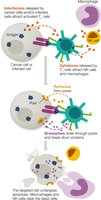
Antigen Elimination by T Cells
Cytotoxic T cells release perforins and granzymes to induce apoptosis in target cells. Helper T cells release cytokines to activate other immune cells.
Humoral Response of Adaptive Immunity
Stages of B Cell Response
Stage 1: Antigen Presentation – B cells can be activated by T-dependent or T-independent antigens.
Stage 2: B Cell Activation – T-dependent activation requires help from T helper cells; T-independent activation occurs with repetitive antigens.
Stage 3: Proliferation and Differentiation – Activated B cells proliferate and differentiate into plasma cells (antibody producers) and memory B cells.
Stage 4: Antigen Elimination – Antibodies neutralize, opsonize, and agglutinate antigens, and activate complement.
T-Dependent B Cell Activation
Most antigens require T helper cell assistance for full B cell activation. The process involves antigen binding, processing, MHC II presentation, and cytokine signaling from T helper cells.
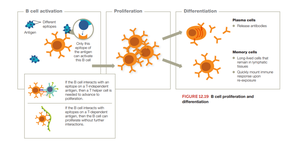
B Cell Proliferation and Differentiation
Activated B cells proliferate and differentiate into plasma cells (which secrete antibodies) and memory B cells (which provide long-term immunity).
Antibody Structure and Isotypes
Antibody Structure
Antibodies (immunoglobulins) are Y-shaped molecules composed of two heavy and two light chains, each with variable and constant regions. The variable region forms the antigen-binding site, while the constant region determines the antibody class.
Antibody Isotypes
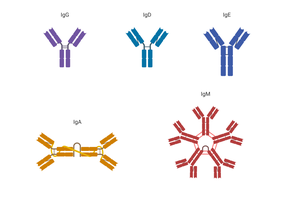
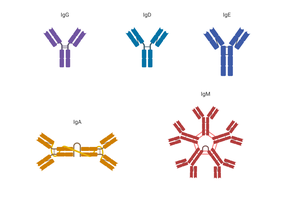
There are five main antibody isotypes, each with distinct functions and locations:
Isotype | Structure | Main Features |
|---|---|---|
IgG | Monomer | Most abundant in serum; crosses placenta; produced second in primary infection |
IgA | Dimer/Monomer | Most abundant in mucosal secretions; protects mucosal surfaces |
IgM | Pentamer/Monomer | First produced in primary infection; largest; effective in blood |
IgD | Monomer | B cell receptor; regulatory role |
IgE | Monomer | Lowest in serum; involved in allergic reactions and defense against parasites |
Immunological Memory
Primary vs. Secondary Response
Primary exposure to an antigen generates IgM first, then IgG. Secondary exposure triggers a rapid, high-affinity IgG response due to memory B and T cells, providing long-term protection.
Acquisition of Humoral Immunity
Types of Adaptive Immunity
Naturally acquired active immunity: Infection triggers immune response; long-term protection.
Naturally acquired passive immunity: Antibodies received (e.g., maternal); temporary protection.
Artificially acquired active immunity: Vaccination; long-term protection.
Artificially acquired passive immunity: Antibody administration (antiserum); temporary protection.
Additional info: The adaptive immune system's ability to generate a vast diversity of antigen receptors is due to somatic recombination and hypermutation processes in lymphocytes. Memory cells are the basis for the effectiveness of vaccines and long-term immunity.
