 Back
BackImmunization, Immunoassays, and Immune Disorders: Study Notes
Study Guide - Smart Notes

Immunization and Immunoassays
Primary vs. Secondary Antibody Response
The immune system responds differently to first and subsequent exposures to an antigen. Understanding these responses is crucial for vaccine development and immunological testing.
Primary Antibody (Ab) Response: The initial antibody response following vaccination or natural infection. It is typically slower and produces lower levels of antibodies.
Secondary Antibody (Ab) Response: The 'memory' response that occurs after a second exposure (booster vaccination or reinfection). It is faster and produces higher levels of antibodies due to memory B cells.
Immunization: Artificial Immunity
Immunization can be achieved actively or passively, each with distinct mechanisms and applications.
Active Immunization: Administration of antigens to stimulate the patient's own adaptive immune response (e.g., vaccines).
Passive Immunotherapy: Transfer of preformed antibodies from an immune individual or animal to provide immediate protection.
Types of Vaccines
Vaccines are designed to safely induce immunity. They vary in composition and method of preparation.
Attenuated (Modified Live) Vaccines: Contain live pathogens rendered avirulent. They induce strong, long-lasting immunity. Examples: Measles, Mumps, Rubella (MMR), Chickenpox, Smallpox vaccines.
Inactivated (Killed) Vaccines: Contain pathogens killed by chemicals (e.g., formalin). May be whole-agent or subunit and require adjuvants to enhance immunogenicity. Examples: Killed Polio, Influenza, Hepatitis vaccines.
Toxoid Vaccines: Contain inactivated bacterial toxins. Examples: Diphtheria, Tetanus, Pertussis toxoids (DPT/DTaP vaccine).
Combination Vaccines: Combine antigens from multiple pathogens for simultaneous administration. Example: MMR vaccine.
Vaccines Using Recombinant Gene Technology: Use genetic engineering to produce antigens. Example: Rabies gene inserted into vaccinia virus for oral immunization of wild animals.
Passive Immunization and Immunotherapy
Passive immunization provides immediate, short-term protection by administering preformed antibodies or immune molecules.
Antiserum (Animal or Human): Used for individuals not vaccinated or exposed to rare diseases.
Cytokines: Such as interferons to decrease viral replication or stimulate immune cell activity (e.g., in cancer therapy).
Hematopoietic Growth Factors: Stimulate production of blood cells, especially in immunosuppressed patients.
Monoclonal Antibodies: Identical antibodies produced from a single plasma cell clone (hybridoma technology). Used in diagnostics and cancer therapy.
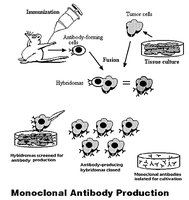
Limitations of Passive Immunization: Can cause serum sickness, antibodies are rapidly degraded, and do not provide long-term protection. Monoclonal antibodies overcome some of these limitations.
Medicinal Uses of Monoclonal Antibodies
Diagnostic Reagents: Used to detect human antibodies, MHC antigens, and pathogens.
Cancer Immunotherapy: Monoclonal antibodies target and kill cancer cells, especially in lymphomas and leukemias.
Serology and Serological Tests
Serology involves the detection of antibodies or antigens in patient samples to diagnose diseases.
Precipitation Tests: Detect soluble antigen-antibody complexes.
Agglutination Tests: Detect clumping of insoluble particles (e.g., blood typing, pathogen detection).
Neutralization Tests: Assess the ability of antibodies to neutralize pathogens or toxins.
ELISAs (EIAs): Enzyme-linked immunosorbent assays for sensitive, quantitative detection of antibodies or antigens.
Agglutination and Hemagglutination
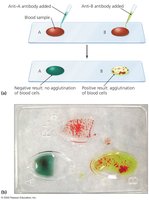
Agglutination is the visible clumping of particles by antibodies, useful for blood typing and pathogen detection.
Hemagglutination: Agglutination of red blood cells, used to determine blood type.
ELISA and Point-of-Care Immunoassays
ELISA is a widely used immunoassay that employs enzyme-labeled antibodies to detect antigens or antibodies. Point-of-care tests provide rapid results for clinical decision-making.
Advantages of ELISA: High sensitivity, quantification, easy automation, and cost-effectiveness.
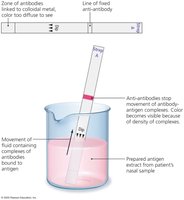
Point-of-Care Tests: Immunofiltration and immunochromatography assays (e.g., rapid strep, COVID, pregnancy tests) provide quick results.
Immune Disorders
Immunodeficiency Diseases
Immunodeficiencies result from defective immune mechanisms, leading to increased susceptibility to infections.
Primary Immunodeficiency Diseases: Congenital, genetic, or developmental defects present at birth (rare).
Acquired Immunodeficiency Diseases: Develop after birth due to aging, stress, malnutrition, or infections (e.g., AIDS caused by HIV destroying CD4+ T cells).
Hypersensitivity Diseases
Hypersensitivities are exaggerated immune responses causing tissue damage. All types require prior sensitization to the antigen.
Type I (Immediate): Rapid allergic reactions (e.g., hay fever, asthma, anaphylaxis) mediated by IgE and mast cells. Treatment includes antihistamines and epinephrine for anaphylaxis.
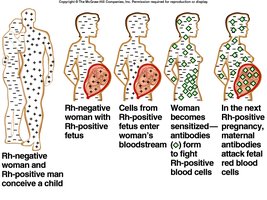
Type II (Cytotoxic): Antibody-mediated destruction of cells (e.g., blood transfusion reactions, Rh incompatibility, autoimmune hemolytic anemia).
Type III (Immune Complex Disease): Deposition of large antigen-antibody complexes in tissues, causing inflammation and tissue damage (e.g., glomerulonephritis, lupus, rheumatoid arthritis).
Type IV (Delayed): Cell-mediated reactions (e.g., TB skin test, contact dermatitis, graft rejection) involving T cells and macrophages, not antibodies.
Types of Grafts
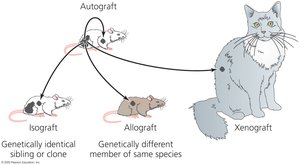
Transplantation immunology classifies grafts based on genetic relationship between donor and recipient.
Autograft: From the same individual.
Isograft: From a genetically identical individual (twin or clone).
Allograft: From a genetically different member of the same species.
Xenograft: From a different species.
Immunologically Privileged Sites
Certain body sites (e.g., cornea, brain, testes) are less likely to reject grafts due to unique immune characteristics, such as lack of lymphatic drainage or low MHC expression.
Graft-versus-Host Disease
Occurs when transplanted immune cells attack the recipient's tissues, often after allogeneic stem cell transplantation. Immunosuppressive therapy is required to prevent severe complications.
Autoimmune Diseases
Autoimmunity arises when the immune system attacks self-antigens, leading to tissue damage. It is more common in the elderly and can be systemic or organ-specific.
Systemic Autoimmune Diseases: Affect multiple organs (e.g., systemic lupus erythematosus, rheumatoid arthritis).
Single-Organ Autoimmune Diseases: Target specific organs (e.g., type 1 diabetes mellitus, multiple sclerosis, hemolytic anemia).
