 Back
BackInnate Immunity: Principles and Mechanisms
Study Guide - Smart Notes

Innate Immunity
Overview of Immune Responses
The immune system orchestrates physiological processes to eliminate antigens and protect the host from infection. Immunity refers to specific protection conferred by immune responses, while susceptibility indicates vulnerability to infection by a given pathogen. The immune system is divided into innate and adaptive branches, both of which recognize diverse pathogens, eliminate invaders, and distinguish self from non-self antigens.
Innate Immunity: Inborn, non-specific, and generalized responses present in all multicellular organisms.
Adaptive Immunity: Found only in vertebrates, matures over time, is highly specific, and exhibits memory.
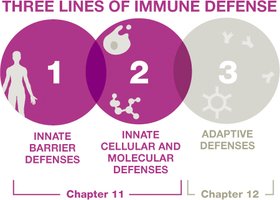
Additional info: Adaptive immunity typically requires 4–7 days to fully activate and is covered in detail in subsequent chapters.
Role of Normal Microbiota
Normal microbiota play a central role in inducing, training, and calibrating immune responses. The good hygiene hypothesis suggests that reduced microbial diversity in our microbiota may negatively affect immune development, as shown by underdeveloped immune systems in germ-free animals.
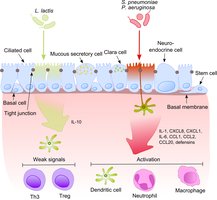
Lines of Defense
First-line Defenses
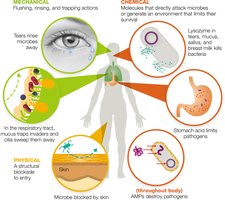
First-line defenses prevent pathogen entry and are categorized as mechanical, chemical, and physical barriers.
Mechanical Barriers: Rinse, flush, or trap pathogens (e.g., tears, urine, saliva, mucus membranes, mucociliary escalator).
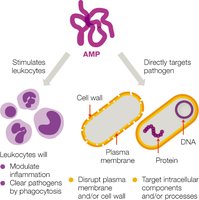
Chemical Barriers: Directly attack invaders or create hostile environments (e.g., lysozyme in secretions, stomach acid, fatty acids in sweat and earwax, antimicrobial peptides such as defensins).
Physical Barriers: Structures that block pathogen entry (e.g., skin, tightly packed epithelial cells of the epidermis).
Second-line and Third-line Defenses
If pathogens bypass first-line barriers, they encounter second-line defenses (molecular factors and leukocytes) and third-line defenses (T and B lymphocytes of the adaptive immune response).
Organs, Tissues, Cells, and Molecules of the Immune System
Lymphatic System
The immune system is closely linked to the lymphatic system, which collects, circulates, and filters fluid in body tissues before returning it to the blood.
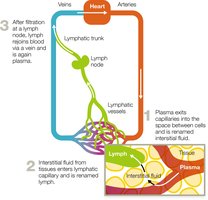
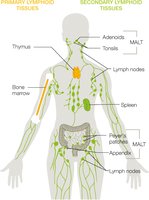
Primary and Secondary Lymphoid Tissues
Primary Lymphoid Tissues: Sites of leukocyte production and maturation (thymus for T cells, bone marrow for red and white blood cells).
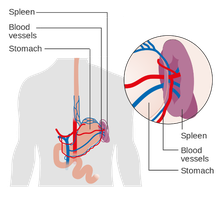
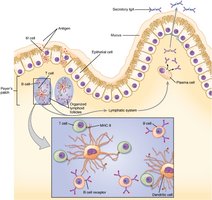
Secondary Lymphoid Tissues: Filter lymph and include lymph nodes, spleen, and mucosa-associated lymphoid tissue (MALT).
Leukocytes (White Blood Cells)
Leukocytes are essential immune cells, classified as granulocytes (with cytoplasmic granules) or agranulocytes (without granules).
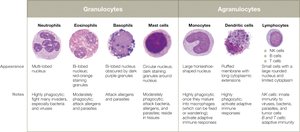
Granulocytes
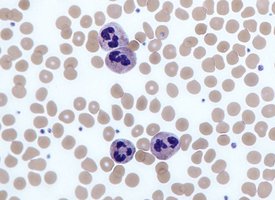
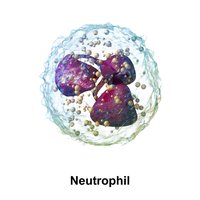
Neutrophils: Most numerous, first responders, phagocytic, release antimicrobial peptides (AMPs).
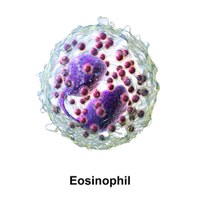
Eosinophils: Combat parasites, moderate phagocytic activity, granules contain enzymes and toxins.
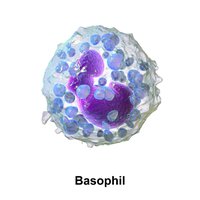
Basophils: Involved in allergic responses and parasitic infections, granules contain histamine.
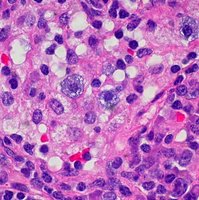
Mast Cells: Reside in tissues, release histamine, involved in allergies and parasite defense, capable of phagocytosis.
Agranulocytes
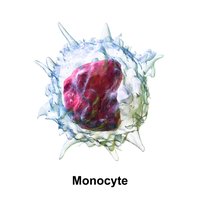
Monocytes: Largest agranular WBCs, mature into macrophages in tissues, elevated in chronic infections and inflammation.
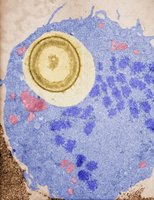
Macrophages: Highly phagocytic, can be fixed (tissue-resident) or wandering.
Dendritic Cells: Highly phagocytic, patrol tissues, present antigens to adaptive immune cells.
Lymphocytes: Include natural killer (NK) cells (innate immunity), B cells, and T cells (adaptive immunity).
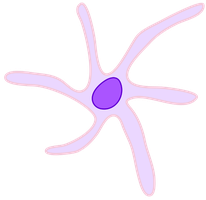
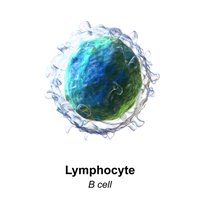
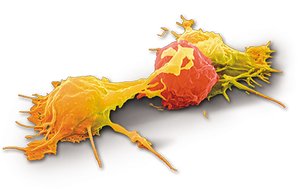
White Blood Cell Counts as Clinical Measures
Differential WBC counts are rapid, inexpensive diagnostic tools. Leukocytosis is an increase, and leukopenia is a decrease, in leukocyte numbers. Specific patterns can indicate different types of infections or immune responses.
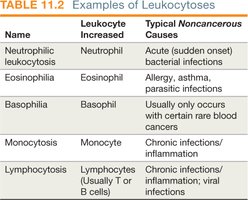
Immune System Molecules
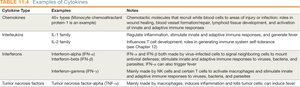
Cytokines: Signaling proteins for cell communication and immune coordination.
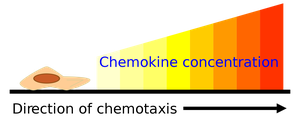
Chemokines: Induce chemotaxis, recruit cells to infection sites, and aid in tissue repair.
Interleukins (ILs): Activate immune responses, regulate inflammation, and stimulate hematopoiesis.
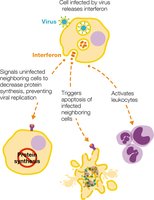
Interferons (IFNs): Signal viral infection, induce antiviral defenses, and activate leukocytes.
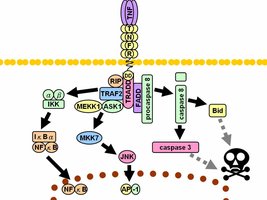
Tumor Necrosis Factors (TNFs): Stimulate inflammation, fever, and can kill tumor cells.
Iron-Binding Proteins and Pathogen Strategies
The body limits free iron to restrict microbial growth using proteins such as hemoglobin, ferritin, lactoferrin, and transferrin. Some pathogens produce siderophores to steal iron or lyse red blood cells to access hemoglobin.
Complement System
The complement system consists of over 30 proteins that, when activated, enhance immune defenses through a cascade. The three main outcomes are:
Opsonization: Tagging invaders for phagocytosis.
Membrane Attack Complex (MAC) Formation: Causes cytolysis of pathogens.
Inflammation: Promotes recruitment of immune cells and pathogen clearance.
Inflammation
Mechanisms and Phases
Inflammation is a key innate defense, triggered by tissue damage or infection. It recruits immune defenses, limits pathogen spread, and promotes tissue repair. The three phases are:
Vascular Changes: Vasodilation and increased vessel permeability allow immune cells and proteins to access tissues.
Leukocyte Recruitment: Chemoattractants guide leukocytes to the site; cells exit vessels via margination and diapedesis.
Resolution: Signals tone down inflammation, clear exudate, and initiate tissue repair.
Cardinal Signs of Inflammation
Redness
Pain
Localized heat
Swelling
Loss of function
Inflammatory Mediators
Histamine: Increases vessel permeability, produced by mast cells, basophils, eosinophils, and platelets.
Kinins: Induce vascular changes and pain, assist in clotting.
Eicosanoids: Prostaglandins, leukotrienes, and thromboxanes; induce vascular changes and pain. NSAIDs and SAIDs reduce eicosanoid production.
Chronic Inflammation
Chronic inflammation results from prolonged immune activation, causing tissue injury and contributing to diseases such as atherosclerosis, certain cancers, and neurodegenerative disorders.
Fever
Mechanisms and Effects
Fever (pyrexia) is an abnormally high systemic body temperature, induced by pyrogens such as bacterial toxins and cytokines (IL-1, TNF-α, IFN-α). The hypothalamus raises the body's temperature set point in response.
Low-grade fever (37.5°C to 38.3°C): Considered protective, enhances interferon effects, phagocyte efficiency, leukocyte production, limits pathogen growth, and promotes tissue repair.
High fever (>40.5°C): Life-threatening, can denature essential enzymes and proteins; above 43°C is fatal.
Antipyretics (e.g., aspirin, ibuprofen, acetaminophen) are used to lower fever by limiting prostaglandin production in the hypothalamus.
Summary Table: Leukocyte Types and Functions
Type | Appearance | Function |
|---|---|---|
Neutrophil | Multi-lobed nucleus, granules | Phagocytosis, first responder, AMPs release |
Eosinophil | Bi-lobed nucleus, red-orange granules | Combat parasites, moderate phagocytosis |
Basophil | Double-lobed nucleus, granules | Release histamine, allergy, parasite defense |
Mast cell | Granules, tissue-resident | Release histamine, allergy, phagocytosis |
Monocyte | Large, horseshoe-shaped nucleus | Mature into macrophages, phagocytosis |
Dendritic cell | Star-shaped | Phagocytosis, antigen presentation |
Lymphocyte | Large nucleus, little cytoplasm | NK cells (innate), B and T cells (adaptive) |
Summary Table: Cytokine Types and Functions
Cytokine Type | Examples | Notes |
|---|---|---|
Chemokines | Monocyte chemoattractant protein-1 | Induce chemotaxis, wound healing, lymphoid tissue development |
Interleukins | IL-1, IL-2 family | Regulate inflammation, activate immune responses, fever, apoptosis |
Interferons | IFN-α, IFN-β, IFN-γ | Antiviral responses, activate macrophages and NK cells |
Tumor necrosis factor | TNF-α | Stimulates inflammation, fever, kills tumor cells |
