 Back
BackInnate Immunity: Structure and Function in Host Defense
Study Guide - Smart Notes

Innate Immunity
Overview of Immune Responses
The immune system protects the body from pathogens through coordinated physiological processes. Immune responses are classified as either innate or adaptive. Both branches recognize diverse pathogens, eliminate invaders, and discriminate between self and foreign antigens.
Innate immunity: Inborn, ancient protection present in all eukaryotes; provides generalized, nonspecific responses.
Adaptive immunity: Found only in vertebrates; matures over time, responds specifically to pathogens, and exhibits memory.
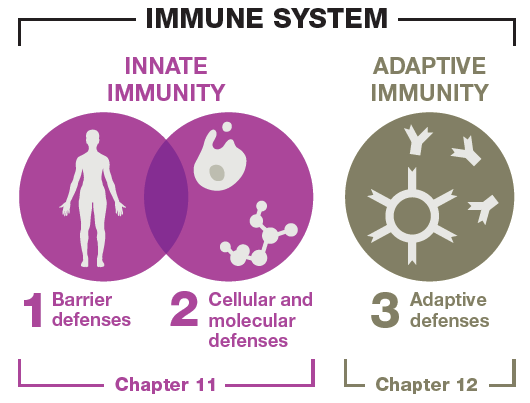
Major Components of Host Defenses
Immunity consists of three collaborating lines of defense:
First-line defenses: Prevent pathogen entry.
Second-line defenses: Cellular and molecular responses after breach of first-line defenses.
Third-line defenses: Adaptive immune responses (covered in Chapter 12).
The Role of Normal Microbiota
Normal microbiota are symbiotic microbes living in and on the body. They fine-tune the immune system to fight pathogens and tolerate nonpathogens, food, and self-tissues. Disruptions in microbiota can lead to immune confusion and overreaction against harmless agents.
First-Line Defenses
Types of First-Line Defenses
First-line defenses are subcategorized as mechanical, chemical, and physical barriers. Their goal is to prevent pathogen entry.
Mechanical barriers: Rinse, flush, or trap pathogens (e.g., tears, urine, saliva, mucus membranes).
Chemical barriers: Attack invaders or create hostile environments (e.g., lysozyme, hydrochloric acid, sweat, sebum, antimicrobial peptides).
Physical barriers: Structures that physically block pathogen entry (e.g., epithelial tissue, skin epidermis).
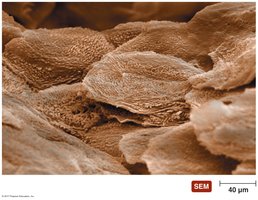
Physical Barriers: Epithelial Tissue
Epithelial tissue lines every body cavity and entrance. The epidermis of the skin is composed of tightly compacted dead epithelial cells called the stratum corneum, which is cornified and keratinized, providing a robust barrier against pathogens.
The Lymphatic System
Structure and Function
The immune system is interconnected with the lymphatic system, which collects, circulates, and filters fluid in body tissues before returning it to the blood. The lymphatic system consists of vessels, lymph fluid, organs, and cells.
Primary lymphatic organs: Red bone marrow (site of B cell maturation and blood cell production) and thymus gland (site of T cell maturation).
Secondary lymphoid tissues: Lymph nodes, spleen, MALT, GALT; serve as filtering and screening centers for lymph.
Second-Line Defenses
Leukocytes (White Blood Cells)
Leukocytes are essential in all immune responses. They are divided into granulocytes and agranulocytes, many of which exhibit phagocytosis.
Neutrophils: Most numerous; first responders; phagocytize foreign cells and viruses.
Dendritic cells: Found in most tissues; modulate immune responses.
Monocytes: Largest agranular WBCs; mature into macrophages in tissues.
Macrophages: Largest, long-lived phagocytes; can be fixed or wandering.
Basophils: Involved in inflammation and allergic reactions; release histamine and serotonin.
Mast cells: Reside in tissues; release histamine.
Eosinophils: Involved in worm infections and allergies; moderate phagocytic properties.
Lymphocytes: Include NK cells (innate protection) and B/T cells (adaptive immunity).
Molecular Second-Line Defenses
Leukocytes release molecules into the local environment to recruit immune cells, restrict pathogen growth, generate fever, and induce inflammation.
Cytokines: Signaling proteins for cell communication; include interleukins, interferons, and tumor necrosis factor.
Iron-binding proteins: Restrict pathogen access to iron.
Complement system: Over 30 proteins working in a cascade to boost immune defenses.
Cytokines: Interferons
Virus-infected cells produce IFN-alpha and IFN-beta to stimulate nearby cells to mount antiviral defenses.
Complement Cascades
The complement system is activated by three pathways:
Classical pathway: Triggered by antibodies bound to invaders.
Alternative pathway: Direct interaction with invaders.
Lectin pathway: Requires mannose-binding lectin.
All pathways result in:
Opsonization: Tags invaders for phagocytosis.
Cytolysis: Formation of membrane attack complex (MAC).
Inflammation: Promotes immune cell recruitment.
Inflammation
Functions and Signs
Inflammation is a key innate defense and essential for healing. Its chief functions are to mobilize immune components, repair tissue, and destroy/block microbes. Cardinal signs include:
Redness: Increased circulation and vasodilation.
Pain: Stimulation of nerve endings.
Localized heat: Increased blood flow.
Swelling: Fluid escape into tissues.
Phases of Inflammation
Vascular changes: Vasodilation and increased vessel permeability due to histamine, prostaglandins, kinins.
Leukocyte recruitment: Cytokines attract leukocytes; neutrophils and monocytes exit vessels via diapedesis.
Resolution: Inflammation subsides, healing begins, pus and dead cells are cleared.
Chronic Inflammation
Chronic inflammation is not protective and can exacerbate tissue injury, promoting diseases such as atherosclerosis, certain cancers, and neurodegenerative disorders.
Fever: A Systemic Innate Immune Response
Mechanism and Sources
Fever (pyrexia) is an abnormally high body temperature induced by pyrogens that signal the hypothalamus to raise the body's baseline temperature. Pyrogens can be exogenous (from infectious agents) or endogenous (released by immune cells).
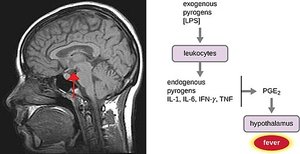
Functions and Ranges of Fever
Enhances antiviral effects of interferons
Increases phagocyte efficiency
Enhances leukocyte production
Limits pathogen growth
Promotes tissue repair
Fever ranges:
Low grade: 99.5°F to 101°F (protective)
High: 104°F to 105°F (seek medical care)
Above 109.4°F: Fatal
Treatment for low to moderate fever (102-103°F): ibuprofen and acetaminophen, which limit prostaglandin production in the hypothalamus.
Summary Table: First-Line Defenses
Barrier Type | Mechanism | Examples |
|---|---|---|
Mechanical | Rinse, flush, trap pathogens | Tears, urine, saliva, mucus membranes |
Chemical | Attack invaders, hostile environment | Lysozyme, stomach acid, sweat, sebum, AMPs |
Physical | Block pathogen entry | Epithelial tissue, skin epidermis |
