 Back
BackMicrobial Mechanisms of Pathogenicity: Structured Study Notes
Study Guide - Smart Notes

Microbial Mechanisms of Pathogenicity
Introduction to Bacterial Pathogenesis
Bacterial pathogenesis refers to the process by which bacteria cause disease in a host. This process involves several distinct steps, each critical for the successful establishment of infection and subsequent disease development.
Pathogenesis: The process of disease development (infection) in a host.
Key Steps: Exposure, adhesion, invasion, multiplication, and damage to the host.
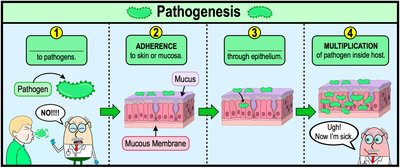
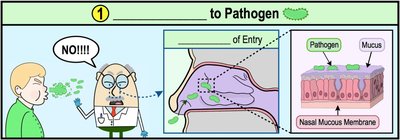
Step 1: Exposure to Pathogen
The first step in pathogenesis is exposure to the pathogen. Not all exposures result in infection; the pathogen must enter host tissues via a portal of entry.
Portal of Entry: Locations where host tissue cells directly contact the external environment (e.g., skin, mucous membranes, parenteral routes).
Most Common Portal: The respiratory tract (e.g., spread of SARS-CoV-2).
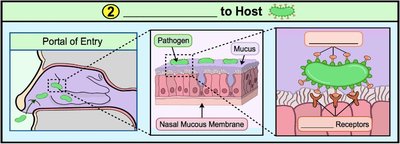
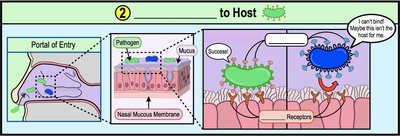
Step 2: Adhesion to Host
After exposure and entry, the pathogen must adhere to the host. Adhesion is mediated by specific molecules called adhesins, which bind to host cell receptors.
Adhesion: Ability of a pathogen to attach to host cells using adhesion factors (adhesins).
Adhesins: Molecules on the surface of pathogens (found on pili, fimbriae, flagella) that bind specific receptors on host cells.
Specificity: Adhesin-receptor binding is highly specific and determines the cell type a pathogen will adhere to.
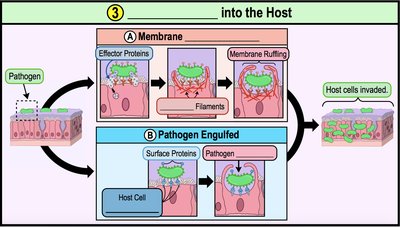
Step 3: Invasion into Host Cells or Tissues
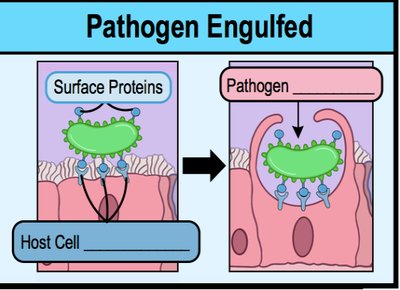
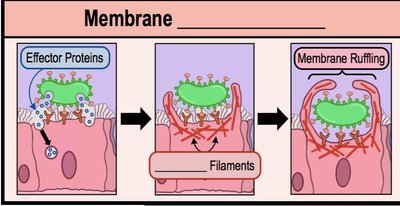
Once adhered, pathogens invade host cells or tissues. This allows them to evade immune responses and access nutrients. Invasion often involves induced endocytosis or membrane ruffling.
Induced Endocytosis: Pathogen manipulates host cell to engulf it, often through secretion of effector proteins.
Membrane Ruffling: Rearrangement of actin filaments in host cell, resulting in membrane ruffles that enclose the pathogen.
Surface Proteins: Pathogen expresses proteins that bind to host cell receptors, facilitating engulfment.
Step 4: Multiplication (Colonization) Inside Host
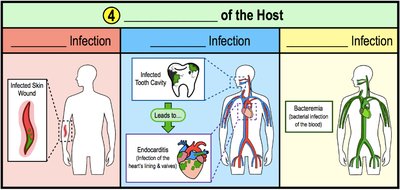
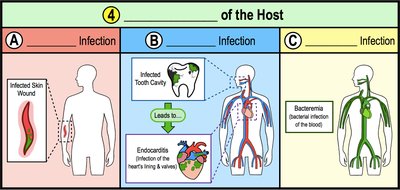
After entering host cells or tissues, pathogens multiply and cause infection. The infection can be local, focal, or systemic depending on its spread.
Local Infection: Confined to a specific area near the portal of entry.
Focal Infection: Localized infection spreads to a secondary location, often via the bloodstream.
Systemic Infection: Infection disseminates throughout the entire body.
Pathogenic Toxins
Introduction to Pathogenic Toxins
Some pathogens produce biological poisons called toxins, which allow them to invade and damage host tissues. Toxins are classified into two main groups: exotoxins and endotoxins.
Toxigenicity: Ability of a pathogen to produce toxins that damage host cells.
Exotoxins: Soluble proteins released by pathogens during infection or following lysis.
Endotoxins: Lipopolysaccharide (LPS) found on the outer membrane of gram-negative bacteria.
Exotoxins: Types and Effects
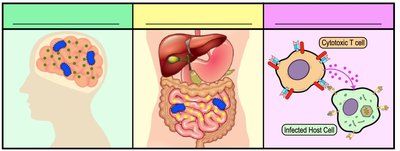
Exotoxins are highly specific and can be grouped based on the tissue they affect or their structure and function.
Neurotoxins: Damage nervous system tissues, potentially causing paralysis.
Enterotoxins: Damage gastrointestinal tract tissues, causing diarrhea and vomiting.
Cytotoxins: Damage various cell types by interfering with cellular mechanisms or causing cell death.
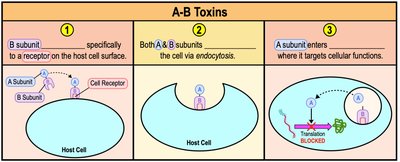
A-B Toxins
A-B toxins consist of two parts: the A (active) subunit, which is enzymatic and responsible for toxic activity, and the B (binding) subunit, which determines cell specificity.
Stepwise Action: B subunit binds to host cell receptor, both subunits enter via endocytosis, A subunit targets cellular functions.
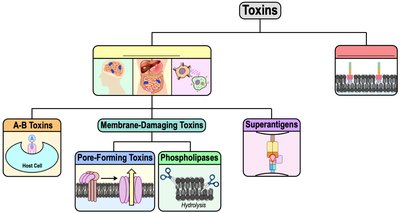
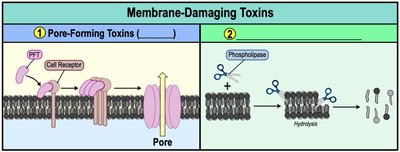
Membrane-Damaging Toxins
These exotoxins disrupt cytoplasmic membranes and cause lysis of host cells. They include pore-forming toxins and phospholipases.
Pore-Forming Toxins (PFTs): Create pores in the phospholipid bilayer, causing cell lysis.
Phospholipases: Enzymes that hydrolyze phospholipids in the membrane.
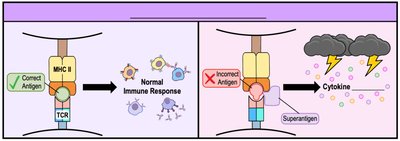
Superantigens
Superantigens are exotoxins that inappropriately stimulate T helper (TH) cells, leading to excessive cytokine production (cytokine storm), which can be life-threatening.
Mechanism: Bind MHC II on antigen-presenting cells, causing TH cells to respond to antigens they normally would not.
Effects: Excessive proliferation of TH cells and massive cytokine release.
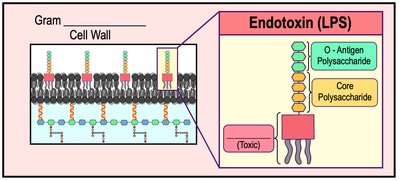
Endotoxins: Structure and Effects
Endotoxins are components of the outer membrane of gram-negative bacteria, specifically the lipopolysaccharide (LPS) molecule. The toxic component is Lipid A.
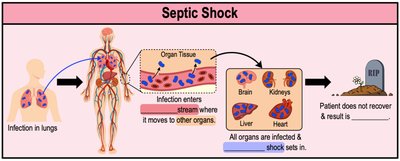
Lipid A: Triggers inflammatory responses and can cause septic shock if released into the bloodstream.
Septic Shock: Systemic response including fever, anemia, weakness, diarrhea, inflammation, and rapid dilation of blood vessels.
Exotoxins vs. Endotoxins
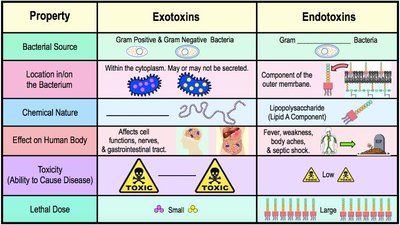
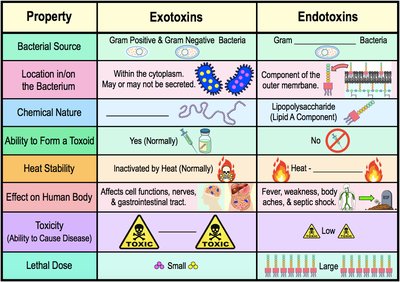
Exotoxins and endotoxins differ in their source, chemical nature, effects, and toxicity.
Property | Exotoxins | Endotoxins |
|---|---|---|
Bacterial Source | Gram Positive & Gram Negative Bacteria | Gram Negative Bacteria |
Location in/on Bacterium | Within cytoplasm; may or may not be secreted | Component of outer membrane |
Chemical Nature | Proteins | Lipopolysaccharide (Lipid A) |
Effect on Human Body | Affects cell functions, nerves, GI tract | Fever, weakness, aches, septic shock |
Toxicity | High | Low |
Lethal Dose | Small | Large |
Heat Stability | Inactivated by heat | Heat stable |
Ability to Form Toxoid | Yes (normally) | No |
Immune Response Damage to the Host
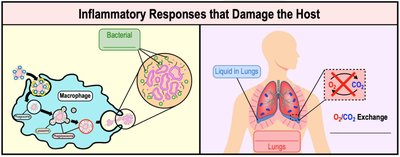
Damaging Effects of Inflammation
The inflammatory response, while protective, can cause unintended damage to host tissues. This is analogous to a sprinkler system that prevents fire but may cause water damage.
Phagocytic Cells: Release enzymes and toxic products that can damage surrounding tissues.
Delicate Systems: Inflammation in sensitive areas (e.g., meninges) can be severe or life-threatening.

Summary
Bacterial pathogenesis involves exposure, adhesion, invasion, multiplication, and host damage.
Pathogenic toxins are classified as exotoxins (A-B toxins, membrane-damaging toxins, superantigens) and endotoxins (LPS).
Exotoxins are highly toxic, protein-based, and affect specific tissues; endotoxins are less toxic, heat stable, and cause systemic effects.
Immune responses, especially inflammation, can inadvertently damage host tissues.
